Mallory-Weiss tear
Background
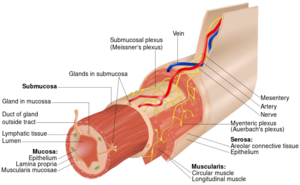
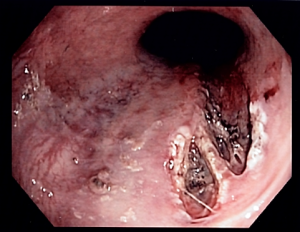
- Longitudinal lacerations through mucosa and submucosa
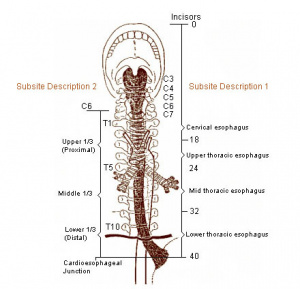
- 75% in proximal stomach, rest in distal esophagus
- Due to sudden increase in intrabdominal pressure
- Typically in the setting of forceful vomiting or retching
Clinical Features
Risk Factors
- Hiatal hernia
- Alcoholism
- Anything that increases intrabdominal pressure: blunt abdominal trauma, CPR, etc.
History
- Classic presentation: Hematemesis following vomiting or retching
- As few as 30% of patients present this way
- Coffee ground emesis
- Melena
- Hematochezia
Differential Diagnosis
Upper gastrointestinal bleeding
- Peptic ulcer disease (most common cause)
- Gastritis/esophagitis
- Gastric/esophageal varices
- Mallory-Weiss tear
- Malignancy
- Aortoenteric fisulta
- Boerhaave
- Dieulafoy's lesion
- Angiodysplasia
- Hemobilia
- Hemorrhagic gastritis, EtOH
- Celiac disease
- Dengue
- Other intrabdominal bleeds
- Lower GI bleeding
- Hemorrhagic pancreatitis
- Splenic rupture
- Subcapsular cavernous hemangiomas
- Peliosis hepatis
Mimics of GI Bleeding
- Hemoptysis
- Vaginal/Urethra bleeding
- ENT bleeding
- Dietary (Iron, bismuth, beets)
- Swallowed maternal blood (in neonate)
Evaluation
- Approach as any GI bleed
- CBC
- BMP
- Type and screen
- Guiac
- CXR
- Definitive diagnosis by endoscopy
Management
- Most Mallory-Weiss tears are minor and resolve on their own, but up to 3% of upper gastrointestinal bleeding deaths are a result of Mallory-Weiss tears
- Endoscopy only for active and on-going bleeding[1]
- Treat as undifferentiated upper GI bleed
- Many of these patients are alcoholics and have cirrhosis; consider esophageal varices
- History of vomiting/retching; consider boerhaave
Treatments Not Supported by the Literature
- No evidence to support octreotide use
Disposition
- Anticipate admission
See Also
External Links
References
- ↑ Gyawali CP. The Washington Manual Gastroenterology Subspecialty Consult 2ed. 2008. Washington University School of Medicine.