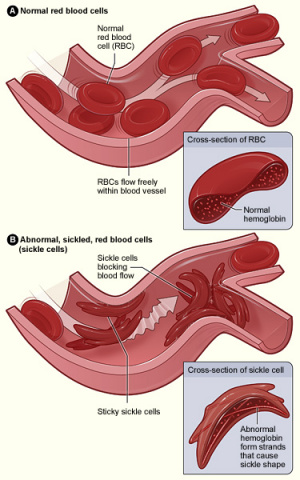
Sickle cell crisis
(Redirected from Sickle cell)
Background
Precipitating Factors
- For vaso-occlusive crisis:
- Stress
- Cold weather
- Dehydration
- Hypoxia
- Infection
- Acidosis
- Alcohol intoxication
- Pregnancy
- Exertional stress
- For aplastic crisis:
- Parvovirus B19 infection
- Folate deficiency
Clinical Features
Vaso-Occlusive Crisis[1]
See Vaso-occlusive pain crisis
Bony infarction
- More debilitating and refractory pain than past episodes
- Localized bone tenderness, elevated WBC
- Fat embolism can be complication
Dactylitis
- Tender, swollen hands/feet
- May have low-grade fever
- Occurs in <2yr old, extremely rare >5yr old
- Radiographs will show soft tissue swelling in the acute phase. Recurrent episodes can lead to a mottled appearance of hand and feet small bones on radiography. [2]
Avascular necrosis of femoral head
- Due to occlusion of blood vessel lumens, which causes microfractures, leading to collapse of cancellous bone and the articular surface
- Occurs in 30% of patients by age 30yr, prevalence increases with age
- Patients present with afebrile, inguinal pain with weight-bearing but can be asymptomatic
- Decreased ROM and pain with ambulation or passive ROM
- Other common sites of involvement are the humeral head and the area above the knee
Respiratory distress and chest pain
- Acute Chest Syndrome
- Pneumonia
- Caused by chlamydia, mycoplasma, viral, strep pneumo, staph, H. flu
- Only need blood culture in patients ill enough to require ventilator
- Asthma
- Common in patients with SCD
- Increases likelihood of acute chest syndrome by 4-6x
- Pulmonary Hypertension
- Develops in 15-35% of children with SCD
- Chest pain, DOE, hypoxia, right-sided heart failure, syncope
- Develops in 15-35% of children with SCD
- Pulmonary embolism
- Increased risk in SCD
- Consider especially if signs of DVT
Abdominal pain
- Pain crisis
- 3rd most common site of pain crisis
- Sudden onset of poorly localized abdominal pain
- May have tenderness, guarding; should not have rigidity/rebound
- Gallbladder disease (stones) is common; may occur as early as 2-4yr old
- Acute hepatic or splenic sequestration
- Labs are variable
- US or CT shows diffuse hepatomegaly or splenomegaly
- Bacterial gastroenteritis
- Increased risk for salmonella
- Consider treatment with ciprofloxacin and Bactrim in ill-appearing
Infection
- Across all ages, infection is leading cause of death
- Increased prevalence of meningitis, pneumonia, septic arthritis, osteomyelitis
- No spleen means more susceptible to encapsulated organisms
- Children aged 6mo to 3yr at greatest risk for sepsis
- Parvovirus B19
- Can cause several different syndromes:
- Erythema infectiosum ("slapped cheeks" rash)
- Gloves and socks syndrome
- Well-demarcated, painful, erythema of hands and feet
- Evolves into petechiae, purpura, vesicles, skin sloughing
- Well-demarcated, painful, erythema of hands and feet
- Arthropathy - symmetric or asymmetric, knees and ankles
- Aplastic crisis
- Reticulocyte count drops 5d post-exposure, followed by hemoglobin drop
- Can cause serious anemia which lasts for 2wk
- Can cause several different syndromes:
Musculoskeletal infection
- Patients with SCD have increased rates of bone and joint infection
- Difficult to distinguish from bony infarcts
- High fever is more typical of infection
- Limited range of motion is much more typical of infection
- Left shift is unique to infection
- ESR is unreliable
- May require bone scan or MRI to definitely distinguish infection from infarct
- Difficult to distinguish from bony infarcts
Splenic sequestration
- Major cause of mortality in <5yr old
- Labs: hemoglobin drop, no change in bili, normal to increased retic count
- 2 types: major and minor
- Major
- Rapid drop of hb (>3pt)
- Pallor, LUQ pain, splenomegaly
- Can progress within hours to altered mental status, hypotension, cardiovascular collapse
- Minor
- More insidious, smaller drop in hemoglobin
- Major
- 2 types: major and minor
Neurologic disease
- CVA is 250x more common in children with SCD
- 10% of children suffer clinically overt stroke
- 20% found to have silent CVA on imaging
- Increased rate of cerebral aneurysm and ICH
GU
Differential Diagnosis
Sickle cell crisis
- Vaso-occlusive pain crisis
- Bony infarction
- Dactylitis
- Avascular necrosis of femoral head
- Acute chest syndrome
- Asthma
- Pulmonary hypertension
- Gallbladder disease
- Acute hepatic sequestration
- Infection
- Parvovirus B19
- Splenic sequestration
- CVA
- Cerebral aneurysm and ICH
- Priapism
- Papillary necrosis
Evaluation
Work-up
Based on clinical presentation, but may include:
- CBC (assess for significant anemia)
- Reticulocyte count (<0.5% suggests aplastic crisis - rare in adults), calculating reticulocyte index
- Laboratory value is a percentage, and absolute count corrects for level of anemia
- Absolute retic count = % retics x (pt Hct / normal Hct)
- Retic index = absolute retic count / maturation factor[4]
- ≥35%, maturation factor 1.0
- 25 to <35%, maturation factor 1.5
- 20 to <25%, maturation factor 2.0
- <20%, maturation factor 2.5
- Reticulocyte index ≥2 means adequate response
- Reticulocyte index <2 suggests hypoproliferation
- Metabolic panel, lipase (if abdominal pain)
- CXR (if cough, shortness of breath, or fever)
- ECG
- VBG
- Urinalysis
- Pregnancy test
- CT brain (if symptoms of CVA)
- Note that if patient is anemic, CT non-contrast is unreliable in ruling out hemorrhagic stroke, subarachnoid hemorrhage[5]
- Will need CTA, MRI, and/or MRA
Evaluation
- Generally a clinical diagnosis
- Certain syndromes require imaging/labs for confirmation (see below)
Management
- Only use supplemental oxygen for patients who are hypoxic (<92%)
- Reserve IVF bolus for patients who are hypovolemic
- Over hydration may cause atelectasis which may precipitate Acute Chest Syndrome and hyperCl acidosis which could lead to further sickling \
- Make sure to use hypotonic fluids: 1/2NS, D5-1/2NS
Anemia
- Packed red blood cells (transfuse 10 mL/kg over 2hr period)
- Indications:
- Aplastic crisis
- Sequestration crisis
- Hemoglobin <6 with inappropriately low retic count
- Hemoglobin <10 with acute crisis (e.g. symptomatic dizziness, SOB, chest pain)
- Indications:
Vaso-occlusive pain crisis
- Analgesia
- IV opioids (morphine or hydromorphone)
- Redose in 30min if inadequate
- Non-opioid analgesia
- NSAIDs (e.g. ketorolac 15mg q6h)
- Acetaminophen
- IV/IM haloperidol or droperidol 5-10mg[6]
- Ketamine (IN 1mg/kg 1ml per nostril or IV 0.3mg/kg)[7]
- Nonpharmacologic measures (e.g. heating packs, distraction)
- IV opioids (morphine or hydromorphone)
- Hydration
- Controversial
- Dehydration promotes sickling
- IVF bolus may lead to atelectasis, pulmonary edema, and acute chest syndrome. Hyperchloremic metabolic acidosis due to normal saline may further precipitate sickling. [8] [9] [10]
- There are no randomized controlled trials that have assessed the safety and efficacy of different routes, types or quantities of fluid.[11]
- Controversial
- O2 if hypoxia; otherwise may inhibit erythropoiesis
Acute Chest Syndrome
- O2; titrate to pulse oximetry >92%
- Incentive Spirometer
- Hydration: Oral hydration preferred, IV hydration with hypotonic fluid if patient unable to tolerate PO
- Analgesia: pulmonary toilet is important but avoid excessive sedation
- Bronchodilators
- Antibiotics: 3rd generation cephalosporin + macrolide
- Transfusion (leucocyte depleted); consider transfusion to goal of hemoglobin 11 / hematocrit 30 for:
- O2 Sat <92% on room air
- hematocrit 10-20% below patient's usual hematocrit or dropping hematocrit
- Exchange transfusion; consider for:
- Progression of acute chest syndrome despite simple transfusion
- Severe hypoxemia
- Multi-lobar disease
- Previous history of severe acute chest syndrome or cardiopulmonary disease
Priapism
- Hydration
- Transfusion and/or exchange transfusion
- Urology consult
- If persists for >4-6hr:
- Aspiration of corpora
- Irrigate and infuse 1:1,000,000 epinephrine solution
Neurologic disease
- tPA is not recommended
- Exchange transfusion urgently (within 8 hours) to decrease hemoglobinS below 30%
- Hydration
Splenic sequestration
Fever
- Any fever of ≥38.5C requires empiric antibiotics (regardless of well appearance or any localized infection found)
- Ceftriaxone 50mg/kg (maximum single dose 2g)
Disposition
Consider admission to the hospital
- Fever
- Acute chest syndrome is suspected
- Sepsis, osteomyelitis, or other serious infection is suspected
- Priapism, aplastic crisis, hypoxia
- WBC >30K
- Platelet <100K
- Pain is not under control after 2-3 rounds of analgesics in ED
- <1yr old
Consider discharge
- Pain is under control and patient can take oral fluids and medications
- Ensure appropriate oral analgesics are available
- Provide home care instructions
- Ensure resource for follow-up
Medication Dosing
Pain Management
- Ketorolac 15 mg q6hr IV
See Also
References
- ↑ Lovett P. et al. Sickle cell disease in the emergency department. Emerg Med Clin North Am. 2014 Aug;32(3):629-47
- ↑ George, A., DeBaun, M., & DeBaun, M. (2021, April 28). Acute and chronic bone complications of sickle cell disease. Retrieved April 20, 2022, from https://www.uptodate.com/contents/acute-and-chronic-bone-complications-of-sickle-cell-disease?search=sickle%20cell%20disease%20children&topicRef=110699&source=see_link
- ↑ George, A., DeBaun, M., & DeBaun, M. (2021, April 28). Acute and chronic bone complications of sickle cell disease. Retrieved April 20, 2022, from https://www.uptodate.com/contents/acute-and-chronic-bone-complications-of-sickle-cell-disease?search=sickle%20cell%20disease%20children&topicRef=110699&source=see_link
- ↑ Poorana PP and Subhashree AR. Role of Absolute Reticulocyte Count in Evaluation of Pancytopenia-A Hospital Based Study. J Clin Diagn Res. 2014 Aug; 8(8): FC01–FC03.
- ↑ Lyon M et al. Approach to the diagnosis and treatment of acute subarachnoid hemorrhage in a patient with sickle cell disease. Am J Emerg Med. 2015 Mar;33(3):481.e3-4.
- ↑ *Lyness, D., & Motov, S. (2016, July 7). CERTA Opioid Alternatives and Analgesics. Retrieved July 25, 2016, from http://www.propofology.com/infographs/certa-opioid-alternatives-as-analgesics
- ↑ *Lyness, D., & Motov, S. (2016, July 7). CERTA Opioid Alternatives and Analgesics. Retrieved July 25, 2016, from http://www.propofology.com/infographs/certa-opioid-alternatives-as-analgesics
- ↑ Glassberg, J., Evidence-based management of sickle cell disease in the emergency department.Emerg Med Pract, 2011. 13(8): p. 1-20
- ↑ Carden, M.A., et al., Variations in pediatric emergency medicine physician practices for intravenous fluid management in children with sickle cell disease and vaso-occlusive pain: A single institution experience.Pediatr Blood Cancer, 2018. 65(1)
- ↑ Carden, M.A., et al., Normal Saline Bolus Use in Pediatric Emergency Departments is Associated with Worse Pain Control in Children with Sickle Cell Anemia and Vaso-occlusive Pain.Am J Hematol, 2019.
- ↑ Okomo U, Meremikwu MM. Fluid replacement therapy for acute episodes of pain in people with sickle cell disease. Cochrane Database of Systematic Reviews 2015, Issue 3. Art. No.: CD005406. DOI: 10.1002/14651858.CD005406.pub4