Harbor:ED policy manual
Harbor-UCLA Medical Center Emergency Department Policy Manual
- This reference is intended only for quick reference and these listed DEM policies and protocols MAY NOT BE COMPLETE OR UP TO DATE.
- All policies listed here are in addition to and NOT in place of Harbor-UCLA and DHS policies.
- To access Harbor-UCLA Medical Center Policies and Procedures, you must be log into the internal Harbor-UCLA Medical Center sharepoint site.
- Internal home page
- Select Policies & Procedures
- Select Harbor-UCLA Medical Center.
ED Care
#1: Provision of Care
POLICY
- The Department of Emergency Medicine (DEM) is part of a Level I Trauma and ST Elevation Myocardial Infarction (STEMI) Receiving Center that provides diagnostic and therapeutic services for unforeseen physical and mental disorders which, if not properly treated, could lead to marked suffering, disability, or death.
- Scope of Services
- Basic emergency medical services for all patients (in accordance with the California Code of Regulations, Title 22).
- Level 1 Trauma Center
- STEMI Receiving Center
- Pediatric Medical Center
- Patient Intake - All patients will recieve MSE on arrival.
- After initiation of the MSE are cared for in one of the following areas: Adult ED (AED), Adult Fast Track, Pediatric ED (PED), Adult Psychiatric ED, Adolescent Psychiatric ED, Medicine Urgent Care Clinic (UCC), Gynecology Urgent Care Clinic, or Labor and Delivery.
- DEM services provided include:
- Provision of an MSE to ALL patients.
- Provision of immediate evaluation, stabilization and disposition of patients who present with emergent medical, surgical, gynecologic, or behavioral problems (when active medical issues are present).
- Patients requiring services that cannot be provided at Harbor-UCLA are transferred to appropriate healthcare facilities following initial stabilization.
- As resources allow, provision of timely evaluation, treatment and disposition of patients who present with urgent and non-urgent medical, surgical, gynecologic, or behavioral problems.
- Provision of medical direction and consultation for field units of the Los Angeles County Emergency Medical Services Agency, as well as staff for the Hospital Emergency Response Team.
- Referral of patients that are not admitted to inpatient services to appropriate primary care and specialty resources that will provide ongoing medical care for stabilized medical conditions and chronic diseases.
- Disaster Resource Center (DRC)
- DEM serves as the DRC for the South Bay Area of Los Angeles
- Responsibilities include: provides around-the-clock mass decontamination capability, stores resources and medications necessary to augment hospital response in the event of mass-casualty disasters, provides guidance in dis-aster preparedness to umbrella hospitals in the South Bay and disaster preparedness education to a wide variety of audiences, and maintains a network linking Harbor-UCLA Medical Center to local public safety agencies, umbrella facilities and the Los Angeles County EMS Agency.
- Department Goals
- Patient Flow
- Overall LOS (AED<8.2hrs, PED<5.5hrs)
- DC LOS (AED<5.6, PED<2.5)
- LOS for mid to low-acuity (ESI 3<7 hrs, ESI 4&5 <3 hrs)
- Provider to decision provider productivity (<2 hrs)
- Consult TAT (<2 hours)
- Maintain the amount of time ambulance patients spend waiting to be offloaded (Metric - EMS Wall Time. Goal: 30 m)
- Patient Safety
- Maintain our left without being seen rate (< 2%)
- Reduce LBTC (<8.6%)
- Maintain door to EKG time (<10 min)
- Maintain electronic prescription for controlled substances to reduce narcotic diversion
- Standardize TeamSTEPPs shift briefing, debriefing and huddles to improve care team communication
- Patient Experience
- Maintain pain reassessment after administration of analgesics per hospital policy (>90%)
- Employee Satisfaction
- Staff shifts to patient demand, adjust working hours/shifts based on feedback from employees where possible, including nurse practitioners and emergency medicine residents
- Revise and disseminate a follow-up staff satisfaction survey. (Goal: 10% improvement over baseline)
- Continue LEAN Visual Management Boards in all care areas to engage employees in performance improvement initiatives, solicit their input on processes, and enhance employee communication
- Performance Improvement
- Track and improve performance on timely administration of antibiotics to patients with open long bone fractures
- Track and improve performance on compliance with ultrasound image uploading for trauma patients
- Implementation of Code Stroke program with the development of specific QI using metrics and case review
- Continued efforts to improve hospital-wide core measures specific to the emergency department
- Financial Performance
- Continue lab and test follow-up functions to reduce the load on the Continuing Care Clinic.
- Audit and provide feedback on the appropriate placement of patients in the observation area (with regards to insurance and placement status)
- Repatriating Out of Plan patients to their home health network.
- Ambulatory Care
- Revised clerk clinic scheduling process for smoother discharges
- Develop a facilitated process for DHS eligible patients presenting to the emergency department solely for specialist follow-up
- Overall LOS (AED<8.2hrs, PED<5.5hrs)
- Patient Flow
- Quality Management Program
- The quality of medical care provided in the DEM is reviewed and evaluated, in a systematic and ongoing fashion, by the ED Quality Improvement Committee and the ED Community Council. These multi-disciplinary committees review the following.
- DEM statistics and trends, including patient volume, length of stay for admitted and discharged patients, left without being seen and left before treatment complete rates, and critical wait time (time the most acute patients wait to see a physician)
- Cases reviewed from outside departments, hospital committees or individual physicians. Case reviews are done in a timely fashion by tracking overall turnaround and volume
- Paramedic base station radio communications and field operations
- Reports regarding patient and staff safety, patient relations, hospital staff relations, and patient care, including responding in a timely manner to patient and insurance plan concerns forwarded to the department.
- The quality of medical care provided in the DEM is reviewed and evaluated, in a systematic and ongoing fashion, by the ED Quality Improvement Committee and the ED Community Council. These multi-disciplinary committees review the following.
#8 Invasive Procedures
Policy
- Invasive procedures will be performed by, or under the supervision of, an appropriately credentialed provider. A list of approved ED physicians (faculty and residents) for each procedure will be available and updated on a periodic basis.
- The decision to perform an invasive procedure will be made after an assessment of the patient's history, physical examination, a review of available diagnostic data, an assessment of the risks and benefits of the procedure, and an assessment of the need to administer blood or blood products. Appropriate precautions, clothing, and equipment will be used as indicated for the procedure.
- When possible, the patient will be informed of the procedure, risks, benefits, alternatives to the procedure, and need for or risk of blood transfusion. If the patient or their parent or guarding (in the case of minors) agrees to the procedure, the patient or parent/guardian will sign an informed consent form for the specific invasive procedure.
- In many critical situations, emergent procedures may be necessary when informed consent may not be possible. In such circumstances, the physician will attempt to obtain verbal consent, which will cover procedures performed in the ED on an emergency basis (e.g., when the patient is critically ill and unable to sign the consent form or when a parent/guardian is not available).
- Patients will be appropriately monitored during and after all procedures as per general guidelines of the hospital and the ED. Harbor-UCLA Policy 355' should be followed for any patients requiring procedural sedation.
- Performance of all procedures in the ED, the patient's response, and complications of the procedure will be documented in the medical record.
#10 Authorization for ED Treatment
Policy
- Authorization for treatment of patients presenting to the ED is obtained in one or more of the following ways:
- General Consent
- Adult patients (aged 18 years or older) who present to the ED for care will be asked to read and sign a General Consent form at the time of registration. This form grants consent to ED staff (providers and nurses) to take a medical history, perform a physical examination, order routine diagnostic tests (e.g., blood tests, urinalysis, x-rays, etc.), and initiate basic treatment as well as perform simple procedures (e.g.,. administration of intravenous fluids, laceration repair, incision and drainage of abscesses, etc.).
- Informed Consent
- Specific Informed Consent will be obtained for additional tests and procedures that are: (1) complex (as defined by Harbor-UCLA Policy 604A), (2) associated with significant complications or side effects, (3) performed for the purpose of an Institutional Review Board approved research study, (4) when alternative tests or treatments are available.
- Emergency Consent
- In the case of a medical emergency, treatment may proceed without a patient’s consent so long as no evidence exists to indicate that the patient, or the patient’s legal representative, would refuse the treatment. When the emergency exception rule is invoked, there should be clear documentation as to the rationale for the emergency intervention that was required. Treatment exceeding that needed for the emergency condition will not be rendered without patient consent.
- Patients Lacking Capacity to Provide Consent
- Emergency medical treatment for patients who lack the capacity to provide consent will be rendered in compliance with Harbor-UCLA Policy 620.
- Simple and Complex Procedures
- Examples of “simple” basic procedures covered by general patient care consent include (but are not limited to): Phlebotomy, Peripheral venous access, Bedside ultrasound, Incision and drainage of abscess, and Laceration repair (suture, staple, or adhesive).
- Examples of “complex” invasive procedures requiring specific informed consent include but are not limited to (see Harbor-UCLA Policy 604A, Appendix B for a comprehensive set; below is a list of common ED procedures requiring consent): Blood transfusion, Procedural sedation, Elective cardioversion, Central vein catheterization, Lumbar puncture, Paracentesis, and Thoracentesis or non-emergent thoracostomy.
#15 Death Notification From the ED (Family of Deceased)
POLICY
- When a patient dies in the Emergency Department, it is the duty of the provider responsible for the patient’s care in the ED to notify the patient’s family, and the patient’s private physician, when known and appropriate. This notification should be documented in the patient’s electronic medical record.
- If the patient’s family cannot be located, Social Work should be contacted to assist in locating the family so the provider may notify them of the death.
- It is recommended that families be notified in person. The family should be informed that their family member has come to the Emergency Department in critical condition and that the family should come immediately. When the family member(s) arrive, they should promptly be directed to the Family Room. Social work should accompany the ED provider during the death notification process whenever possible and be available for supportive counseling. The Los Angeles Sheriff’s Department should be contacted for violent traumatic deaths as soon as appropriate after the family arrives. Refer to Harbor-UCLA Policy 140 (Decedent Viewing) when there is a criminal investigation.
- Family members who are unable to come in person should be informed of the patient’s death over the phone in a compassionate manner. In doing so, the physician should make sure that the family:
- Has a chance to ask all their questions,
- Is given a contact person (physician name and ED phone number – 424-306-5001) in case they have further questions, and
- Is informed that they can contact the Decedent Affairs Office at Harbor-UCLA (424.306.4034) to discuss the process for release of the body.
#16 Discharge Process
POLICY
- All patients discharged home will have appropriate follow-up care plan discussed with the patient prior to discharge. No patient will be discharged without attempting to obtain a reasonable follow-up plan for that patient. The condition of the patient at the time of discharge is to be documented on the chart.
Protocol:
- Document vital signs within 2 hours of discharge or at the time of discharge if previously abnormal.
- DEM provider to complete documentation in electronic medical record.
- Verify all orders have been carried out and signed off (nursing staff).
- DEM physician to complete documentation of aftercare plan and discharge instructions, and print out copy for patient
- Discuss after care plan with patient and/or appropriate responsible parties.
- Obtain patient signature or verbal consent (or responsible guardian) on discharge instructions, witnessed by discharging personnel.
- Give copy of after care plan, specific instruction forms and prescriptions as indicated to patient.
- Return all personal belongings.
- Document time of discharge.
#17 Provision of Disability from the ED
POLICY
- Disability will not be given to emergency department patients by ED staff. Patients requesting disability will be referred to a long-term care provider (at Harbor-UCLA Medical Center or in the community). Patients who have been followed in the Harbor-UCLA Medical Center Clinics may be referred to the Medical Records Department (daytime, Monday – Friday) to determine if the medical record contains sufficient documentation to complete the disability forms.
- Short-term time off (< one week) or limited duty (< one week) may be given by the emergency physician to a patient with an acute problem needing short-term restricted activities. To give limited time off or restricted activity, the emergency physician is to write for the specific restricted activity and duration of time in the discharge-related documentation in the electronic medical record (eg. Off work 2 days; strict bed rest 2 days; no lifting >15# for 5 days). The patient is to be given a copy of their discharge paperwork at time of ED discharge.
- In the setting of infectious diseases requiring a period of quarantine, CDC guidelines should be followed for prescription of time off work/school.
#18 Supervision of House Staff and Medical Students
POLICY
- Refer to Harbor UCLA Policy 622a.
- Medical Students
- Medical students may perform histories, physical examinations and procedures with appropriate supervision. All medical orders require co-signature by a licensed physician. Medical students are supervised at all times by the residents and faculty assigned to the DEM. All charts by medical students must be cosigned by a licensed physician and reviewed by the senior Emergency Medicine resident or faculty member.
#19 Approval of DEM House Staff in Performance of Invasive Procedures
POLICY
- DEM housestaff are initially allowed to perform specified procedures only under the direct supervision of DEM faculty or other housestaff who have already been approved in the performance of those procedures. Once residents have been approved for a certain procedure, they can perform the procedure independently, with indirect supervision of faculty.
- The following is a list of the procedures that are covered by this policy, including the number of times each procedure must be performed under direct supervision before a resident can be approved in that procedure:
- The following procedure will be used to privilege DEM housestaff in the performance of specified procedures:
- When a resident performs a procedure he/she will fill out a procedure note in the electronic health record (and in a separate electronic log when at outside rotations), which identifies the patient, the procedure performed and the supervising physician.
- Intermittently, each resident will be provided with feedback regarding the number of procedures they have performed. This feedback will note the procedures they are currently credentialed to perform independently.
- This will be posted for reference on the Harbor-UCLA intranet homepage (Clinical --> Applications -> iPrivileges/Resident Competencies).
#20 Transition of Care
POLICY
- ED patients: All transitions of care for patients occur during rounds. Rounds occur 3 times a day between 8-hours shifts with overlap. Rounds are staggered so that there is not a complete change of providers at any given time. Most patients are seen and discharged or admitted during one shift. There are no more than 3 transitions in a 24-hour period. Patients who are signed out to an oncoming team are assigned a new provider on the electronic health record (EHR) and the providers communicate two identifiers (typically name and MRN#), current clinical condition, what has been done for the patient, any tests, tasks or consults that require follow-up, and a working diagnosis when appropriate. Rounds are supervised by an Emergency Medicine attending physician.
- Admissions: See Harbor-UCLA Policy 312.
#22 Medication Refills
POLICY
- Medications will only be refilled for registered ED patients. Unregistered patients will be referred to their primary care provider for refills.
- For psychiatric medication refills, referral can be made to the Psychiatric ED or Exodus.
#23 Family Presence During Procedures
POLICY
- Due to the unique setting of the Emergency Department, the decision to permit visitation is at the discretion of the Emergency Department staff. Visitation may be restricted in an emergency situation and/or any active or potential hospital safety situation.
- In accordance with Harbor-UCLA Policy 109A, each patient has the right to designate visitors of his/her choosing with the following exceptions:
- Staff safety needs to be maintained at all times;
- Staff needs to be able to perform their duties with minimal interference from visitors;
- When no visitors are allowed
- The patient has notified the healthcare provider that he/she no longer wants a particular person to visit;
- No more than one visitor at the bedside unless approved by DEM staff; or
- Visitors must remain inside the patient’s room. Visitors will not be allowed to stand in the hallways.
- In some instances, it may be beneficial to allow a family member or support person to be present while a procedure is being performed at the discretion of ED staff. This usually relates to a parent/guardian of a child, caregiver, or support person who can enhance the patient cooperation interaction experience.
- A chair should be provided for all family members who are present during a procedure/resuscitation for their own safety.
- Prior to a family member entering the resuscitation area, a staff member will notify the team that the family has arrived/present.
- Offer the family simple comforts such as a phone, tissues, water, restroom access, and clergy.
- As much as possible, a staff member (MD, NP, RN, LCSW) will accompany and explain to the family members the following:
- What they are about to see.
- They can leave the room at any time.
- They may be asked to leave the room at any time for a variety of reasons
- While we understand that they may become emotional and we support. their feelings, they must not interfere with medical treatment.
- In the event of patient death:
- Department of Social Services or nursing should provide the family with a copy of the Harbor UCLA Medical Center Bereavement Packet with information on funeral homes, community support groups, and information concerning the disposition of the body.
- For pediatric deaths, nursing may offer the family a lock of hair, a hand or foot print when possible.
- Provide the family with the telephone number to the ED for any questions they may have after returning home.
#29 Spinal Cord Injury
POLICY
- When a potentially unstable spinal cord injury (SCI) is identified, procedures will be taken to immediately immobilize the spine and ensure that all staff caring for the patient in the Emergency Department (ED) are aware and maintain this strict immobilization. Appropriate specialists are consulted to make timely decisions on the best intervention and disposition for the individual patient. If these precautions are no longer needed, then can be discontinued.
Protocol
- Patients identified by the provider as potentially having an unstable spinal cord injury will be immobilized immediately by the most appropriate means (c-collar, sandbags, lying flat, logroll with staff assistance, etc.) to maintain strict alignment should the patient move or need to be moved.
- The Department of Emergency Medicine (DEM) resident or attending physician will notify nursing and clinical staff of the patient's injury.
- The DEM resident or attending physician will place an order for “high risk spine precautions” in the electronic medical record.
- The nurse will place a high-visibility "High Risk Spine Precautions” sticker on the patient's c-collar and gurney. These stickers are located in the Trauma clerk station.
- When the injury is confirmed after CT imaging, the DEM resident or attending will consult Neurosurgery team and the Trauma Surgery team if not already involved.
- ED attending will communicate the concern or diagnosis of Spinal Cord Injury (SCI) to Trauma attending and ensure a prompt neurosurgical consultation.
- A physician must accompany the patient for transport to and from MRI to assist in maintaining c-spine and full spinal alignment during the physical transfer.
- Patients with unstable SCIs will be prioritized for transfer from the DEM to an inpatient ICU bed.
- Neurological status will be assessed a minimum of every 2 hours or per neurosurgery recommendations
Family and Next-of-Kin (#17 NOTIFICATIONS & REPORTING, Policy 17.1)
- All attempts will be made to notify family or legal guardians whenever possible and as soon as possible when a minor presents or is brought to the emergency room. However, these attempts will not delay emergent care when an emergency medical condition exists. Additionally, the family or next-of-kin of adult patients will be notified at the patient’s request.
- In the event of a critical patient or patient death Social Services will be contacted to assist with family notification.
- All attempts to notify family and next of kin should be documented on the patient’s health record.
Triage
#7 Scope of Assessment
Policy
- Patients are initially assessed in triage for the severity of their complaint, where they will also be seen by a provider to initiate the Medical Screening Exam (MSE). ESI Triage guidelines are utilized to ensure standardization of care. Patients are seen in the patient care areas in the order of their triage acuity and ED capacity. Patients in the waiting area are reassessed on a regular basis and treated as their current condition requires.
- When patients are brought into the patient care areas of the ED, they are assessed by the physicians, nurses, and other members of the emergency health care team, and individualized care and treatment goals are identified. A care plan personalized to each patient’s needs and available resources is developed, approved by the senior physicians in the ED, discussed with the patient, and enacted. Initial evaluation and treatment is provided. Senior physicians in the ED are defined as the emergency medicine attendings and senior emergency medicine residents (PGY-3 or 4). Emergency department nurse practitioners may also develop and approve care plans within their independent scope or in consultation with an emergency medicine senior physician when necessary.
- Patients are admitted to the hospital per the Harbor-UCLA Policy 312' (Emergency Department Admission Process), transferred, or discharged from the ED after appropriate treatment as per the patient's care plan.
- The assessment, findings, results, consultations, care plan, and emergency department course are documented in the patient's medical record (see DEM Policy 12.1).
- Per Harbor-UCLA Policy 370, Emergency medicine attendings have admitting privileges to all hospital inpatient services. Once an admission decision has been made by the admitting team or by the emergency medicine attending, a handoff conversation has taken place between the emergency medicine provider and the admitting team, and the “Request for Admit” order is placed, the official responsibility for the care of that patient is transferred from the emergency medicine attending physician to the attending physician for the admitting service. Patient care by ED nursing and ancillary services is continued per the patient’s individual care plan made by the primary admitting team until the patient physically leaves the emergency department. If after the admission decision and transfer of care to the admitting service, the patient is physically still in the emergency department and becomes clinically unstable, emergency patient care will be provided by the emergency medicine physicians.
#9 ED Respiratory Illness Protocol
Policy
- Triage
- Patients presenting to the initial intake window with symptoms consistent with an illness transmitted by respiratory droplets will be instructed to wear a surgical mask.
- If during the nursing triage interview a patient who is not currently masked is found to have symptoms consistent with a respiratory illness, they will also be instructed to wear a surgical mask and placed in droplet precautions. Respiratory isolation patients (RIPT) will likewise be placed in a mask per current protocol as well as airborne precautions.
- Any patient placed in a mask for any reason, must continue wearing that mask until cleared from all respiratory precautions by an ED provider.
- At the time of vital sign checks, triage nurses will check to ensure that patient’s masks are not soiled or moist. Soiled or moist masks will be replaced with a fresh mask.
- ED
- Any additional patients who are not currently masked but found to have symptoms consistent with a respiratory illness will be instructed to wear a surgical mask and placed in droplet precautions.
- Patients with fever and a clear alternative diagnosis (e.g., peritonsillar abscess, appendicitis, etc.) may have their masks discontinued at the discretion of the ED provider.
- In general, patients with respiratory symptoms should remain in droplet precautions.
- When a patient is placed in droplet precautions, the door to the room may remain open, and health care workers and visitors need to wear masks within 3 feet of the patient. Patients moving about the hospital or in crowded areas of the hospital away from a private room should wear a mask.
Legal Issues
#2 Suspected Abuse
POLICY
- Assault/abuse should be evaluated and reported to Los Angeles Sheriff’s Department (LASD) in all cases of assault/abuse reported by the patient or patient's caregiver. If the suspected perpetrator is a family member/caregiver or lives in the home of the child, a report should also be made to the Department of Children and Family Services (DCFS).
- Suspected Abuse in Pediatric:
- See Harbor-UCLA Policy 332B
- Suspected Abuse in Adults
- See Harbor-UCLA Policy 332A
- Perform MSE and provide appropriate medical care as necessary.
- Call Los Angeles County Sheriff’s Department (LASD) to report the incident. LASD will decide on the SART location, contact the appropriate jurisdictional law enforcement agency, and LASD or appropriate jurisdictional law enforcement agency will provide transport for the patient to the appropriate SART facility. The patient may choose to drive herself/himself, or other alternative transport, but law enforcement should follow them and needs to be present at the SART. You do not need to contact the accepting SART facility unless you have a specific question for them (see attachment 1 for contact information).
- Contact Social Work for supportive counseling and community resource referrals (see attachment 2 for a list of Rape Crisis Centers and hotlines).
- If the patient declines transportation to a SART facility for forensic examination and counseling, ED staff still need to report the incident to law enforcement.
- The patient should be offered prophylaxis against sexually transmitted illnesses as appropriate. HIV prophylaxis is not routinely offered but may done on a case to case basis.
- Suspected Abuse or Neglect in Dependent Adults or Elders
- See Harbor-UCLA Policy 332D
#11 Treatment of Minors Not Accompanied By Guardian
POLICY
- As described in Harbor-UCLA Policy 604A, any pediatric (or minor) patient presenting to the Emergency Department with an emergent problem may be seen without the parent/guardian present. Attempts to notify the family or legal guardian should be made as soon as possible. If the legally responsible representative is not available in the Emergency Department, notification should be attempted by telephone.
- Any other minor who presents without an emergent medical condition or special circumstances will require consent from a parent or guardian which can be in the form of a signed and dated note by the parent or guardian stating that medical care is requested or once contact is made with the parent or guardian.
- Patients with special circumstances as defined in Hospital Policy 604A, Appendix A, may be seen with the consent of the minor alone. These include:
- Emancipated or previously married minors
- Self-sufficient minors
- Active duty military
- Requiring care for a communicable disease
- Pregnancy-related concerns
- Rape or sexual assault
- Drug or alcohol abuse
- Mental health issues
#12 Consent for Blood Alcohol Tests Requested by Law Enforcement
Policy
- It is the policy of DHS hospitals (File:DHS policy 377 Blood Draws on Non-Consenting Persons Under Arrest for DUI of Alcohol, Drugs.pdf) to cooperate with the requests of police officers to obtain blood samples from arrestees for suspicion of driving a motor vehicle under the influence of alcohol who are brought to the ED for evaluation of medical or surgical problems, for use in determining alcoholic content for legal purposes.
- Note: Patients with hemophilia or on anti-coagulants are exempt from the blood test.
Protocol:
- Patients in police custody presenting to DEM for blood alcohol test MUST BE REGISTERED and have appropriate documentation made in the electronic medical record.
- If the blood sample is drawn by Harbor staff member, a PHYSICIAN SIGNATURE ON THE MEDICAL RECORD IS REQUIRED (eg, NEED MSE NOTE, OK TO BOOK FORM; no need for communication order).
- A police officer must sign a written request form, with witnessed signature. This will go into the medical record.
- If the patient has capacity, is conscious and coherent, reasonable effort should be made to obtain consent. If the patient does not have capacity, then implied consent per the state of California, allows the blood draw to occur.
- ED staff will not attempt to obtain a blood alcohol test if physical force is required (on the part of staff or law enforcement personnel) to obtain the test
- Police must supply the evidence collection tube for the lab draw and then follow chain of custody.
- For patient that do NOT have capacity and are getting a blood draw for their medical care, staff can draw for police if they have the appropriate written requests and the evidence tube per the implied consent in California.
#13 Leaving the Hospital Against Medical Advice
POLICY
- In approaching a patient who refuses medical care and/or wishes to leave the hospital against medical advice, in conjunction with Harbor-UCLA Policy 301, the following steps should be taken:
- The capacity of the patient to refuse medical care should be documented, i.e., the patient should be alert, oriented, rational, and able to understand the consequences of their decisions.
- The patient’s reason for refusal of care should be documented whenever possible.
- An attempt to persuade the patient to accept the recommended test, procedure, or treatment should be made and documented.
- If possible, a third party (family, private physician, nurse, social worker, clergy, etc.) should be used to help persuade the patient to accept the recommended care.
- If the patient is unable to follow-up with a provider within a reasonable time period, they should be encouraged to return to the emergency department for re-evaluation.
- The AMA Form should be signed by the patient, the physician, and one witness.
- If the patient refuses to sign the AMA Form, this should be documented in the chart.
- The patient should be provided with discharge instructions and appropriate prescriptions whenever possible despite refusal of certain aspects of care.
#14 Coroner's Cases (Including Release of Body or Remains)
POLICY
- All deaths in the DEM which meet the following criteria will be handled as a coroner’s case, in accordance with Section 102850 (Health and Safety Code, State of California). The coroner will be notified immediately when:
- Death is unattended (or unwitnessed)
- The deceased not attended by a physician within 20 days prior to death
- Where the attending physician is unable to state the cause of death
- Known or suspected homicide or suicide
- Where the deceased person died as a result of an accident
- Under such circumstances as to afford a reasonable ground to suspect that the death was caused by the criminal act of another
- Contagious disease constituting a public hazard
- Death in prison or while under sentence
- Death of all unidentified persons
Protocol:
- Emergency Department documentation will be completed in the electronic medical record including documentation of history, physical exam, and treatment by DEM staff, and time of death.
- The clerk will notify Bed Control of the death if the patient is assigned an inpatient bed.
- The DEM staff shall immediately notify the coroner for cases meeting the above criteria. The coroner’s case number should be documented in the electronic medical record if applicable.
- DEM staff will notify the patient’s family when they are available.
- DEM staff will notify social work for supportive counseling and community resources.
- Pastoral care will be notified as indicated at the request of the patient’s family and friends.
- Valuables/patient belongings may be removed and listed only by the coroner when the patient is dead on arrival. Otherwise, the patient’s valuables will be itemized and stored in patient valuables, or, in case of weapons, by the Los Angeles Sheriff’s Department.
- All infusion lines should be cut at point of entry and tied off or capped.
- Non-disposable equipment should be removed from patient prior to sending body to morgue.
- Non-Coroner’s Cases
- The DEM physician should notify the patient’s private attending physician, if known, to verify signing of death certificate.
#21 Medical-Legal Specimens
POLICY
- Medical-legal specimens removed from patients (e.g., a bullet) in the DEM will be handed to law enforcement if available or taken to the Pathology Department. Each person handling the specimen will be expected to complete the chain of possession information.
Protocol:
- Containers or envelopes for legal specimens can be obtained from Pathology.
- Complete all information on front of the small envelope. Physician to place specimen into the envelope and seal.
- Employee who seals the small envelope must sign across the outside flap.
- RN to fill in all information on the top third of the large envelope as well as #1 under Chain of Possession of Specimen. Place small envelope into larger one, DO NOT SEAL.
- RN to hand the envelope to law enforcement or take envelope along with Surgical Pathology Tissue Report Form (completed by Physician) to Pathology Department.
Consults
#5 Evaluation By Consulting Services
- This policy specifically outlines consultant evaluation of a patient after the initial MSE but PRIOR to ED Provider evaluation.
POLICY
- In general, consulting services should not evaluate ED patients prior to initiation of the medical screening exam (MSE). In certain select situations, a consulting service may evaluate patients after initiation of the MSE and prior to evaluation by the definitive ED providers if the following protocol is followed:
- The Consulting Resident identifies the ED patient(s) that they have not yet been consulted on that have an isolated problem in the specialty area of the consulting service.
- The Consulting Resident seeks approval from the ED provider to see this patient.
- The Consulting Resident evaluates the patient either in triage or their specialty clinic (i.e., not in a patient care area of the ED). The Consulting Resident is responsible for informing the RME area charge RN that the patient will be “out of department” so the nursing staff can note the patient’s location in the electronic patient tracking board.
- The Consulting Resident should document their exam findings along with assessment and treatment recommendations in the patient’s electronic medical record.
- The Consulting Resident then discusses the case with an ED provider who will also independently evaluate the patient and write their own note in the ED chart.
- DHS Policy 360a
- Emergent within 2 hours
- must document recommendations, attending co-sign within 24 hours
- DHS Policy 605 - 72 hours for attending signature
Psych
#6 Flow of Patients Between Psychiatry and ED
POLICY
- Initial Triage of Patients
- Ambulatory Patients
- Patients presenting with abnormal behavior without prior psychiatric diagnoses or with an acutely altered mental status are initially evaluated in the ED where a medical screening exam (MSE) will be performed. Patients with a known psychiatric history and behavior consistent with their previous diagnosis, without apparent acute medical problems requiring intervention, may be directly transferred to the Psychiatric ED after appropriate infectious disease screening. The triage nurse will provide a verbal report to the Psychiatric ED nurse. Arrangements for and acceptance of transfers from outside facilities are made by each respective service, for their service only.
- Ambulance Patients
- Patients arriving by via the ambulance entrance with psychiatric complaints should have an MSE initiated by a licensed ED provider. If the patient:
- Is determined to be safe to go to the waiting room (has capacity, not on 5150, not suicidal/homicidal), then the patient goes through the typical triage process.
- Requires immediate medical evaluation, the patient is placed in a patient care area in the ED and treated as indicated.
- Requires immediate psychiatric evaluation and has no acute medical issues, then the patient may be medically cleared and transferred to the Psychiatric ED after appropriate infectious disease screening. The ED provider will provide verbal report to the Psychiatric ED provider. Any history and physical examination by the ED provider should be documented in the electronic medical record. The ED nurse will call the Psychiatric ED nurse to inform them of the impending transfer.
- Patients arriving by via the ambulance entrance with psychiatric complaints should have an MSE initiated by a licensed ED provider. If the patient:
- Psychiatric Consultations to the ED
- All consultations are performed by (or are presented to and signed by) a licensed physician.
- Patients requesting voluntary evaluation by a psychiatrist are transferred to the Psychiatric ED after they have been medically cleared and as soon as a space is available for them in the Psychiatric ED. The ED provider discusses the case with the Psychiatry provider. Nursing is informed of the transfer and the patient is transferred with his/her paperwork, hospital ID, and personal belongings.
- Patients in the ED that have been medically cleared and require acute psychiatric evaluation are transferred to the Psychiatric ED as soon as a bed is available. Exceptions where the psychiatric evaluation is initiated while the patient is physically in the ED can be made on a case-by-case basis in consultation between the respective departments.
- The extent of evaluation for medical clearance in the ED is determined by the ED provider. Prior to the transfer, the ED provider will discuss the case with the Psychiatry provider. Nursing should be informed as soon as the transfer is agreed upon. The patient is transferred with their paperwork, hospital ID, and personal belongings.
- All patients on a 5150 hold:
- With a blood alcohol level or breathalyzer >0.200, delirium, complicated alcohol withdrawal, drug overdose, or other acute medical problems are evaluated in the ED.
- Require a psychiatric evaluation prior to discharge from the ED. This is done in the Psychiatric ED unless the ED provider agrees to have it performed in the ED.
- Require a psychiatric evaluation in the ED prior to admission.
- Should receive a psychiatric evaluation within a timely manner.
- Medical Consultations to the Psychiatric ED
- All consultations are performed (or are presented to and signed by) a licensed physician in a timely manner. Patients in the Psychiatric ED that require acute medical evaluation may either:
- Receive a medical consultation in the Psychiatric ED if the Psychiatric ED provider feels the patient is medically stable, OR...
- Be transferred to the ED as soon as a bed is available.
- All consultations are performed (or are presented to and signed by) a licensed physician in a timely manner. Patients in the Psychiatric ED that require acute medical evaluation may either:
- Medical indications of Psychiatric ED patients necessitating transfer to Medical ED.
- After evaluation by the Psychiatry provider it is felt the patient has suspected dementia, delirium, or other medical disorders, then the Psychiatry provider will write a brief note and discuss the patient with the ED provider. If the ED provider feels the patient warrants a transfer to the ED, they will notify the ED area charge nurse. The patient is then transferred with his/her paperwork, hospital ID card, and personal belongings as soon as an ED bed and patient sitter are available.
- Patients in the Psychiatric ED who may require treatment with sedating medications and are deemed to be at risk for significant oxygen desaturation when sedated, based on clinical evidence, should be transferred to a monitored bed in the ED. Examples of clinical evidence include a credible history of significant obstructive sleep apnea (OSA) or witnessed apnea, hypoxia, or desaturation when sleeping after treatment with sedating medications. Transfers to the ED from the Psychiatric ED for concerns about OSA should be based on physician clinical judgment, and not solely on body mass index. These patients are co-managed by physicians from both areas.
- Infectious Disease Isolation
- Patients under the care of the Psychiatry ED but temporarily located in the ED due to infectious disease isolation procedures will be primarily managed by the Psychiatry providers.
- Patients Requiring Placement
- Patients with chronic medical disorders (e.g., dementia) that require placement are managed in the ED. Psychiatric patients with chronic disorders (e.g., schizophrenia) that require placement are managed in the Psychiatric ED.
- Ambulatory Patients
Admissions
#3 CLINIC ADMISSIONS
POLICY
- A clinic patient who is a direct admit but requires a monitored bed when there is none available in the hospital should be sent to the DEM (AED or PED) after notification of the DEM attending physician or senior resident.
- Place patient on FirstNet Track as “Pre-Arrival”.
- A stable clinic patient who has been admitted to the hospital may be sent to the DEM on approval of the patient flow facilitator to await bed availability only after the appropriate medical and clerical admission duties have been completed in the admitting clinic, and the DEM attending physician or senior resident has been notified.
- Place patient on FirstNet Track as “Pre-Arrival”. It should be noted that the patient is a direct admission so that the ED registration does not occur.
Transfers
#4 Out of Plan Patients
POLICY
- Once the patient is deemed stable for transfer, the Emergency Department staff will attempt to arrange transfer to the appropriate facility for patients with third-party payer private insurance who require continued care beyond their ED (observation or admission). HUMC ED providers will make the determination of stability and the type of transport necessary (BLS, ACLS, physician transport, etc.).
- OOP Patient Protocol/Workflow
- The ED provider should collaborate with UR to notify OOP insurance/provider regarding the patient’s condition, clinical impression, and need for admission.
- If a private physician requests a transfer, the patient is deemed stable for transfer, and the patient agrees to be transferred, the transfer to the appropriate facility should be arranged using the procedure outlined in Harbor-UCLA Policy 308A.
Accepting Stable Inpatient Transfers 303a
- HUMC 303A
- HUMC must have capacity (reviewed by PFF), accepting physician, pt stable
- Does not apply to EMTALA EMC (Policy 308C)
Emergency transfers TO other facilities 308A
Emergency Transfers FROM other facilities 308C
ELTC DHS Transfer 373.3
EMS
#24 Paramedic Clinical Training
POLICY
- Paramedic/trainees, during the course of their education, will abide by the clinical practice policies for the Department of Emergency Medicine (DEM).
- Paramedics/trainees shall be directly supervised by a physician or a registered nurse working in the clinical area. Paramedic/trainees must adhere to local Los Angeles County Paramedic Scope of Practice Ref. 803, while performing clinical duties in the emergency department.
- Paramedics/trainees may administer medication only when directly supervised by a physician, registered nurse, or paramedic instructor. Paramedics/trainees may administer only those medications found in the Los Angeles County Paramedic Scope of Practice, Ref. 803. It is the responsibility of the paramedics/trainees to be knowledgeable of all information concerning each medication prior to administration.
- Any specific medical questions directed at a paramedic/trainee shall be referred to the patient’s physician or registered nurse.
- In the event of an incident involving a paramedic/trainee in the clinical setting, reporting of the incident should be in accordance with Harbor-UCLA policy 612A. The paramedic/trainee shall report the incident to the Charge Nurse, who will notify the prehospital care coordinator (PCC). The PCC will report the incident to the paramedic/trainee’s training institute and to their provider agency.
#25 RedditNet System
POLICY
- Updates of the ReddiNet System is the responsibility of the Mobile Intensive Care Nurse (MICN) on duty and will be in accordance with Los Angeles County Prehospital Care Manual Ref. 228 ReddiNet Utilization.
#26 Pronouncement in the Field
POLICY
- Pronouncement may only be performed by an attending physician in the Department of Emergency Medicine or a senior resident (3rd or 4th year resident) that has completed the Base Hospital Physician Course and Radio Internship.
- The physician will determine if futility is met and comply with LA County Prehospital Care Manual Ref No. 814 Determination/Pronouncement of Death in the Field when pronouncing a patient in the field.
- The MICN or Base Physician providing the online medical direction will complete the base documentation form with all of the pertinent information, including the name of the pronouncing physician and time of death.
ADDITIONAL DEM POLICIES AND PROCEDURES
Emergency Department Bedside Ultrasound (EBUS) Policy and Procedure Guidelines (#4 CLINICAL POLICIES-MISCELLANEOUS, Policy 4.7)
Animal Bites (#17 NOTIFICATIONS & REPORTING, Policy 17.2)
- All animal bites to people, including bites by domestic animals, are legally reportable in Los Angeles County, except for rodent and rabbit bites. Animal bites will be reported to the Los Angeles County Veterinary Public Health-Rabies Control Program by the DEM staff upon completion of emergency treatment. Exceptions include animal bites sustained in Pasadena, Long Beach, or Vernon, which should be reported to their respective animal control agencies.
- Reporting may be done via the Los Angeles County Veterinary Public Health-Rabies Control Program Animal Bite Reporting Form or via the Los Angeles Veterinary Public Health-Rabies Control Program online portal.
- Pertinent information should be documented in the electronic medical record and electronically submitted to Los Angeles County Veterinary Public Health (http://publichealth.lacounty.gov/vet/Forms.htm). This information includes:
- Name, sex, and age of patient
- Name, address, phone number of patient
- Address of circumstance (bite)
- Circumstance of bite
- Nature of wound and location of injury
- Treatment given and by whom
- Approximate age of animal
- Accurate description of animal
- Date and time of circumstance
Lost and Found (#17 NOTIFICATIONS & REPORTING, Policy 17.3)
- All lost and found items in the DEM can be secured as well as retrieved from the DEM property and valuable cashier located in the DEM registration area.
HIV testing in the ED (#18 DIAGNOSTIC TESTS, Policy 18.1)
- In compliance with Harbor-UCLA Policy 318, when HIV testing is performed in the ED:
- Patients MUST be informed that they are being tested for HIV, with an opportunity to decline, or “opt out” of the test.
- HIV tests ordered in the ED on patients who might be discharged should always be rapid HIV test, so that the results come back while the patient is in the ED. The ELISA test should be reserved for admitted patients.
- The ordering physician (or a designee) should follow up on the result of a rapid HIV test before the patient leaves the ED. If the patient leaves prior to completion of care, the patent should be placed on the lab follow-up track to ensure notification of results.
- For a positive HIV result in adults, the HIV fellow should be contacted. For pediatric patients, the pediatric ID service should be consulted. These consults should occur before the patient leaves ED, to arrange for follow up, to assist with recommendations regarding disclosure of the preliminary positive result, and also to ascertain the likelihood of this result being a true positive (if thrush, leukopenia, seborrheic dermatitis, etc. are present, the HIV service would like to see the patient in the ED). If the fellow cannot be reached, the Director of the HIV Clinics at HUCLA may be contacted.
- The patient should be informed of a positive result before leaving the ED and be counseled that the test (rapid HIV test or ELISAs) yields a preliminary result. A positive test doesn’t always indicate HIV infection, but should be taken seriously with arrangements made for early follow up of the confirmatory test.
- A confirmatory test (the Western Blot) should be sent on all patients with a positive rapid HIV or ELISA. The results take about a week come back and will be followed up by the HIV service.
- Patients should be scheduled to go to Harbor-UCLA Medical Center’s HIV clinic in about one week, to discuss test results (the Western Blot should be back by then). The fellow can help arrange for an appointment.
Follow-up of Abnormal Test Results – Adult ED and Pediatric ED (#18 DIAGNOSTIC TESTS, Policy 18.3)
- In conjunction with Harbor-UCLA Policy 393B, the following mechanisms have been established for notifying and recalling Emergency Department (ED) patients with abnormal/critical test results who are deemed to need further evaluation or care.
laboratory Studies:
- Critical Laboratory Values – When the laboratory calls the ED with critical lab values the following procedures will be followed:
- For patients in the ED, the clerk who receives the call from the lab will transfer the call to the RN caring for the patient. The RN will verbally report the critical lab value to the appropriate care provider. This verbal report process includes a read back by the provider for confirmation, and nursing documentation of the verbal report in the electronic medical record. In all cases, the provider and nurse caring for the patient will be apprised of the test results.
- For patients still in the waiting room, the clerk who receives the call from the lab will refer the call to the triage provider, who will assure that the patient is brought into the ED for further evaluation as soon as appropriate and possible.
- For patients who have been discharged from the ED, or who have left the ED or waiting room before completion of their evaluation, the clerk who receives the call from the lab will refer the call to the triage provider. The provider will attempt to contact the patient (by phone or telegram) and ask him/her to return to the ED for evaluation if appropriate. Documentation of communications regarding critical lab results and plan of action will be placed in the electronic medical record.
- Critical Laboratory Values – When the laboratory calls the ED with critical lab values the following procedures will be followed:
- Lab Follow-up:
- Any patients with outstanding lab results at the point of discharge will be placed on the lab follow-up track for review and patient contact once the labs are resulted.
- Clinic Referrals:
- When patients are referred to Harbor-UCLA Medical Center clinics or to community clinics with access to the hospital information system, follow-up on laboratory results can be performed by their empaneled provider. The ED provider should message the empaneled provider in the EHR (and “save to chart”) to ensure follow-up.
- Sexually Transmitted Disease:
- Patients with outstanding tests for sexually transmitted infections (STI) should be placed on the lab follow-up track. Once reviewed, the patient will be contacted with results and prescriptions will be given if further treatment is warranted.
- Radiographic Studies:
- Plain film (x-ray) radiographic studies performed on ED patients are always interpreted by the emergency provider prior to the patient being discharged from the ED. This initial interpretation is documented in the electronic medical record. All radiographic studies are also interpreted by the radiologist.
- For all radiographic studies, when there is a critical result or the radiologist's interpretation differs significantly from the emergency physician's interpretation, radiology will immediately notify the Adult ED attending or DEM senior resident for adult patients, and the PED attending or resident for pediatric patients, per the Department of Radiology policy. If the patient has left the ED, the ED Attending or Senior Resident will review the patient's record. If appropriate, the physician will call or send the patient/child’s parents a telegram informing them of the need to return to the ED for re-evaluation. The physician’s actions are recorded in the patient's medical record.
- Microbiology Studies:
- Positive blood or stool cultures are reported by laboratory to the AED senior resident for adult patients, and to the senior PED resident or pediatric nurse practitioner in the PED. The provider is responsible for review of the electronic medical record, and for calling the patient back to the ED for re-evaluation and treatment as needed. The provider is also responsible for documentation of their medical decision making about
Medical Screening Examination Policy (#21 TRIAGE AND MEDICAL SCREENING EXAMINATION, Policy 21.1)
- A medical screening exam (MSE) will be provided to any child or adult who comes to the Emergency Department (ED) per the Harbor-UCLA Policy 374A Medical Screening Exam. The MSE will be performed within the capability of the Department of Emergency Medicine. The examination will be the same appropriate screening examination that would be performed on any individual with similar signs and symptoms, regardless of the individual’s ability to pay for medical care.
- A medical record will be established for every patient who registers to be seen in the ED. If a patient leaves the hospital before receiving a MSE, a hospital medical record will be established for the patient with documentation of the results of the visit.
- The MSE is a continuous process reflecting ongoing monitoring in accordance with the individual’s needs. Monitoring will continue until the individual is stabilized or appropriately transferred. Reevaluation of the patient must occur prior to discharge or transfer.
- The categories of persons qualified to perform a ED MSE include licensed independent practitioners (physicians and nurse practitioners).
Guidelines for Triage and Medical Screening Examination (MSE) (#21 TRIAGE AND MEDICAL SCREENING EXAMINATION, Policy 21.2)
- Triage priority is based on the router nurse’s perceived urgency of a patient’s need for medical evaluation and/or treatment following initial assessment. Patient acuity is determined at the time of triage in accordance with the Emergency Severity Index (ESI). Please refer to the AHRQ Implementation Handbook for details.
- Ambulance patients are generally placed directly into ED treatment bays, but may be referred to the Triage/MSE Area for formal assessment and prioritization relative to other ED waiting room patients if assessment by a licensed physician determines that the patients are non-critical and stable for triage.
- An MSE will be performed and documented on all patients who register for evaluation in compliance with Harbor-UCLA Policy 374A. After triage, low-acuity patients who have been determined to not have an emergent medical condition (EMC) after initial evaluation may qualify to be seen in the Urgent Care Clinic (UCC), GYN Urgent Care Clinic, or referral to another specialty clinic. At no time will ED staff imply that patients must be seen in the UCC.
- For patients with severe pain, the nurse and/or independent practitioner will document how the patient’s pain was addressed prior to sending the patient to the UCC for further evaluation.
Risk Assessment Policy (#21 TRIAGE AND MEDICAL SCREENING EXAMINATION, Policy 21.3)
- All patients presenting to the DEM will be screened for the following risk:
- Falls
- Domestic Violence/Abuse
- Psychiatric illness/suicide ideation
- Violence predictability/aggressive behavior
- ILI/CLI
- RIPT (adults only)
- RIPT Protocol
- Factors, symptoms or complaints of respiratory tuberculosis (TB) using the RIPT criteria.
- All adult patients presenting to the Emergency Department will be screened by a registered nurse at the time of triage using the RIPT criteria in the electronic health record (EHR).
- A total of five points or greater indicates the need for immediate initiation of the RIPT procedure.
- The nurse will explain to the patient and family the need for respiratory isolation precautions including masking of the patient.
- The triage nurse will notify the triage provider who will order a PA and lateral chest x-ray.
- The triage nurse will hand off communication to the Area Charge Nurse (ACN).
- On completion of the chest x-ray, the ACN will follow-up with a Senior Resident or Attending Physician for interpretation of the chest x-ray.
- The decision to release the patient back to the waiting area or continue isolation in a designated isolation room will be made by the provider at that time.
- All documentation of the RIPT and interventions shall be maintained in the EHR.
Care of the Potential Myocardial Ischemia Patient in Triage (#21 TRIAGE AND MEDICAL SCREENING EXAMINATION, Policy 21.4)
- All adult patients presenting to the DEM triage area with a chief complaint suggestive of myocardial ischemia will be screened rapidly to determine the need for immediate intervention.
Protocol
- All adult patients presenting to the Emergency Department will be screened by the Router RN for suspected cardiac ischemia using the following criteria:
- Age >35 AND chest, arm, neck, jaw pain that is described as pressure, heaviness, or discomfort.
- Age >45 AND Shortness of Breath, weakness, or arm numbness, CONCERNING FOR A CARDIAC ETIOLOGY and without other explanation
- Age > 65 AND Nausea, lightheadedness, “indigestion”, or “dizziness" CONCERNING FOR A CARDIAC ETIOLOGY and without other explanation
- Clinical concern for myocardial ischemia exists despite absence of 1-3
- If the patient meets the above criteria the Router RN will assign “cardiac” triage priority which automatically orders an EKG.
- Router RN will notify the triage RN/provider team
- Patient will be placed immediately in Triage room 1
OLD POLICIES AND PROCEDURES (as of 7-28-2021)=
Home Page → Policies and Procedures → HUMC → HUMC Policies and Procedures
ALL POLICIES ARE IN ADDITION TO AND NOT IN PLACE OF HARBOR-UCLA AND DHS POLICIES
2 - Abuse (Adult and Peds)
- Peds
- If <120 hours, contact Sheriff, DCFS, and SCAN Teams (8-5 M-F on-site at HUMC, otherwise USC or SART Center)
- If >120 hours, contact SCAN team to determine appropriate evaluation and follow-up
- Adult
- Refer to SART center if <120 hours since assault
- Contact Sheriff who will determine appropriate SART center and either transport or escort the patient
- HIV prophylaxis is not routinely given, but can be offered in conjunction with ID recommendations
- SART Center at Little Company of Mary San Pedro 562-497-0147
1 Abuse (Adult and Peds) POLICY: Assault/abuse should be evaluated and reported to Los Angeles Sheriff’s Department (LASD) in all cases of assault/abuse reported by the patient or patient's caregiver. If the suspected perpetrator is a family member/caregiver or lives in the home of the child, a report should also be made to the Department of Children and Family Services (DCFS).
ADULTS
- See Harbor-UCLA Policies 332A
- Perform MSE and provide appropriate medical care as necessary.
- Call Los Angeles County Sheriff’s Department (LASD) to report the incident. LASD will decide on the SART location, contact the appropriate jurisdictional law enforcement agency, and LASD or appropriate jurisdictional law enforcement agency will provide transport for the patient to the appropriate SART facility. The patient may choose to drive herself/himself, or other alternative transport, but law enforcement should follow them and needs to be present at the SART. You do not need to contact the accepting SART facility unless you have a specific question for them (see attachment 1 for contact information).
- Contact Social Work for supportive counseling and community resource referrals (see attachment 2 for a list of Rape Crisis Centers and hotlines).
- If the patient declines transportation to a SART facility for forensic examination and counseling, ED staff still need to report the incident to law enforcement. The patient should be offered prophylaxis against sexually transmitted illnesses as appropriate. HIV prophylaxis is not routinely offered but may done on a case to case basis after evaluation by the Infectious Diseases service.
PEDIATRICS:
- See Harbor-UCLA Policy 332B
SUSPECTED ABUSE OR NEGLECT OF DEPENDENT ADULTS OR ELDERS
- See Harbor-UCLA Policies 332D
12 - Consent for Blood Alcohol Tests
- Patient must be registered, police sign written consent form
- ED staff will draw samples if the patient submits to the test, but will NOT attempt to obtain blood if physical force is required (by staff or law enforcement) to obtain the test
- Persons under arrest are only deemed to have given implied consent if they are unconscious or cannot refuse a test for other reasons
- DHS Policy 377
- HUMC 312
- 8.3
- Disability will not be given to emergency department patients by ED staff. Patients requesting disability will be referred to a long term care provider (at Harbor-UCLA Medical Center or in the community). Patients who have been followed in the Harbor-UCLA Medical Center Clinics may be referred to the Medical Records Department (daytime, Monday – Friday) to determine if the medical record contains sufficient documentation to complete the disability forms.
- Short term time off (< one week) or limited duty (< one week) may be given by the emergency physician to a patient with an acute problem needing short term restricted activities. To give limited time off or restricted activity, the emergency physician is to write for the specific restricted activity and duration of time in the discharge-related documentation in the electronic medical record (eg. Off work 2 days; strict bed rest 2 days; no lifting >15# for 5 days). The patient is to be given a copy of their discharge paperwork at time of ED discharge.
- In the setting of infectious diseases requiring a period of quarantine, CDC guidelines should be followed for prescription of time off work/school.
10 - Residents & Medical Students
10.1 Supervision of Medical Students
- Medical Students
- Medical students may perform histories, physical examinations, and procedures with appropriate supervision. All medical orders require co-signature by a licensed physician. Medical students are supervised at all times by the residents and faculty assigned to the DEM. All charts by medical students must be cosigned by a licensed physician and reviewed by the senior Emergency Medicine resident or faculty member.
10.2 Approval of DEM Housestaff in Performance of Invasive Procedures
POLICY:
DEM housestaff are initially allowed to perform specified procedures only under the direct supervision of DEM faculty or other housestaff who have already been approved in the performance of those procedures. Once residents have been approved for a certain procedure, they are allowed to perform the procedure independently, with indirect supervision of faculty.
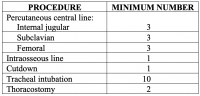
The following is a list of the procedures that are covered by this policy, including the number of times each procedure must be performed under direct supervision before a resident can be approved in that procedure:
- PROCEDURE MINIMUM NUMBER
- Percutaneous central line:
- Internal jugular 3
- Subclavian 3
- Femoral 3
- Intraosseous line 1
- Cutdown 1
- Tracheal intubation 10
- Thoracostomy 2
- Percutaneous central line:
Procedure
- The following procedure will be used to privilege DEM housestaff in the performance of specified procedures:
- When a resident performs a procedure he/she will fill out a procedure note in the electronic health record (and in a separate electronic log when at outside rotations), which identifies the patient, the procedure performed and the supervising physician.
- Intermittently, each resident will be provided with feedback regarding the number of procedures they have performed. This feedback will note the procedures they are currently credentialed to perform independently.
- This will be posted for reference on iPrivileges/Resident Competencies located on the Harbor-UCLA intranet homepage (Clinical --> Applications -> iPrivileges).
10.3 Transition of Care
All transitions of care for patients occur during rounds. Rounds occur 3 times a day between 8-hours shifts with overlap. Rounds are staggered so that there is not a complete change of providers at any given time. Most patients are seen and discharged or admitted during one shift. There are no more than 3 transitions in a 24 hour period. Patients who are signed out to an oncoming team are assigned a new provider on the electronic health record (EHR) and the providers communicate two identifiers (typically name and MRN#), current clinical condition, what has been done for the patient, any tests, tasks or consults that require follow-up, and a working diagnosis when appropriate. Rounds are supervised by an Emergency Medicine attending physician.
11 - Med Legal Section
- Drugs found on patients (other than small amount of THC)
- Call the Sheriffs to dispose of substance
- No charges pressed if here for OD
- If here for CC other than drug OD, may have charges pressed
- Call the Sheriffs to dispose of substance
11.1 Medical-Legal Specimens
Medical –legal specimens removed from patients in the DEM will be handed to law enforcement if available or taken to the Pathology Department. Each person handling the specimen will be expected to complete the chain of possession information.
PROCEDURE
- Containers or envelopes for legal specimens can be obtained from Pathology.
- Complete all information on front of the small envelope. Physician to place specimen into the envelope and seal.
- Employee who seals the small envelope must sign across the outside flap.
- RN to fill in all information on the top third of the large envelope as well as #1 under Chain of Possession of Specimen. Place small envelope into larger one, DO NOT SEAL.
- RN to hand envelope to law enforcement or take envelope along with Surgical Pathology Tissue Report Form (completed by Physician) to Pathology Department.
14 Medications
14.2 Prescription Refill for Patients from Harbor-UCLA Clinics
- Medications will only be refilled for registered ED patients. Unregistered patients will be referred back to their primary care provider for refills.
- For psychiatric medication refills, referral can be made to the Psychiatric ED or Exodus.
15.1 Visitors in the ED
- Due to the unique setting of the Emergency Department, the decision to permit visitation is at the discretion of the Emergency Department staff. Visitation may be restricted in an emergency situation and/or any active or potential hospital safety situation.
- In accordance with Harbor-UCLA Policy 109A, each patient has the right to designate visitors of his/her choosing with the following exceptions:
- Staff safety needs to be maintained at all times;
- Staff needs to be able to perform their duties with minimal interference from visitors;
- When no visitors are allowed;
- The patient has notified the healthcare provider that he/she no longer wants a particular person to visit;
- No more than one visitor at the bedside unless approved by DEM staff; or
- Visitors must remain inside the patient’s room. Visitors will not be allowed to stand in the hallways.
In some instances, it may be beneficial to allow a family member or support person to be present while a procedure is being performed at the discretion of ED staff. This usually relates to a parent/guardian of a child, caregiver, or support person who can enhance the patient cooperation interaction experience.
- Family presence at the bedside or in the room is encouraged for a variety of medical or surgical procedures, including resuscitation, while avoiding any disruption in care being provided.
- A chair should be provided for all family members who are present during a procedure/resuscitation for their own safety.
- Prior to a family member entering the resuscitation area, a staff member will notify the team that the family has arrived/present.
- Offer the family simple comforts such as a phone, tissues, water, restroom access, and clergy.
- As much as possible, a staff member (MD, NP, RN, LCSW) will accompany and explain to the family members the following:
- What they are about to see.
- They can leave the room at any time.
- They may be asked to leave the room at any time for a variety of reasons
- While we understand that they may become emotional and we support. their feelings, they must not interfere with medical treatment.
- In the event of patient death:
- Department of Social Services or nursing should provide the family with a copy of the Harbor UCLA Medical Center Bereavement Packet with information on funeral homes, community support groups, and information concerning the disposition of the body.
- For pediatric deaths, nursing may offer the family a lock of hair, a hand or foot print when possible.
- Provide the family with the telephone number to the ED for any questions they may have after returning home.
16 Prehospital Care
16.1 Paramedic Clinical Training Policy
- Paramedic/trainees, during the course of their education, will abide by the clinical practice policies for the Department of Emergency Medicine (DEM).
- Paramedics/trainees shall be directly supervised by a physician or a registered nurse working in the clinical area. Paramedic/trainees must adhere to local EMT-P Scope of Practice, per Ref. 803 Los Angeles County Prehospital Care Manual, while performing clinical duties in the emergency department.
- Paramedics/trainees may administer medication only when directly supervised by a physician, registered nurse, or paramedic instructor. Paramedics/trainees may administer only those medications found in the Los Angeles EMT-P Scope of Practice per Los Angeles County Prehospital Care Manual Ref. 803. It is the responsibility of the paramedics/trainees to be knowledgeable of all information concerning each medication prior to administration.
- Any specific medical questions directed at a paramedic/trainee shall be referred to the patient’s physician or registered nurse.
- In the event of an incident involving a paramedic/trainee in the clinical setting, reporting of the incident should be in accordance with Harbor-UCLA policy 612A. The paramedic/trainee shall report the incident to the Charge Nurse, who will notify the prehospital care coordinator (PCC). The PCC will report the incident to the paramedic/trainee’s training institute and to their provider agency.
16.4 Guidelines for Prouncement in the Field
- Pronouncement may only be performed by an attending physician in the Department of Emergency Medicine or a senior resident (3rd or 4th year resident) that has completed the Base Hospital Physician Course and Radio Internship.
- The physician will determine if futility is met and comply with LA County Prehospital Care Manual Ref No. 814 Determination/Pronouncement of Death in the Field when pronouncing a patient in the field.
- The MICN or Base Physician providing the online medical direction will complete the base documentation form with all of the pertinent information, including the name of the pronouncing physician and time of death
16.5 Paramedic Radio Candidate (Internship) Protocol
- In order to be eligible to begin internship, the MICN or Base Physician candidate must demonstrate completion of the LA County MICN certification examination or Harbor-UCLA Base Physician Course respectively.
- Currently certified MICNs, not sponsored by Harbor, requesting to intern on Harbor’s paramedic radios will: 1) Provide proof of current Advanced Cardiac Life Support Provider Course completion and 2) Provide proof of current Los Angeles County MICN certification.
- Preceptors will directly observe the candidate in the process of taking paramedic runs.
- The direction of the run will be the responsibility of the preceptor.
- Direction of a paramedic run by a MICN or Base Physician candidate without the observation of a preceptor may be considered grounds for failure.
- Preceptors will have a minimum of 6 months experience as a MICN at Harbor, or be a senior DEM resident or a DEM attending that has completed the Base Physician Course and Internship.
- MICNs must comply with LA County Prehospital Care Manual Ref 1010 Mobile Intensive Care Nurse (MICN) Certification and complete the internship in accordance with this policy.
- Satisfactory completion of radio internship will require that the Base Hospital Medical Director (BHMD), PCC and Asst. PCC (if applicable) are in agreement that the MICN or Base Physician candidate has performed in a safe and competent manner in the area of assessment, treatment, verbal communication, or record keeping skills.
- Failure of internship will require that the BHMD, PCC, and Asst. PCC (if applicable) are in agreement that the MICN or Base Physician candidate has failed to perform in a safe and competent manner in assessment, treatment, verbal communication, or record keeping skills.
- In the event of failure of an MICN candidate, the MICN candidate may petition the BHMD and PCC to retake the radio internship. The petition should occur within 6 months of taking the LA County MICN certification, or Harbor-UCLA authorization exam.
- In the event of failure of a DEM physician candidate, the physician will be remediated until competency is achieved.
17 Notification & Reporting
17.1 Family and Next-of-Kin
- All attempts will be made to notify family or legal guardians whenever possible and as soon as possible when a minor presents or is brought to the emergency room. However, these attempts will not delay emergent care when an emergency medical condition exists. Additionally, the family or next-of-kin of adult patients will be notified at the patient’s request.
- In the event of a critical patient or patient death Social Services will be contacted to assist with family notification.
- All attempts to notify family and next of kin should be documented on the patient’s health record.
17.2 Animal Bites
- All animal bites to people, including bites by domestic animals, are legally reportable in Los Angeles County, except for rodent and rabbit bites. Animal bites will be reported to the Los Angeles County Veterinary Public Health-Rabies Control Program by the DEM staff upon completion of emergency treatment. Exceptions include animal bites sustained in Pasadena, Long Beach, or Vernon, which should be reported to their respective animal control agencies.
- Reporting may be done via the Los Angeles County Veterinary Public Health-Rabies Control Program Animal Bite Reporting Form or via the Los Angeles Veterinary Public Health-Rabies Control Program online portal.
- Pertinent information should be documented in the electronic medical record and electronically submitted to Los Angeles County Veterinary Public Health
18 Diagnostic Tests
18.1 HIV testing in the ED
In compliance with Harbor-UCLA Policy 318, when HIV testing is performed in the ED:
- Patients must be informed that they are being tested for HIV, with an opportunity to decline, or “opt out” of the test.
- HIV tests ordered in the ED on patients who might be discharged should always be rapid HIV test, so that the results come back while the patient is in the ED. The ELISA test should be reserved for admitted patients.
- The ordering physician (or a designee) should follow up on the result of a rapid HIV test before the patient leaves the ED. If the patient leaves prior to completion of care, the patent should be placed on the lab follow-up track to ensure notification of results.
- For a positive HIV result in adults, the HIV fellow should be contacted. For pediatric patients, the pediatric ID service should be consulted. These consults should occur before the patient leaves ED, to arrange for follow up, to assist with recommendations regarding disclosure of the preliminary positive result, and also to ascertain the likelihood of this result being a true positive (if thrush, leukopenia, seborrheic dermatitis, etc. are present, the HIV service would like to see the patient in the ED). If the fellow cannot be reached, the Director of the HIV Clinics at HUCLA may be contacted.
- The patient should be informed of a positive result before leaving the ED, and be counseled that the test (rapid HIV test or ELISAs) yields a preliminary result. A positive test doesn’t always indicate HIV infection, but should be taken seriously with arrangements made for early follow up of the confirmatory test.
- A confirmatory test (the Western Blot) should be sent on all patients with a positive rapid HIV or ELISA. The results takes about a week come back and will be followed up by the HIV service.
- Patients should be scheduled to go to Harbor-UCLA Medical Center’s HIV clinic in about one week, to discuss test results (the Western Blot should be back by then). The fellow can help arrange for an appointment.
18.3 Follow-up of Abnormal Test Results – Adult ED and Pediatric ED
In conjunction with Harbor-UCLA Policy 393B, the following mechanisms have been established for notifying and recalling Emergency Department (ED) patients with abnormal/critical test results who are deemed to need further evaluation or care.
- Laboratory Studies:
- Critical Laboratory Values – When the laboratory calls the ED with critical lab values the following procedures will be followed:
- For patients in the ED, the clerk who receives the call from the lab will transfer the call to the RN caring for the patient. The RN will verbally report the critical lab value to the appropriate care provider. This verbal report process includes a read back by the provider for confirmation, and nursing documentation of the verbal report in the electronic medical record. In all cases, the provider and nurse caring for the patient will be apprised of the test results.
- For patients still in the waiting room, the clerk who receives the call from the lab will refer the call to the triage provider, who will assure that the patient is brought into the ED for further evaluation as soon as appropriate and possible.
- For patients who have been discharged from the ED, or who have left the ED or waiting room before completion of their evaluation, the clerk who receives the call from the lab will refer the call to the triage provider. The provider will attempt to contact the patient (by phone or telegram) and ask him/her to return to the ED for evaluation if appropriate. Documentation of communications regarding critical lab results and plan of action will be placed in the electronic medical record.
- Lab Follow-up
- Any patients with outstanding lab results at the point of discharge will be placed on the lab follow-up track for review and patient contact once the labs are resulted.
- Clinic Referrals – When patients are referred to Harbor-UCLA Medical Center clinics or to community clinics with access to the hospital information system, follow-up on laboratory results can be performed by their empaneled provider. The ED provider should message the empaneled provider in the EHR (and “save to chart”) to ensure follow-up.
- Sexually Transmitted Disease Information – Patients with outstanding tests for sexually transmitted infections (STI) should be placed on the lab follow-up track. Once reviewed, the patient will be contacted with results and prescriptions will be given if further treatment is warranted.
- Radiographic Studies:
- Plain film (x-ray) radiographic studies performed on ED patients are always interpreted by the emergency provider prior to the patient being discharged from the ED. This initial interpretation is documented in the electronic medical record. All radiographic studies are also interpreted by the radiologist.
- For all radiographic studies, when there is a critical result or the radiologist's interpretation differs significantly from the emergency physician's interpretation, radiology will immediately notify the Adult ED attending or DEM senior resident for adult patients, and the PED attending or resident for pediatric patients, per the Department of Radiology policy. If the patient has left the ED, the ED Attending or Senior Resident will review the patient's record. If appropriate, the physician will call or send the patient/child’s parents a telegram informing them of the need to return to the ED for re-evaluation. The physician’s actions are recorded in the patient's medical record.
- Microbiology Studies:
- Positive blood or stool cultures are reported by laboratory to the AED senior resident for adult patients, and to the senior PED resident or pediatric nurse practitioner in the PED. The provider is responsible for review of the electronic medical record, and for calling the patient back to the ED for re-evaluation and treatment as needed. The provider is also responsible for documentation of their medical decision making about these test results in the electronic medical record
21 Triage and Medical Screening Examination
==21.1 Medical Screening Examination Policy
- A medical screening exam (MSE) will be provided to any child or adult who comes to the Emergency Department (ED) per the Policy No. 374A Medical Screening Exam. The MSE will be performed within the capability of the Department of Emergency Medicine. The examination will be the same appropriate screening examination that would be performed on any individual with similar signs and symptoms, regardless of the individual’s ability to pay for medical care.
- A medical record will be established for every patient who registers to be seen in the ED. If a patient leaves the hospital before receiving a MSE, a hospital medical record will be established for the patient with documentation of the results of the visit.
- The MSE is a continuous process reflecting ongoing monitoring in accordance with the individual’s needs. Monitoring will continue until the individual is stabilized or appropriately transferred. Reevaluation of the patient must occur prior to discharge or transfer.
- The categories of persons qualified to perform a ED MSE include licensed independent practitioners (physicians and nurse practitioners).
21.2 Guidelines for Triage and Medical Screening Examination (MSE)
- Triage priority is based on the router nurse’s perceived urgency of a patient’s need for medical evaluation and/or treatment following initial assessment. Patient acuity is determined at the time of triage in accordance with the Emergency Severity Index (ESI). Please refer to the AHRQ Implementation Handbook for details.
- Ambulance patients are generally placed directly into ED treatment bays, but may be referred to the Triage/MSE Area for formal assessment and prioritization relative to other ED waiting room patients if assessment by a licensed physician determines that the patients are non-critical and stable for triage.
- A MSE will be performed and documented on all patients who register for evaluation in compliance with Harbor-UCLA Policy 374A. After triage, low-acuity patients who have been determined to not have an emergent medical condition (EMC) after initial evaluation may qualify to be seen in the Urgent Care Clinic (UCC), GYN Urgent Care Clinic, or referral to another specialty clinic. At no time will ED staff imply that patients must be seen in the UCC.
- For patients with severe pain, the nurse and/or independent practitioner will document how the patient’s pain was addressed prior to sending the patient to the UCC for further evaluation.
- Patients with the following vital signs should not be referred out of the Emergency Department:
- Blood Pressure < 90/50 or > 240/140
- Heart Rate < 40 or >120
- Temperature < 95˚F or >103.9˚F
- Respiratory Rate < 8 or ≥ 28
- Pulse Oximetry < 90% on room air or the patient’s dose of home oxygen
- Glucose < 60 or > 400 (Only measure if indicated/not necessary on all patients)
21.3 Respiratory Isolation Patient Protocol[1]
All adult patients presenting to the DEM will be screened at the time of triage by a RN for risk factors, symptoms or complaints of respiratory/tuberculosis (TB) using the RIPT criteria in the EHR; five points or greater indicates the need for immediate initiation of the RIPT procedure.
- A mask will be placed on the patient and PA/Lateral chest x-ray will be ordered by the triage provider or nurse (with a DEM Attending on duty as ordering physician)
- The patient will be escorted to the radiology waiting area, and the triage nurse will hand off communication to the Area Charge Nurse (ACN).
- On completion of the chest x-ray, the ACN will follow-up with the R-3 or Attending Physician for interpretation of the chest x-ray. The decision to release the patient back to the waiting area or continue isolation in a designated isolation room will be made by the provider at that time.
<https://www.ncbi.nlm.nih.gov/pubmed/10736118>
<http://www.currytbcenter.ucsf.edu/sites/default/files/ic_book_2011.pdf>
21.4 Care of Potential Myocardial Ischemia Patient in Triage
- All adult patients presenting to the DEM triage area with a chief complaint suggestive of myocardial ischemia will be screened rapidly by the Router RN to determine the need for immediate intervention using the following criteria:
- Age >35 AND chest, arm, neck, jaw pain that is described as pressure, heaviness, or discomfort.
- Age >45 AND Shortness of Breath, weakness, or arm numbness, CONCERNING FOR A CARDIAC ETIOLOGY and without other explanation
- Age > 65 AND Nausea, lightheadedness, “indigestion”, or “dizziness" CONCERNING FOR A CARDIAC ETIOLOGY and without other explanation
- Clinical concern for myocardial ischemia exists despite absence of 1-3
- If the patient meets the above criteria the Router RN will assign “cardiac” triage priority which automatically orders an EKG.
- the patient will be placed in RME1 for immediate EKG
- Once the ECG has been completed, the triage nurse will notify the RME provider who will review the ECG
Approved June 2015, Chappell 2/22/16
21.5 Medications in Triage: Standardized Procedure
- Administration of medications in triage (MIT) is to provide timely treatment for patients arriving to the ED with pain, fever, dyspepsia, or nausea and vomiting at the time of triage/assessment and reassessment. Available medications include Acetaminophen, Ibuprofen, Maalox, or Ondansetron.
- PAIN: All patients who arrive to the ED Triage area will have their level of pain assessed and documented in the EMR. The pain scales used are FLACC, Numeric, and Faces, depending upon the age of the patient.
- FEVER: All patients who present to the ED Triage area will have their temperatures taken and documented in the electronic medical record. All patients who present with a temperature > 100.4º F (38º C) [can be axillary, rectal, or oral temperature] shall be offered acetaminophen or ibuprofen. If a previous antipyretic has been given (either at home or in triage), an alternate antipyretic will be given if temperature >100.4º F (38º C). Rectal temperatures must be obtained for all of the following pediatric patients: Infants less than 2 months old, Children less than 2 years old with the exception of children presenting with minor trauma, & Active seizure patients up to 3 years old
- Assessment of the patient’s symptoms (pain, fever, gastritis symptoms, nausea and/or vomiting) should be reassessed within 1 hours of the medication given in triage.
- Patients who after reassessment of pain (within one hour of receiving the 1st dose of acetaminophen or ibuprofen) continue to complain of pain and desire further analgesic treatment will then be offered acetaminophen or ibuprofen alternating from the previous medication administration.
- Patients who continue to complain of pain and/or fever may have a repeat dose of acetaminophen 4 hours after the initial dose, and/or a repeat dose of ibuprofen 6 hours after the initial dose.
- Patients who continue to complain of dyspepsia may have a repeat dose of aluminum hydroxide and magnesium hydroxide antacid (Mag-Al Plus) 6 hours after the initial dose.
- A nurse practitioner or physician provider will be notified of any patient that:
- The triage nurse assesses to require more analgesia than oral acetaminophen or ibuprofen or aluminum hydroxide and magnesium hydroxide antacid (Mag-Al Plus) can provide
See Also
- Harbor:Main
- Harbor: ED Bedside Ultrasound Policy and Procedure Guidelines
- Harbor: Base Hospital Resource for Physicians and MICNs
- ↑ Approved June 2015, Chappell 2/22/16