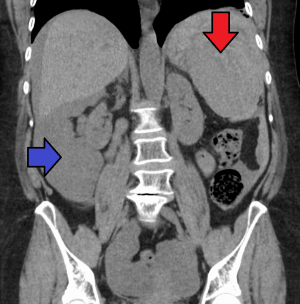
Splenic trauma
Background
- Most commonly injured visceral organ in blunt trauma
Clinical Features
- LUQ pain
- Signs of shock
- Hypotension
- Left lower rib pain
- Kehr's sign
- Acute pain in the tip of the shoulder due to the presence of blood in the peritoneal cavity when a patient's legs are elevated while laying flat.
Differential Diagnosis
Abdominal Trauma
- Abdominal compartment syndrome
- Diaphragmatic trauma
- Duodenal hematoma
- Genitourinary trauma
- Liver trauma
- Pelvic fractures
- Retroperitoneal hemorrhage
- Renal trauma
- Splenic trauma
- Trauma in pregnancy
- Ureter trauma
Evaluation
ATLS Blunt Abdominal Trauma Algorithm
- Unstable
- Stable
- CT scan
- Exploratory laparotomy, angiographic embolization, conservative management as indicated
- CT scan
AAST Criteria
| Grade | Hematoma | Laceration |
| I |
|
|
| II |
|
|
| III |
|
|
| IV |
|
|
| V |
|
|
Interactive calculators have been developed that facilitate grading of splenic injuries per AAST guidelines.[1]
Management
- Observation, angiographic embolization, or surgery depending upon:
- Hemodynamic status of the patient
- Grade of splenic injury
- Presence of other injuries and medical comorbidities
- Operative Management
- Indicated for diffuse peritonitis or hemodynamic instability after blunt abdominal trauma
- Not indicated based on injury grade alone[2]
- Nonoperative management
- Failure rate of 10-15%
- Some advocate nonoperative management only if <55yr and CT injury grade less than IV
- Should only be considered in locations with resources available for urgent laparotomy
Disposition
- Admit
See Also
References
- ↑ Spleen trauma injury score calculator- Rad At Hand
- ↑ Stassen N, Bhullar I, Cheng J, et al. Selective nonoperative management of blunt splenic injury: An Eastern Association for the Surgery of Trauma practice management guideline. J Trauma Acute Care Surg 2012; 73(5):s293-s300