Epigastric abdominal pain
(Redirected from Epigastric pain)
Background
- This page outlines the general approach to adult epigastric pain
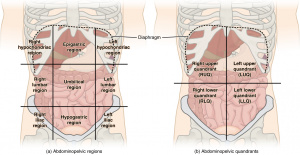
- The epigastric region contains: stomach, duodenum, pancreas, hepatic flexure, transverse colon, and the abdominal aorta
- Key EM considerations: acute coronary syndrome can present as epigastric pain (always consider in patients >40 or with cardiac risk factors), pancreatitis, peptic ulcer disease, AAA
- Epigastric pain is one of the most common presentations for atypical MI, especially in women, elderly, and diabetic patients
Classification by Abdominal pain location
| RUQ pain | Epigastric pain | LUQ pain |
| Flank pain | Diffuse abdominal pain | Flank pain |
| RLQ pain | Pelvic pain | LLQ pain |
Clinical Features
History
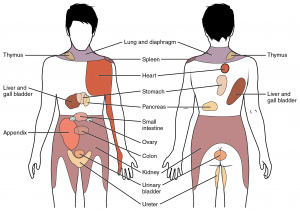
- Onset, character, radiation (back = pancreatitis, AAA; chest = ACS, GERD; right shoulder = biliary)
- Relationship to meals: postprandial (biliary, peptic ulcer), relief with eating (duodenal ulcer), worse with eating (gastric ulcer)
- Alcohol use, gallstone history (pancreatitis)
- NSAID/aspirin use (peptic ulcer disease)
- Cardiac risk factors (ACS presenting as epigastric pain)
- Melena or hematemesis (GI bleeding from ulcer or varices)
- Prior episodes
Physical Exam
- Epigastric tenderness, guarding
- Murphy sign (biliary — though usually more RUQ)
- Cullen sign (periumbilical ecchymosis) or Grey Turner sign (flank ecchymosis) — late signs of hemorrhagic pancreatitis
- Pulsatile abdominal mass (AAA)
- Absent/decreased bowel sounds
Red Flags
- Epigastric pain with diaphoresis, dyspnea, or radiation to jaw/arm (ACS)
- Hematemesis or melena (GI bleeding)
- Rigid abdomen with free air (perforated ulcer)
- Pulsatile mass (ruptured AAA)
- Severe pain radiating to back with hemodynamic instability (pancreatitis with hemorrhage or ruptured AAA)
Differential Diagnosis
Epigastric Pain
- Gastroesophageal reflux disease (GERD)
- Peptic ulcer disease with or without perforation
- Gastritis
- Pancreatitis
- Gallbladder disease
- Myocardial Ischemia
- Splenic Infarctionenlargement/rupture/aneurysm
- Pericarditis/Myocarditis
- Aortic dissection
- Hepatitis
- Pyelonephritis
- Pneumonia
- Pyogenic liver abscess
- Fitz-Hugh-Curtis Syndrome
- Hepatomegaly due to CHF
- Bowel obstruction
- SMA syndrome
- Pulmonary embolism
- Bezoar
- Ingested foreign body
Must Not Miss
- Acute coronary syndrome: atypical MI presentation — get ECG early
- Perforated peptic ulcer: free air, peritonitis
- Ruptured AAA: hypotension, pulsatile mass, elderly
- Severe pancreatitis: especially necrotizing
- Boerhaave syndrome: esophageal perforation after forceful vomiting
Evaluation
Immediate
- ECG: obtain early in all patients with epigastric pain, especially age >40 or any cardiac risk factors — inferior MI commonly presents as epigastric pain
- Bedside glucose
Laboratory
- CBC, BMP
- LFTs, lipase (>3x upper limit of normal diagnostic for pancreatitis)
- Troponin (ACS screening)
- Urinalysis
- Urine pregnancy test (females of reproductive age)
- Coagulation studies if bleeding
- Lactate if concern for ischemia or sepsis
- Type and screen if active GI bleeding
Imaging
- CXR: free air under diaphragm (perforation), mediastinal air (Boerhaave)
- RUQ US: gallstones, biliary pathology
- CT abdomen pelvis with IV contrast: pancreatitis complications, perforation, AAA, mass
- POCUS: free fluid, gallbladder, aorta (AAA screening)
- CT angiography if AAA or aortic pathology suspected
Management
- ECG first in older patients or those with risk factors — if ACS, activate cardiac protocol
- IV fluids, analgesia
- GI cocktail (antacid + viscous lidocaine +/- anticholinergic): may provide symptomatic relief for GERD/gastritis, but does NOT rule out cardiac cause even if effective
- PPI (pantoprazole) for suspected peptic ulcer or GERD
- Pancreatitis: aggressive IV fluid resuscitation, pain control, NPO initially, monitor for complications
- GI bleeding: resuscitation, PPI infusion, GI consultation for endoscopy
- Perforated ulcer: emergent surgical consultation, broad-spectrum IV antibiotics
- Ruptured AAA: emergent vascular surgery, permissive hypotension
Disposition
- Admit: pancreatitis requiring IV management, ACS, GI bleeding, perforation, biliary obstruction
- Discharge: mild gastritis/GERD with resolved symptoms, negative cardiac workup, ability to tolerate oral intake
- Follow-up: PCP in 1-2 weeks for new PPI starts; GI referral for suspected ulcer (H. pylori testing, EGD)
- Return precautions: worsening pain, vomiting blood, black stools, chest pain, lightheadedness