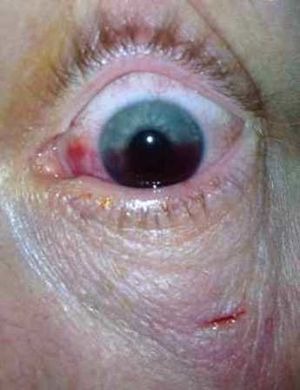
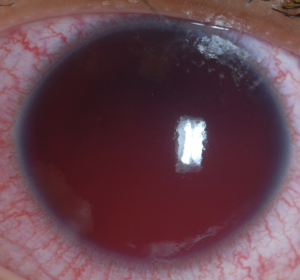
Traumatic hyphema
Background
- Grossly visible blood in the anterior chamber of the eye
- Typically caused by blunt trauma to the orbit
- Can result in permanent vision loss
- Outcome dependent on prevention of rebleeding and control of intraocular pressure
- In non-traumatic hyphema, all patients of African decent should be screened for sickle cell disease with hemoglobin electrophoresis
Clinical Features
- Vision loss
- Eye pain
- History of trauma to eye
- Direct and consensual photophobia
- Nausea/vomiting
- Hyphema grading
- Grade I: ≤ 1/3 anterior chamber volume
- Grade II: 1/3-1/2 anterior chamber volume
- Grade III: > 1/2 anterior chamber volume
- Grade IV: total anterior chamber volume, "eight ball hyphema"
- Elevated grading correlates to increase in intraocular pressure[1]
- 13.5% have IOP increase in Grade I to II
- 52% with IOP increase in Grade IV
Differential Diagnosis
Maxillofacial Trauma
- Ears
- Nose
- Oral
- Other face
- Zygomatic arch fracture
- Zygomaticomaxillary (tripod) fracture
- Related
Unilateral red eye
- Nontraumatic
- Acute angle-closure glaucoma^
- Anterior uveitis
- Conjunctivitis
- Corneal erosion
- Corneal ulcer^
- Endophthalmitis^
- Episcleritis
- Herpes zoster ophthalmicus
- Inflamed pinguecula
- Inflamed pterygium
- Keratoconjunctivitis
- Keratoconus
- Nontraumatic iritis
- Scleritis^
- Subconjunctival hemorrhage
- Orbital trauma
- Caustic keratoconjunctivitis^^
- Corneal abrasion, Corneal laceration
- Conjunctival hemorrhage
- Conjunctival laceration
- Globe rupture^
- Hemorrhagic chemosis
- Lens dislocation
- Ocular foreign body
- Posterior vitreous detachment
- Retinal detachment
- Retrobulbar hemorrhage
- Traumatic hyphema
- Traumatic iritis
- Traumatic mydriasis
- Traumatic optic neuropathy
- Vitreous detachment
- Vitreous hemorrhage
- Ultraviolet keratitis
^Emergent diagnoses
^^Critical diagnoses
Spontaneous hyphema (non-traumatic hyphema)
- Sickle cell disease
- Ocular or laser surgery
- HSV, VZV uveitis
- Neoplastic
Evaluation
evaluation is best performed under slit-lamp exam
- Blood in anterior chamber
- May only see difference in color of irises if patient is supine because blood layering is gravity dependent
- Blood in anterior chamber only visible on slit lamp is a microhyphema
- Vision loss / Acuity changes
- Inspect the lids, lashes, lacrimal ducts, and cornea
- Corneal abrasions often co-exist
- Assess direct and consensual pupillary response for the presence of a relative afferent pupillary defect
- Assess for Ruptured Globe which is associated with high energy mechanisms (shrapnel, BB guns, paintballs, etc)
- Check intraocular pressure after Globe Rupture is excluded
- Inquire about bleeding diathesis, anticoagulant/NSAID/aspirin use
Management
- Elevate head of bed and upright position to layer blood by gravity, open visual field while blood resorbs
- Eye shield
- Pharmacologic control of pain and emesis
- Weigh risks and benefits of stopping NSAIDs, ASA, anticoagulants
- If IOP elevated (>22) the treatment is similar to glaucoma management except if there is also a concern for a retrobulbar hematoma as a result of trauma.[2] Topical and oral treatments include
- Consult ophtho regarding:
- Dilation of pupil to avoid "pupillary play" -constriction and dilation movements of the iris in response to changing lighting, which can stretch the involved iris vessel causing additional bleeding
- Use of topical α-agonists and/or acetazolamide to decrease intraocular pressure (avoid acetazolamide if the patient has sickle cell disease as this increase sickling)
- Cycloplegic can be given for comfort and to decease pupillary play if globe rupture has been excluded. Options include:
- Tropicamide (Mydriacyl)
- Homatropine
- Cyclopentolate (Cyclogyl, Cylate, Pentolair)
- Scopolamine
- Topical steroid
- Treat any underlying coagulopathy
Disposition
- Should be made by the ophthalmologist after examining the patient
- Hyphemas <33% of anterior chamber are frequently managed as outpatients
- Patients being managed as an outpatient should have ophthalmologist referral and consider outpatient screening for spontaneous hyphema due to the association with sickle cell disease and hemophilia
- Patients on anticoagulation or antiplatelet agents should be admitted for reversal and observation.[2]
Discharge instructions
- No reading (accommodation may further stress injured blood vessels)
- Avoid NSAIDs
- Wear hard shield at all times
- Return to ED if rapid increase in size of hyphema or large increase in pain
Prognosis
- Rebleeding worsens prognosis as patients are at higher risk of permanent vision loss.
- Occurs 3-5 days after initial incident
- Complicates ~30% of cases
- Populations at highest risk:
- Sickle cell disease or sickle cell trait
- Bleeding dyscrasia (including aspirin, NSAID, or anticoagulant use)
- Initial intraocular pressure >22 mmHg
- Pediatric patients
| Grade | Anterior Chamber Filling | Normal Vision Prognosis |
| I | <33% | 90% |
| II | 33-50% | 70% |
| III | >50% | 50% |
| IV | 100% | 50% |
See Also
External Links
References
- ↑ Oldham GW. Hyphema. Jan 6, 2015. http://eyewiki.aao.org/Hyphema#Differential_diagnosis
- ↑ 2.0 2.1 Brandt, MT. Traumatic hyphema: a comprehensive review. Journal of oral and maxillofacial surgery. 2001; Vol. 59 Issue 12 Page 1462.