ITP in Pregnancy
See also ITP main page or Immune thrombocytopenic purpura (peds) for pediatric patients.
Background
- Marked diff between maternal and fetal platelet counts
- No antenatal measures predict fetal status
- Maternal response to medicine does not guarantee a favorable outcome for baby
- Only previous neonatal outcomes provide predictor of neonatal platelet counts.
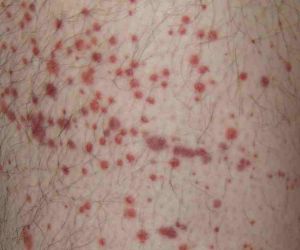
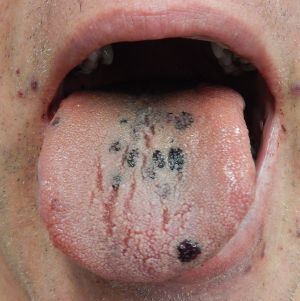
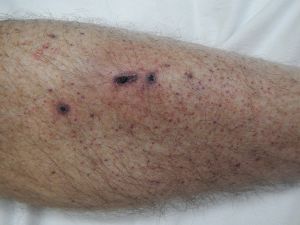
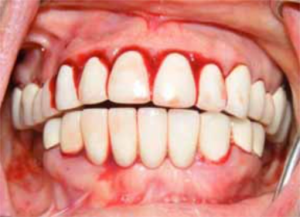
Clinical Features
- Thrombocytopenia during pregnancy
Differential Diagnosis
Thrombocytopenia
Decreased production
- Marrow infiltration (tumor or infection)
- Viral infections (rubella, HIV)
- Marrow suppression (commonly chemotherapy or radiation)
- Congenital thrombocytopenia
- Fanconi anemia
- Alport syndrome
- Bernand Soulier
- Vitamin B12 and/or folate deficiency
Increased platelet destruction or use
- Idiopathic thrombocytopenic purpura
- Thrombotic Thrombocytopenic Purpura (TTP)
- Hemolytic Uremic Syndrome (HUS)
- Disseminated Intravascular Coagulation (DIC)
- Viral infections (HIV, mumps, varicella, EBV)
- Drugs (heparin, protamine)
- Postransfusion or Posttransplantation
- Autoimmune destruction (SLE or Sarcoidosis)
- Mechanical destruction
- Artificial valves
- ECMO
- HELLP syndrome
- Excessive hemorrhage
- Hemodialysis, extracorporeal circulation
- Splenic Sequestration
- Occurs in Sickle cell disease and Cirrhosis
Drug Induced
- sulfa antibiotics, ETOH, ASA, thiazide diuretics/furosemide
Comparison by Etiology
| ITP | TTP | HUS | HIT | DIC | |
|---|---|---|---|---|---|
| ↓ PLT | Yes | Yes | Yes | Yes | Yes |
| ↑PT/INR | No | No | No | +/- | Yes |
| MAHA | No | Yes | Yes | No | Yes |
| ↓ Fibrinogen | No | No | No | No | Yes |
| Ok to give PLT | Yes | No | No | No | Yes |
Evaluation
- Usually mild thrombocytopenia (>70k)
- Platelet count normalizes after delivery
Management
- Balance risk of thrombocytopenia (for mother and fetus/baby) vs potential teratogenesis from therapy
- Treatment indicated if[1]:
- Platelets <10,000
- Platelets <30,000 and bleeding or in 2nd or 3rd trimester
- Risk of prednisone or IVIG outweighed by benefits in above situations[2]
- Infant has slightly increased risk of ICH with v low risk of ICH- but higher of normal baby
- role of cesarean in preventing ICH controversial
- If baby has platelets <30k; IVIG and or prednisone
- No contraindication to breastfeeding.
See Also
References
- ↑ Stavrou E, Mccrae KR. Immune thrombocytopenia in pregnancy. Hematol Oncol Clin North Am. 2009;23(6):1299-316.
- ↑ https://www.ouh.nhs.uk/patient-guide/leaflets/files/13880Pitp.pdf