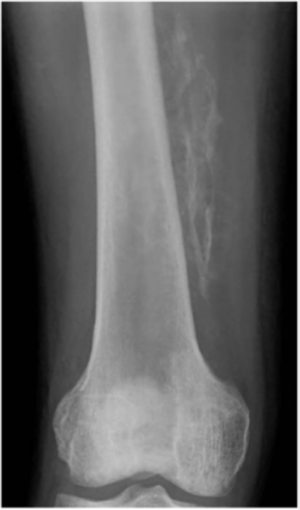
Myositis ossificans
Background
- Also known as heterotopic calcification
- Benign bone deposition within soft tissues, most often skeletal muscle.
- Usually arises secondary to trauma (either one larger traumatic event or repeated small traumas) and will generally be localized to a single muscle or group of muscles involved in the trauma.[1][2]
- Alternatively, can be generalized, widespread, progressive and unrelated to trauma - this is thought to be a hereditary form with a separate pathogenesis and treatment
- Pathophysiology not completely understood - may be related to inappropriate differentiation of mesenchymal cells into chondrocytes and osteoblasts in the setting of trauma/inflammation[3]
Clinical Features
- Length of pain out of proportion to trauma
- Decreased range of motion
- Palpable, painful mass (generally forms within 2 weeks of initial trauma)
Differential Diagnosis
Extremity trauma
- Compartment syndrome
- Contusion
- Crush syndrome
- Degloving injury
- Fracture
- Laceration
- Myositis ossificans
- Open joint injury
- Peripheral nerve injury
- Rhabdomyolysis
- Tendon injury
- Vascular injury
Evaluation
- Plain radiograph showing peripheral soft tissue calcifications
- Early radiographs may be non-diagnostic
- Biopsy may be required if concern for malignancy, calcified peritendonitis/bursitis, etc[1][4]
Management
- Generally self-limited disease process (may take up to 1 year to resolve)[1]
- Supportive care, including pain control and physical therapy, is the mainstay of treatment
Disposition
- Discharge with referral to orthopedic surgery or sports medicine[5]
See Also
External Links
References
- ↑ 1.0 1.1 1.2 Walczak BE, et al. Myositis Ossificans. J Am Acad Orthop Surg. 2015;23(10):612-22.
- ↑ Ropper AH, et al. Chapter 48. Diseases of Muscle. In: Ropper AH, Samuels MA, Klein JP. eds. Adams & Victor's Principles of Neurology, 10e. New York, NY: McGraw-Hill; 2014.
- ↑ Kan L, et al. Dysregulation of local stem/progenitor cells as a common cellular mechanism for heterotopic ossification. Stem Calls. 2009;27(1):150-156.
- ↑ Trojian TH. Muscle contusion (thigh). Clin Sports Med. 2013 Apr;32(2):317-24.
- ↑ Tintinalli JE, et al. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 8e. New York, NY: McGraw-Hill; 2016.