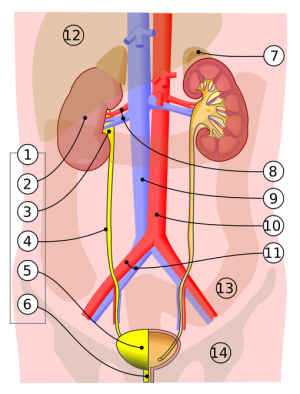
Urolithiasis
Background
- Urolithiasis comprises 3 similar clinical entities:
- Nephrolithiasis
- Ureterolithiasis
- Cystolithiasis
- The most common cause is infection of residual bladder urine with urea-splitting organisms (Proteus, Pseudomonas, Klebsiella, Staphylococcus,Mycoplasma, Providentia stuartii, Serratia, and Morganella morganii)
- Promoters of stone formation [1]
- High serum calcium
- High uric acid and phosphate
- Urine pH abnormalities, either high or low
- Inhibitors of stone formation [2]
- Citrate
- Magnesium
- Various macromolecules
Renal damage
- Irreversible renal damage can occur within 3 weeks in patients with a complete obstruction
- Most have no rise in creatinine because unobstructed kidney functions at up to 185% of its baseline capacity
Epidemiology
- 1-15% lifetime incidence
- More common in males
- 50% recurrence rate within 5-10 years
- More common in hot dry climates
Infection
- 8-15% of kidney stones have urinary co-infection[3]
- Fever, pyuria >10 WBC/hpf, and peripheral WBC >11.3 (any one) best predictors of concomitant UTI[3]
Stone Expulsion Rate
| Stone Size | Passage Rate[4] |
| 1-4 mm | 78% |
| 5 -7 mm | 60% |
| >8mm | 39% |
Types
- Calcium (~80%): Mostly calcium oxylate >> calcium phosphate
- Hyperparathyroidism, hypercalcemia of malignancy, sarcoidosis, increased absorption, loop diuretics, IBD
- The remainder
- Struvite (magnesium ammonium phosphate)
- Associated with infection with urease-producing bacteria such as Proteus, klebsiella, pseudomonas, staph,Providentia stuartii, Serratia, and Morganella morganii
- Uric Acid
- 25% of patients with gout develop kidney stones
- Cystine
- Multiple types of crystals
- Struvite (magnesium ammonium phosphate)
Risk Factors for Complications
- Renal function at risk
- DM
- Hypertension
- HIV
- Renal insufficiency
- Single kidney
- Horseshoe kidney
- Transplanted kidney
- History of difficulty with stones
- Extractions
- Stents
- Ureterostomy tubes
- Lithotripsy
- Symptoms of infection
- Fever
- Hypotension
- Systemic illness
- UTI
- Immunosuppression
Clinical Features
- Pain
- Acute onset, crampy, intermittent, unable to find position of comfort
- Location of pain depends on location of stone:
- Upper ureter: flank pain
- Mid ureter: lower anterior quadrant of abdomen
- Distal ureter: groin pain
- UVJ: Can mimic a UTI (frequency, urgency, dysuria)
- Nausea/vomiting (50%)
- Hematuria (85%)
Differential Diagnosis
Nephrolithiasis is most common misdiagnosis given to patients with rupturing AAA
Flank Pain
- Vascular
- Abdominal aortic aneurysm
- Renal artery embolism
- Renal vein thrombosis
- Aortic dissection
- Mesenteric ischemia
- Renal
- Pyelonephritis
- Perinephric abscess
- Perinephric hematoma
- Papillary necrosis
- Renal cell carcinoma
- Obstructive uropathy
- May or may not be due to nephrolithiasis
- Renal infarction
- Renal hemorrhage
- Ureter
- Nephrolithiasis
- Blood clot
- Stricture
- Tumor (primary or metastatic)
- Bladder
- Tumor
- Varicose vein
- Cystitis
- GI
- Biliary colic
- Pancreatitis
- Perforated peptic ulcer
- Appendicitis (appendix may be pushed to RUQ in pregnancy)
- Inguinal Hernia
- Diverticulitis
- Cancer
- Bowel obstruction
- Gynecologic
- Ectopic Pregnancy
- PID/TOA
- Ovarian cyst
- Ovarian torsion
- Endometriosis
- Mittelschmerz or benign ovulatory pain
- GU
- Other
- Shingles
- Lower lobe pneumonia
- Retroperitoneal hematoma, abscess, or tumor
- Epidural abscess
- Epidural hematoma
- Rib contusion/fracture
Lower Back Pain
- Spine related
- Acute ligamentous injury
- Acute muscle strain
- Disk herniation (Sciatica)
- Degenerative joint disease
- Spondylolithesis
- Epidural compression syndromes
- Thoracic and lumbar fractures and dislocations
- Cancer metastasis
- Spinal stenosis
- Transverse myelitis
- Vertebral osteomyelitis
- Ankylosing spondylitis
- Spondylolisthesis
- Discitis
- Spinal Infarct
- Renal disease
- Intra-abdominal
- Abdominal aortic aneurysm
- Ulcer perforation
- Retrocecal appendicitis
- Large bowel obstruction
- Pancreatitis
- Pelvic disease
- Other
Evaluation
Labs
- Urinalysis: hematuria
- Urine culture :
- Urine pregnancy
- Chemistry
- BUN/Cr to evaluate renal function
- CBC: If concern for infection (>15k concerning)
Imaging
- Consider tailoring your choice of imaging based upon the patient's age, clinical likelihood of stones, risk factors, and prior history of stones[8]
- In young patients, even with no prior history of kidney stones, reasonable approaches may be bedside ultrasound or no imaging
- In middle aged patients with prior history of stones, it may be reasonable to perform a bedside ultrasound although no imaging can be appropriate as well
- In middle aged patients with no prior history of stones, CT imaging is reasonable
- In elderly patients, even with prior history of stones, CT is recommended in order to avoid missing alternative etiologies such as dissection, AAA, or diverticulitis.
- Bedside Renal ultrasound
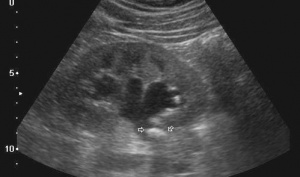
- Consider non-contrast CT abdomen and pelvis (KUB protocol) for:
- 1st time stone
- Older patients with other possible diagnosis
- Avoid CT in young (<50 years old), health patients with known history of nephrolithiasis with presentation consistent with renal colic[9]
- Consider formal ultrasound for:
- Pregnant pt
- Repeat stone (to avoid CT)
- In comparison of diagnosis by CT vs. U/S (by EP) vs. U/S (by radiologist):[10]
- No difference in rate of missed high-risk diagnoses that resulted in complications (pyelo/sepsis/diverticular abscess)
- No difference in rate of serious adverse events, pain scores, return emergency department visits, or hospitalizations
Imaging Findings
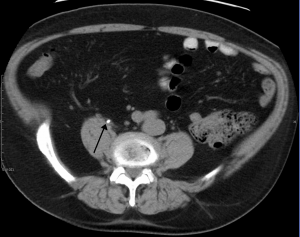
- CT Imaging
- Hydronephrosis
- Hydroureter
- Hydrocalyx
- Note: Hydronephrosis, hydroureter, hydrocalyx alone indicate obstructive uropathy, stone must be seen or collected (if passed) in order to diagnose nephrolithiasis as the etiology.
- Perinephric Stranding
- Location Landmarks
- Renal: Does not cause pain, and usually considered an incidental finding
- UPJ: Ureteropelvic Junction
- UVJ Ureterovesicular Junction
Management
Pain
- Ketorolac 15mg IV or Ibuprofen 600mg PO Q6hrs PRN if the patient can tolerate oral medications[11]
- Avoid high dose NSAIDS in patients with renal failure or insufficiency.
- Ketorolac 15 mg has similar effects to the traditional 30 mg dosage. [12]
- Morphine or other Opioids
- Severe pain not controlled with NSAIDS
- Contraindications to NSAIDS
- eGFR <30 mL/min
Antiemetic
Expulsion Therapy
- Consider Tamsulosin 0.4mg PO QHS (discontinued after successful expulsion; average 1-2 weeks)
- The American Urological Association (AUA) advocates the use of medical expulsive therapy in the form of alpha-blockers (tamsulosin) for uncomplicated distal ureteric stones ≤10 mm (Strong recommendation). The EAU suggests that alpha-blockers be used only in distal ureteric stones >5 mm because a large randomized controlled trial demonstrated no benefit in using alpha-blockers for distal ureteric stones of <5 mm.[13]
- See EBQ:Alpha-blockers for ureteral stone expulsion discussion of evidence
- 76% vs 48% passage rates in tamsulosin vs no treatment, respectively[14]
- Only patients with stones ≥ 5 mm benefited
- Review of 55 RTCs, with NNT of 4
- Tamsulosin number needed to harm (orthostatic hypotension)= 19 (give at night, to reduce side effect rate)[7]
- Use of IV fluids to "flush out" stone has NOT been shown to improve clinical outcomes[7]
Infected Urolithiasis
Inpatient observation is often the safest disposition for patients with infected stones due to the risk of progressing to sepsis. All antibiotics should take into account patient's previous sensitivities and local antibiograms. Treatment is targeted at E. coli, Enterococcus, Klebsiella, Proteus mirabilis, S. saprophyticus.
Outpatient
Consider one dose of Ceftriaxone 1g IV or Gentamicin 7mg/kg IV if the regional susceptibility of TMP/SMX or Fluoroquinolones is <80%
- Ciprofloxacin 500mg PO BID x7 days OR
- Trimethoprim-Sulfamethoxazole DS 160/800mg PO BID x14 days OR[15]
- Cephalexin 500mg QID PO x 10-14 days (OR consider 1000mg BID) OR
- Cefdinir 300mg BID PO x 10-14 days OR
- Cefpodoxime 200mg PO BID x 10 days OR[16]
- Cefixime 400mg PO daily x 10 days OR[17]
- Levofloxacin 750mg PO QD x7 days[18]
Adult Inpatient Options
- Ciprofloxacin 400mg IV q12hr OR
- Ceftriaxone 1gm IV QD (Preferred in pregnancy) OR
- Cefotaxime 1-2gm IV q8hr OR
- Gentamicin 3mg/kg/day divided q8hr +/- ampicillin 1–2 gm q4hr OR
- Piperacillin/Tazobactam 3.375 gm IV q6hr OR
- Cefepime 2gm IV q8hr OR
- Imipenem/Cilastatin 500mg IV q8hr
Pediatric Outpatient Options
- Cephalexin 25-50mg/kg/day PO divided q6-8h x 10-14 days (max 500mg/dose) OR
- Cefixime 8mg/kg PO daily x 10-14 days (max 400mg) OR
- Cefdinir 14mg/kg/day PO divided BID x 10 days (max 600mg/day) OR
- Cefpodoxime 10mg/kg/day PO divided BID x 10 days (max 200mg/dose) OR
- TMP/SMX 6-12mg/kg/day (TMP) PO divided BID x 10-14 days
Pediatric Inpatient Options
- Ceftriaxone 75mg/kg IV QD OR
- Cefotaxime 50mg/kg IV q8hrs OR
- Ampicillin 25mg/kg IV q6hrs + 2.5mg/kg IV q8hrs
- Ampicillin/Sulbactam 3g IM/IV q6 hours x 14 days
Surgical Removal
Considered for ureterolithiasis with:
- Persistent obstruction
- Failure of stone progression
- Increasing or unremitting colic
- Staghorn calculi
Medication Dosing
Ketorolac 15mg IV — 15mg has similar efficacy to 30mg; avoid in renal failure Ibuprofen 600mg Q6hrs PRN PO — Avoid in renal failure or insufficiency Tamsulosin 0.4mg QHS PO
Disposition
Admission
Recommended for any of the following:
- Intractable pain or vomiting[7]
- Proximal urinary tract infection,[7] as evidence by:
- Single or transplanted kidney with obstruction[7]
- Acute renal failure[7]
- Hypercalcemic Crisis
Also consider admission for patients with:
- Solitary kidney or transplanted kidney without obstruction
- Urinary extravasation
- Significant medical comorbidities
Consultation
- Renal insufficiency
- Severe underlying disease
- Stone >10 mm[7]
- Sloughed renal papillae
- Unclear/distal UTI
- Ruptured renal capsule causing urinoma
- pregnancy
- children
Discharge
- Small stone in patient with adequate analgesia and able to arrange urology follow up within 7d
See Also
References
- ↑ Wang Z, Zhang Y, Zhang J, Deng Q, Liang H. Recent advances on the mechanisms of kidney stone formation (Review). Int J Mol Med. 2021 Aug;48(2):149. doi: 10.3892/ijmm.2021.4982. Epub 2021 Jun 16. PMID: 34132361; PMCID: PMC8208620.
- ↑ Wang Z, Zhang Y, Zhang J, Deng Q, Liang H. Recent advances on the mechanisms of kidney stone formation (Review). Int J Mol Med. 2021 Aug;48(2):149. doi: 10.3892/ijmm.2021.4982. Epub 2021 Jun 16. PMID: 34132361; PMCID: PMC8208620.
- ↑ 3.0 3.1 3.2 Abrahamian FM, et al. Association of pyuria and clinical characteristics with presence of urinary tract infection among patients with acute nephrolithiasis. Annals of EM. 2013; 62(5):526-533.
- ↑ Coll DM et al. Relationship of spontaneous passage of ureteral calculi to stone size and location as revealed by unenhanced helical CT. AJR Am J Roentgenol 2002 Jan; 178:101-3.
- ↑ Teichman JM. Clinical practice. Acute renal colic from ureteral calculus. N Engl J Med. 2004 Feb 12;350(7):684-93. doi: 10.1056/NEJMcp030813. PMID: 14960744.
- ↑ Wang Z, Zhang Y, Zhang J, Deng Q, Liang H. Recent advances on the mechanisms of kidney stone formation (Review). Int J Mol Med. 2021 Aug;48(2):149. doi: 10.3892/ijmm.2021.4982. Epub 2021 Jun 16. PMID: 34132361; PMCID: PMC8208620.
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 7.7 7.8 7.9 Wang RC. Managing Urolithiasis. Annals of EM. April 2016. 67(4):449-454
- ↑ Imaging in suspected renal colic: systematic review of the literature and multispecialty consensus Moore CL, Carpenter CR, Heilbrun ME, et al. Ann Emerg Med. 2019;74(3):391-399.
- ↑ Part of Choosing wisely ACEP
- ↑ Smith-Bindman R, Aubin C, Bailitz J, et al. Ultrasonography versus computed tomography for suspected nephrolithiasis. NEJM. 2014; 371(12):1100–1110.
- ↑ Pathan, SA et al. Delivering safe and effective analgesia for management of renal colic in the emergency department: a double-blind, multi-group, randomised controlled trial. Lancet. 2016 May 14;387(10032): 1999-2007
- ↑ Motov S, et al. Comparison of Intravenous Ketorolac at Three Single-Dose Regimens for Treating Acute Pain in the Emergency Department: A Randomized Controlled Trial. Ann Emerg Med. 2017 Aug;70(2):177-184. doi: 10.1016
- ↑ Hughes T, Ho HC, Pietropaolo A, Somani BK. Guideline of guidelines for kidney and bladder stones. Turk J Urol. 2020 Nov;46(Supp. 1):S104-S112. doi: 10.5152/tud.2020.20315. Epub 2020 Oct 9. PMID: 33052834; PMCID: PMC7731951.
- ↑ Hollingsworth JM et al. α-blockers for treatment of ureteric stones: systematic review and meta-analysis. BMJ 2016;355:i6112.
- ↑ Gupta K, Hooton TM, Naber KG, et al. International Clinical Practice Guidelines for the Treatment of Acute Uncomplicated Cystitis and Pyelonephritis in Women. Clinical Infectious Diseases. 2011;52(5):e103-e120. doi:10.1093/cid/ciq257
- ↑ Colgan R, Williams M. Diagnosis and treatment of acute uncomplicated cystitis. Am Fam Physician. 2011 Oct 1;84(7):771-6.
- ↑ Acute Pyelonephritis in Adults. Johnson, JR and Russo, TA. New England Journal of Medicine 2018; 378:48-59.
- ↑ Sandberg T. et al. Ciprofloxacin for 7 days versus 14 days in women with acute pyelonephritis: a randomised, open-label and double-blind, placebo-controlled, non-inferiority trial. Lancet. 2012 Aug 4;380(9840):484-90.