Left ventricular assist device complications
(Redirected from LVAD)
Background
- Commonly referred to as an LVAD
- Developed in 1960s as bridge to cardiac transplant
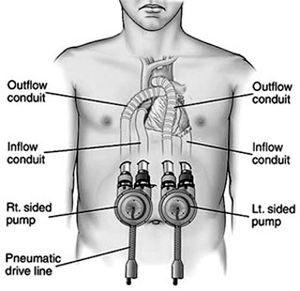
- LVAD (left ventricle), RVAD (right ventricle), BiVAD (both venticles via separate pumps)[1]
- Also used as destination therapy
- VADs have 3 major variables:
- Speed
- Flow
- Power
- Other parameters:
- Battery level - typically powered by two batteries, with power base unit that can be plugged into wall
- Pulsatility index:
- Decreased index, may indicate low preload or decreased native LV contractility
- Increased index, may indicate volume overload or increased native LV contractility
- Pump speed and pulsatility index are inversely related
Applications
- Modern applications have expanded beyond original purpose:
- Bridge to cardiac transplant
- Temporizing measure for cardiomyopathies that are expected to resolve
- Destination therapy for patients who will not undergo cardiac transplant
- Indication is New York Heart Association class 4 heart failure, ejection fraction <25%, VO2 max less than 15 among other criteria[2]
- Goal of a VAD is to assist the ventricle and augment cardiac output
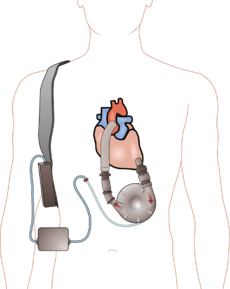
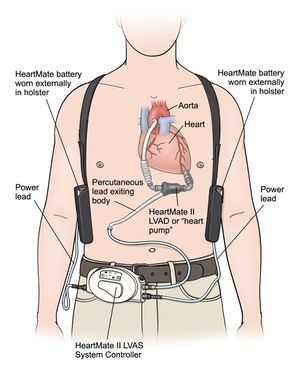
Components
- Pump = Internal pump (usually placed in preperitoneal space), takes blood from a cannula in the apex of the left ventricle and pumps it into the aorta
- Driveline = Percutaneous cable that exits the abdominal wall, connects pump to external components (controller, battery)
- Controller = External "box" containing computer for the device that monitors pump performance, has a display screen and controls for settings/alarms/diagnostics, and will display will show pump speed in RPM and pump output in L/min
- Power Supply = Controller can be connected to batteries for patient mobility, or to a "power base station" that plugs into the wall for home use
Devices Overview
HeartMate I or XVE
- Use: Destination Therapy
- Flow Type: Pulsatile
- Backup Method: Hand Pump
- Battery: 12volt MiMH - 10hrs
- Defib/Cardioversion: Use hand pump during defib/cardioversion
HeartMate II
(Most common type in use today)
- Use: Bridge to transplant or destination therapy
- Flow type: Continuous
- Backup Method: No external method
- Battery: 14V Li-Ion - 10 hrs
- Defib/Cardioversion: No precautions
- Target INR: 1.8 to 2.5
Thoratec VAD (HeartMate III)
- Use: Bridge to Transplant
- Flow Type: Pulsatile
- Backup Method: No external method
- Battery: 12V lead acid gel battery - 7.2 Ah - up to 3 hrs
- Defib/Cardioversion: No precautions
HeartWare HVAD
- Use: Bridge to Transplant
- Anatomy: Designed to be implanted completely in pericardial space, no need for pump pocket formation
- Flow Type: Centrifugal pump
- Target INR: 2.0-3.0
Complications/Differential Diagnosis[3]
- Bleeding - most common reason for ED visit, most common in first month after implant (frequency 42%[4])
- GI bleeding is the most common source (15%-30%) followed by epistaxis.[5]
- Mechanisms:
- Acquired Von Willebrand Disease (vWD) from pump shear forces[6]
- supratherapeutic anticoagulation
- Lack of pulsatile flow → AV malformations in GI tract
- Passive hepatic congestion secondary to biventricular failure, predisoposing to bleeding
- Shear forces from device itself can lead to hemolytic anemia[7]
- Immediately consult VAD team/coordinator
- Treatment - anticoagulant reversal based on specific agents used
- In life-threatening bleeds, consider TXA, PCC, Desmopressin, FFP
- Warfarin reversal carries low risk for acute thrombosis [8]
- Infection - driveline and pocket are most common sites[4]
- Usually gram positive bacteria, but also need to cover for fungal infection
- Pump Thrombosis, estimated at 2-13%, average first thrombosis ~1 year after implant depending on device[9]
- Low output state with falsely elevated pump flow estimates on controller
- Diagnose with echo or cardiac CTA
- Treatment with heparin and antiplatelet therapy
- Consider tPA in life-threatening situations
- Causes:
- Mechanical - post-surgical ventricular debris, cardiac emboli, inflow cannula malposition
- Inadequate anticoagulation and/or antiplatelet treatment
- As optimal dosing and monitoring not well defined due to lack of clinical trials
- Will occur despite rigid regimen and compliance of anticoagulation/antiplatelet
- Prosthetic material inflammatory reaction with blood
- Intrinsic endothelial activation in response to continuous flow-VAD
- Arrhythmia - very common
- Get labs to evaluate electrolytes and troponin
- Treat atrial fibrillation as in any other patient
- Treat ventricular arrhythmias with volume replacement and pharmacological or electrical cardioversion
- Place pads anterior/posterior if going to cardiovert/defibrillate
- "Suction event"
- Pump pulls from an LV that hasn't filled
- Causes:
- Cannula malposition
- Increased peripheral vascular resistance (hypertensive emergency)
- Tamponade
Evaluation[3]
- Assess perfusion and general state (mental status, skin temp/color, capillary refill, etc)
- LVADs are preload dependant - if symptoms of hypoperfusion, give fluid blous
- HR measured via ECG or auscultation (may be difficult secondary to pump noise). A hum or whir should be present to indicate the pump is functioning.
- Get 12-lead ECG on all LVAD patients
- Demonstrates primary cardiac disease[10]
- Generally, VAD does not influence underlying cardiac rhythm
- Imaging:
- Bedside echo if able, formal echo if available, with the following suggestive of thrombosis:
- Cannula flow velocity > 2 m/s
- More frequent opening of aortic valve than at baseline
- Increasing LV internal dimension in diastole without manual speed changes
- CT with contrast to look for thrombus, discuss with radiologist to protocol
- Bedside echo if able, formal echo if available, with the following suggestive of thrombosis:
- Blood pressure measured with manual BP cuff and Doppler ultrasound - MAP is identified when constant flow is heard
- MAP should be 65-80 mmHg[11]
- Can also monitor with arterial line
- Basic lab should be obtained on all LVAD patients
- Cardiac labs - BNP, troponin
- Include thrombolysis, coagulopathy labs
- LDH elevation over 1,150 IU/L suggestive of pump thrombosis[12]
- Approximate sensitivity of ~80% and specificity of 90%
- Hemolysis within thrombosed pump releases LDH
- Assess LVAD status
- Auscultate for pump noise
- Device parameters (found on controller)
- Pump speed - varies by device - 2,000-10,000 RPM
- Power - normal 4-6 Watts
- Flow - normal 4-6 L/min
- Pulsatility Index (PI) - normal 1-10
- Measures magnitude of pulsatile flow provided by native cardiac contractions
- Higher PI = less LVAD support
- Clinical status more important than LVAD parameters
- If hypotension, consider VAD flows
- Low VAD flow
- Low JVP - bleeding, hypovolemia
- High JVP - RV dysfunction, inadequate unloading, PE, PTX, tamponade
- High VAD flows - vasodilatation (sepsis, vasoactive medications)
- Low VAD flow
Management
- Immediately contact hospital or patient's LVAD coordinator to help coordinate care
- Check controller to ensure power light is on
- Ensure humming sound of pump is auscultated over chest/abdomen
- If pump not working, replace with patient's backup controller
- Check all connections to power source, driveline, and controller are intact
- Disconnect all connections after checking, and reconnect immediately
- Inspect driveline for damages/defects
- Assess battery, replace with backup battery
- Patient should be positioned flat on stretcher before replacing battery
- OR connect to hospital's power base unit or patient's power base unit if available
- IF NONE OF ABOVE, contact VAD coordinator to find local LVAD patient in vicinity willing to transport extra batteries to ED
- Take note that if battery is critically low, many devices will automatically lower speed, which can cause syncope or lightheadedness
- Hemodynamic, supportive care[13]
- Many LVAD patients fluid restrict too much due to their history, and LVADs are preload dependent
- IVF crystalloid fluid bolus when indicated (low-flow indicator alarm)
- MAP goal 70-90 mmHg
- LVAD patients afterload sensitive
- Address high BP emergently if thought to contribute to increased work of pump, which leads to thrombus and stroke
- Beware of suction event complication, which requires IVF bolus and allowing the controller to sense this, slow pump speed and slowly bring up to fixed speed to allow for adequate ventricular filling
- Take special care to not twist, bend, cut, or otherwise damage the driveline
- First generation LVADs had pulsatile flow
- Subsequent designs use continuous flow - patient will not have a palpable pulse
- Patient will be on anticoagulation and antiplatelet therapy secondary to high risk of pump thrombus, CVA, and other thromboembolic events
- VADs are ECG independant, unlike ICD (many patients with a VAD will also have an ICD in place)
- ICD discharges are common, and frequently inappropriate (possibly secondary to LVAD interference)[10]
- Ensure that patient or family bring in any additional batteries and charging elements as these will not be available in most hospital settings
- Thrombosis, tPA in emergencies
- Breadth of literature supporting is overall small
- When patient not responding to continuous anticoagulation (heparin, argatroban drip)
- AND when going directly to LVAD exchange or catheter-directed thrombolysis are not possibilities
- Consider tPA if not contraindicated for survival and avoidance of needing LVAD exhange[14]
- 5 mg IV bolus tPA
- 3 mg/hr infusion in NS for 10 hours
- 1 mg/hr for up to 48 hours, never exceeding 100 mg max total dosage
- In single center study cited above, there was:
- 70% that had hemolysis resolve and no need for LVAD exchange at 30 days
- 95% survival at 30 days
- 10% hemorrhagic stroke with no difference between tPA and control group
- Alternative dosing, while plus/minus continuing heparin drip[15]
- Initial dosing of 10 mg IV bolus
- Followed by 1 mg/min for 20 min
- Then 1 mg/hr for 24 hours
- Monitor LDH levels and discontinue heparin drip when LDH acceptably lowered
Cardiac Arrest[3]
- Unconscious, apneic, no evidence of LVAD function (auscultate for mechanical noise)
- Immediately evaluate LVAD components and attach to reliable power source
- Some first-generation LVADs have external hand pumps that can be used to provide circulation
- Begin CPR if patient is unresponsive with MAP less than 50mmHg, end tidal carbon dioxide level less than 20mmHg, or LVAD cannot be restarted.[16]
- Unstable patients with shockable dysrhythmias should be cardioverted.[17]
- Optimal placement of pads is in the anterior-posterior fashion & not over the drive line.
- Patient can be intubated, given IV fluids and ACLS drugs, etc
- Unstable patients with shockable dysrhythmias should be cardioverted.[17]
- New Paradigm shift with since AHA officially endorsed the use of chest compressions in 6/2017.[18]
Disposition
- Immediately contact the patient's VAD coordinator
- Almost all LVAD patient presenting to the ED will require admission or transfer to a site of expertise
See Also
External Links
- VAD Review
- EMCrit LVAD Management
- MyLVAD OR Mechanical Circulatory Support Organization EMS Guide
- CriticalCareNow: Simplified Algorithm for ACLS in LVAD Patients
References
- ↑ Mechem CC. Prehospital assessment and management of patients with ventricular-assist devices. Prehosp Emerg Care. 2013 Apr-Jun;17(2):223-9.
- ↑ Mancini D, Lietz K. Selection of cardiac transplantation candidates in 2010. Circulation. 2010;122(2):173-83.
- ↑ 3.0 3.1 3.2 Partyka C, Taylor B. Review article: ventricular assist devices in the emergency department. Emerg Med Australas. 2014 Apr;26(2):104-12.
- ↑ 4.0 4.1 Rose EA, Gelijns AC, Moskowitz AJ et al. Long-term use of a left ventricular assist device for end-stage heart failure. N. Engl. J. Med. 2001; 345: 1435–1443.
- ↑ Stenberg, R., & Shenvi, C. (2020). Targeted Evaluation of Patients With Left Ventricular Assist Devices and Shock or Hypotension. Annals of Emergency Medicine, 76(1), 34–41. https://doi.org/10.1016/j.annemergmed.2020.01.003
- ↑ Suarez J., Patel C.B., Felker G.M., Becker R., Hernandez A.F., Rogers J.G. Mechanisms of bleeding and approach to patients with axial-flow left ventricular assist devices. Circ Heart Fail. 2011;4:770–784.
- ↑ Jennings DL, Williams CT, Morgan JA. Pentoxifylline for the treatment of hemolytic anemia in a patient who developed recurrent gastrointestinal bleeding while on continuous-flow left ventricular assist device support. ASAIO J. 2013;59(5):526-527. doi:10.1097/MAT.0b013e31829f0eb1
- ↑ Jennings, D, et al. Safety of Anticoagulation Reversal in Patients Supported with Continuous-Flow Left Ventricular Assist Devices. ASAIO Journal. July 2014. 60:381–384
- ↑ Nair N et al. Thrombolytics in VAD management — A single-center experience. Int J Cardiol Heart Vasc. 2016 Jun; 11: 49–54.
- ↑ 10.0 10.1 Pistono M, Corrà U, Gnemmi M, Imparato A, Temporelli PL, Tarro Genta F, Giannuzzi P. How to face emergencies in heart failure patients with ventricular assist device. Int J Cardiol. 2013 Oct 15;168(6):5143-8
- ↑ Stenberg, R., & Shenvi, C. (2020). Targeted Evaluation of Patients With Left Ventricular Assist Devices and Shock or Hypotension. Annals of Emergency Medicine, 76(1), 34–41. https://doi.org/10.1016/j.annemergmed.2020.01.003
- ↑ Zoler ML. Cardiology News. STS: Lactate dehydrogenase of 1,150 IU/L flags LVAD thrombosis. https://www.mdedge.com/ecardiologynews/article/106621/heart-failure/sts-lactate-dehydrogenase-1150-iu/l-flags-lvad. Published Feb 19, 2016.
- ↑ Troubleshooting the Left Ventricular Assist Device. Emergency Medicine. 2016 February;48(2):58-63.
- ↑ Nair N et al. Thrombolytics in VAD management — A single-center experience. Int J Cardiol Heart Vasc. 2016 Jun; 11: 49–54.
- ↑ Webber BT et al. Intravenous thrombolytic therapy for patients with ventricular assist device thrombosis: An attempt to avoid reoperation. Ann Card Anaesth. 2016 Jan-Mar; 19(1): 192–196.
- ↑ Stenberg, R., & Shenvi, C. (2020). Targeted Evaluation of Patients With Left Ventricular Assist Devices and Shock or Hypotension. Annals of Emergency Medicine, 76(1), 34–41. https://doi.org/10.1016/j.annemergmed.2020.01.003
- ↑ Stenberg, R., & Shenvi, C. (2020). Targeted Evaluation of Patients With Left Ventricular Assist Devices and Shock or Hypotension. Annals of Emergency Medicine, 76(1), 34–41. https://doi.org/10.1016/j.annemergmed.2020.01.003
- ↑ Stenberg, R., & Shenvi, C. (2020). Targeted Evaluation of Patients With Left Ventricular Assist Devices and Shock or Hypotension. Annals of Emergency Medicine, 76(1), 34–41. https://doi.org/10.1016/j.annemergmed.2020.01.003
- ↑ Shinar Z, Bellezzo J, Stahovich M, Cheskes S, Chillcott S, Dembitsky W. Chest compressions may be safe in arresting patients with left ventricular assist devices (LVADs). Resuscitation. 2014 May;85(5):702-4.
- ↑ Mabvuure NT, Rodrigues JN. External cardiac compression during cardiopulmonary resuscitation of patients with left ventricular assist devices. Interact Cardiovasc Thorac Surg. 2014 Aug;19(2):286-9.
- ↑ Eric M Rottenberg, Jarrett Heard, Robert Hamlin, Benjamin C Sun, and Hamdy Awad. Abdominal only CPR during cardiac arrest for a patient with an LVAD during resternotomy: A case report. J Cardiothorac Surg. 2011; 6: 91.