Murine typhus
Not to be confused with typhoid fever, a distinct disease caused by a different genera of bacteria
Background

Microscopic image of rat flea.
- Also known as "endemic typhus" and "flea-borne typhus"
- Caused by Rickettsia typhi
- Gram negative, obligate, intracellular bacterium
- Replicates in epithelial cells of flea's midgut
Types of Typhus
Multiple diseases include the word "typhus" in their description. Types include:
| Condition | Bacteria | Reservoir/vector | Notes |
|---|---|---|---|
| Epidemic "Louse-borne" typhus | Rickettsia prowazekii | Human Body louse | When the term "typhus" is used without clarification, this is usually the condition described. Historical references to "typhus" are now generally considered to be this condition. |
| Murine typhus or "endemic typhus" or "flea-borne" typhus | Rickettsia typhi | Fleas on rats | |
| Scrub typhus | Orientia tsutsugamushi | Harvest mites on humans or rodents | Unlike the two conditions above, though it has the word "typhus" in the name, it is currently usually not classified in the typhus group, but in the closely related spotted fever group. |
| Queensland tick typhus | Rickettsia australis | Ticks |
Vector
- Infection is transmitted by fleas
- Typically rat fleas
- Also Rickettsia felis (indistinguishable from R. typhi) carried by fleas on opossum and cats
- Feces containing R. typhi are deposited into wound made by flea bites
- Found in areas with large populations of urban rats
- United States
- Southern Texas
- Southern California
- Internationally: Tropical/Subtropical urban seaboard regions
- United States
- Seasonal predilection for summer months
- Texas: Spring to summer
- California: Summer to fall
Clinical Features
- Incubation period: 7-14 days
Symptoms
- Variable and non-specific
- Often presents as acute, self-limited illness, with no complications[1]
- Most Common Symptoms
- High fever
- Can last ~1 week
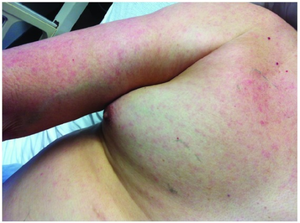
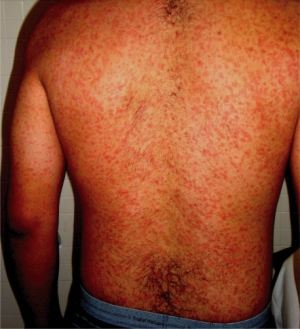
- Rash
- Macular or maculopapular, blanching, non-pruritic
- Starts centrally and moves to the extremities
- Can involve palms/soles but usually sparing
- Starts 6-7 days after symptom onset (fever onset)
- Headache
- Arthralgias
- Other Symptoms/Complications
- Hepatomegaly
- Splenomegaly
- Cough
- Diarrhea
- Nausea/Vomiting
- Abdominal pain
- Meningitis
- Endocarditis
- Rarely death (<1% of cases)
Differential Diagnosis
- Non-specific viral illness
- Most common admitting diagnosis in one case study was "fever of unknown origin"[2]
Tick Borne Illnesses
- Babesiosis
- Colorado tick fever
- Ehrlichiosis
- Heartland virus
- Lyme
- Murine typhus
- Rocky mountain spotted fever
- Southern tick-associated rash illness (STARI)
- Tick paralysis
- Tularemia
Fever in traveler
- Normal causes of acute fever!
- Malaria
- Dengue
- Leptospirosis
- Typhoid fever
- Typhus
- Viral hemorrhagic fevers
- Chikungunya
- Yellow fever
- Rift valley fever
- Q fever
- Amebiasis
- Zika virus
Evaluation
- Infectious work up
- Not sensitive or specific
- CBC- can show anemia and thrombocytopenia
- LFTs- often elevated 3-5x normal
- Lumbar puncture- resembles aseptic meningitis
Diagnostic labs
- Immunofluorescent assay is the gold standard
- Becomes diagnostic with time. Rarely positive at onset of illness.
- PCR
Management
May need to treat empirically while awaiting confirmatory testing.
- Doxycycline 100mg BID continue for 3 days after resolution of symptoms[3]
- Children - 2.2mg/kg BID
- Chloramphenicol 50-100mg/kg/day div Q6hr (Max dose = 4g/day)
Disposition
See Also
External Links
References
- ↑ Civen R, Ngo V, 2008. Murine typhus: an unrecognized suburban vectorborne disease. Clin Infect Dis 46: 913–918.
- ↑ Civen R, Ngo V, 2008. Murine typhus: an unrecognized suburban vectorborne disease. Clin Infect Dis 46: 913–918.
- ↑ Civen R, Ngo V, 2008. Murine typhus: an unrecognized suburban vectorborne disease. Clin Infect Dis 46: 913–918.