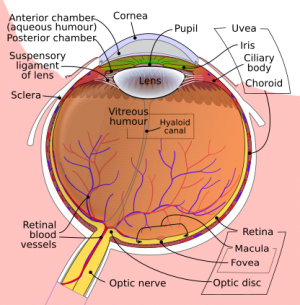
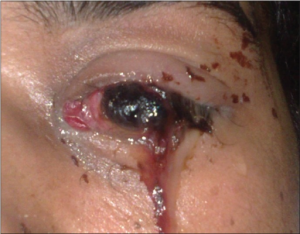
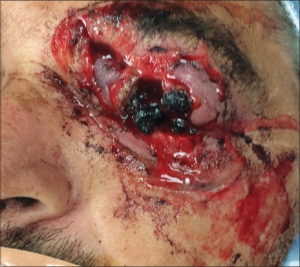
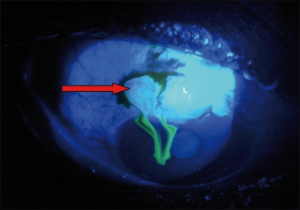
Globe rupture
Background
- Vision threatening emergency
- Is a full thickness disruption of sclera or cornea[1]
- Be careful not to apply pressure to eye
- Evert lids with paperclips or eyelid retractors
Causes
- Blunt Eye Trauma
- Caused by suddenly elevated IOP
- Penetrating trauma
- Suspect globe penetration with any puncture or laceration of eyelid or periorbital area
- More commonly associated with objects from metal on metal, lawn mower, drills, grinders[2]
Clinical Features
- Eye pain
- +/- decreased visual acuity
- Teardrop-shaped pupil
- Flat anterior chamber
- Extrusion of intraocular content
- Subconjunctival hemorrhage involving entire (360 degree) sclera
- Hemorrhagic chemosis
Slit-lamp
- Once the diagnosis of a ruptured globe is made, further examination should be DEFERRED until the time of surgical repair in the operating room. Consider diagnosis via penlight exam. Slit lamp findings described below, but crucial to avoid any pressure on eye, which risks extrusion of intraocular contents.
- Deep or shallow anterior chamber compared to fellow eye, full thickness scleral or corneal laceration, severe subconjunctival hemorrhage (especially involving 360 degrees of bulbar conjunctiva, often bulbous), peaked or irregular pupil, iris transillumination defect, lens material or vitreous in the AC, foreign body tract or new cataract in the lens, limitation of extraocular motility (greatest in the direction of rupture), intraocular contents may be outside of the globe
- Hyphema, periorbital ecchymosis, Lens dislocation, traumatic optic neuropathy, choroidal rupture, dislocated/subluxed lens
- Seidel's sign - do not perform this test if suspect open globe
- May be falsely negative if scleral rupture is small
Differential Diagnosis
Maxillofacial Trauma
- Ears
- Nose
- Oral
- Other face
- Zygomatic arch fracture
- Zygomaticomaxillary (tripod) fracture
- Related
Evaluation
- Inspect lids, lashes, cornea, sclera, and pupils.
- Evaluate for a relative afferent pupillary defect
- Visual acuity
- Do NOT perform tonometry for IOP
- Positive Seidel’s test is indicative of globe rupture
Work-Up
- Non-contrast CT orbit
- Consider if concern for intraocular foreign body OR diagnosis is unclear
- Sensitivity ~60%
Management[3]
- Consult ophtho immediately for emergent surgical repair
- Keep NPO
- Prevent further injury
- Do not manipulate the eye
- Eye covering with metal shield (Fox shield) or paper cup (do not place a patch that touches globe)
- Minimize elevations in intraocular pressure
- Elevate head of bed
- Bed rest; no bending/lifting/Valsalva
- Consider antiemetic (e.g. ondansteron 4mg IV)
- IV pain medications PRN
- Tetanus prophylaxis (if indicated)
- If intubation necessary, use succinylcholine and ketamine <3mg/kg (do not increase intraocular pressure or cause adverse outcomes)[4]
Antibiotics[5]
NO intra-ocular foreign body
- First choice: Fluoroquinolone IV, such as Levofloxacin OR
- Second choice: Vancomycin IV and ceftazidime
Intra-ocular foreign body PRESENT
- Ceftazidime 1gm + vancomycin 1 gm
- Penicillin allergy: Ciprofloxacin + vancomycin
Children
- For children < 12 years, cefazolin 25-50 mg/kg/day in three divided doses, and gentamicin 2 mg/kg iv q8h. Gentamicin peak and trough levels are obtained one-half hour before and after the fifth dose, and BUN/Cr levels are evaluated every other day.
Disposition
- Admission for surgical repair by ophthalmology
- Transfer to tertiary trauma center if ophthalmologist prefer
See Also
References
- ↑ Layer N, et a. Algorithm for evaluation and management of the ruptured globe in an adult. Department of Ophthamology, University of California, San Francisco. http://www.icoph.org/dynamic/attachments/resources/rupturedglobeico.pdf
- ↑ Zhang Y et al. Intraocular foreign bodies in China: clinical characteristics, prognostic factors and visual outcomes in 1421 eyes. Am J Ohthalmol. 2011:152:66-73
- ↑ Layer N, et a. Algorithm for evaluation and management of the ruptured globe in an adult. Department of Ophthamology, University of California, San Francisco. http://www.icoph.org/dynamic/attachments/resources/rupturedglobeico.pdf
- ↑ Libonati MM, Leahy JJ, Ellison N: The use of succinylcholine in open eye surgery. Anesthesiology 1985; 62:637-640
- ↑ Layer N, et a. Algorithm for evaluation and management of the ruptured globe in an adult. Department of Ophthamology, University of California, San Francisco. http://www.icoph.org/dynamic/attachments/resources/rupturedglobeico.pdf