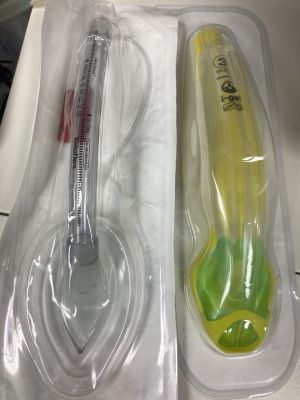
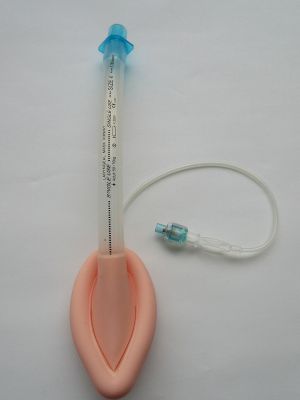
Supraglottic airway
(Redirected from Laryngeal mask airway)
Indications
- Need for positive pressure ventilation (PPV)
- Field intubation by paramedics, especially in pediatric patients[3][4]
Contraindications
Absolute
- Spontaneous respirations
- Gag reflex
Relative
- Significant facial trauma
Difficult Supraglottic Device (RODS)
- Restricted mouth opening
- Obstruction
- Distorted airway
- Stiff lungs (chronic pulmonary disease, obesity) or neck (C-spine collar, limited neck extension)
Equipment Needed
- Supraglottic Airway (SGA) device (many options exist, see below)
- Appropriate sedation/paralytic agents, if indicated
LMA Sizes[5]
| Mask Size | Weight (kg) | Age (yr) | LMA Length (cm) | LMA Cuff Vol (mL) | Largest ETT^ (mm) |
| 1 | <5 | <0.5 | 10 | 4 | 3.5 |
| 1.5 | 5-10 | <1 | 10 | 5-7 | 4 |
| 2 | 6.5-20 | 1-5 | 11.5 | 7-10 | 4.5 |
| 2.5 | 20-30 | 5-10 | 12.5 | 14 | 5 |
| 3 | 30-60 | 10-15 | 19 | 15-20 | 6 |
| 4 | 60-80 | >15 | 19 | 25-30 | 6.5 |
| 5 | >80 | >15 | 19 | 30-40 | 7 |
^Largest ETT that can pass thorough "Intubating LMA" (ILMA)
iGel Sizes
| igel size | patient size | weight (kg) |
| 1 | neonate | 2-5 |
| 1.5 | infant | 5-12 |
| 2 | smal pediatric | 10-25 |
| 2.5 | large pediatric | 25-35 |
| 3 | small adult | 30-60 |
| 4 | medium adult | 50-90 |
| 5 | large adult | 90+ |
Procedure
Due to variety of devices and placement techniques, impossible to give exact universal procedure
- Prepare patient as for intubation
- If patient is awake, provide topical anesthetic
- Place supraglottic airway device by one of the following techniques:
- Use thumb or index finger to guide device along midline of hard palate with cuff deflated or partially inflated and advance until seated
- Insert device with cuff facing hard palate, then rotate 180 degrees while advancing (similar to OPA insertion)
- Insert laterally 45 degrees against tongue, advance and rotate to midline
- Inflate cuff (if applicable)
- Confirm placement as with endotracheal tube
Intubating LMA[6]
- Prepare patient as for intubation
- Partially deflate the cuff of the iLMA and lubricate
- Holding iLMA by metal handle only, insert into patient's mouth with the posterior surface of the iLMA against the hard palate
- Advance the iLMA until it is seated
- Inflate the iLMA cuff
- Ventilate patient and confirm placement as usual
- Lubricate endotracheal tube
- Insert ETT into the aperture on the iLMA
- Slide ETT to appropriate depth
- Inflate ETT cuff and confirm placement as usual
- Disconnect adaptor from ETT
- Deflate iLMA cuff
- Use obturator to push against ETT while slowly removing iLMA
- Grasp ETT in the oral cavity as soon as able
- When iLMA is fully removed, reattach ETT adaptor
- Ventilate patient and confirm placement as usual
Complications[1]
- Bronchospasm
- Hoarseness
- Laryngeal nerve injury
- Hypoglossal nerve injury
- Pharyngeal edema
- Dysphagia
Special Considerations
- There are 2 generations of supraglottic airway devices[7][2]
- 1st Gen = classic LMA, other standard LMAs
- 2nd Gen = iGel, LMA Supreme, Pro-Seal LMA (PLMA)
- Second generation devices achieve improved esophageal and pharyngeal seal (causes ↑ oropharyngeal leak pressure), incorporate a "drain tube" that allows access to the esophagus and stomach, and usually have an incorporated bite block.
- Oropharyngeal leak pressure = the applied pressure at which the seal between the device and the larynx begins to leak.
- Peak inspiratory pressure needs to be less than the oropharyngeal leak pressure for effective ventilation and to prevent gastric insufflation.[8]
- Higher failure rate with obese patients, inappropriate patient position (e.g. trendelenberg), and placement by inexperienced provider[2]
- The AIRWAYS-2 trial found no significant difference in 30-day outcomes between initial use of SGAs and tracheal intubation during out-of-hospital cardiac arrest. However, it noted that SGAs had a higher initial ventilation success rate compared to tracheal intubation [9]
See Also
Airway Pages
- Pre-intubation
- Induction
- Intubation
- Surgical airways
- Post-intubation
External Links
- Merk Manual - How To Insert a Laryngeal Mask Airway
- Merk Manual - How To Insert an Esophageal-Tracheal Double Lumen Tube (Combitube®) or a King Laryngeal Tube
Videos
- Laryngeal Mask Airway (https://www.youtube.com/watch?v=-oXa-f5qkGY)
- I-Gel (https://www.youtube.com/watch?v=YuG6k6ndBpM)
- King Airway (https://www.youtube.com/watch?v=yJGuxDny_fo)
References
- ↑ 1.0 1.1 Apfelbaum JL, et al.; American Society of Anesthesiologists Task Force on Management of the Difficult Airway. Practice guidelines for management of the difficult airway: an updated report by the American Society of Anesthesiologists Task Force on Management of the Difficult Airway. Anesthesiology. 2013 Feb;118(2):251-70
- ↑ 2.0 2.1 2.2 Major complications of airway management in the UK: results of the Fourth National Audit Project of the Royal College of Anaesthetists and the Difficult Airway Society. Cook TM, Woodall N, Frerk C; Fourth National Audit Project. Br J Anaesth. 2011 May;106(5)
- ↑ Zhu X-Y, Lin B-C, Zhang Q-S, Ye H-M, Yu R-J. A prospective evaluation of the efficacy of the laryngeal mask airway during neonatal resuscitation. Resuscitation. 2011;82(11):1405–1409. doi:10.1016/j.resuscitation.2011.06.010
- ↑ Calkins MD, Robinson TD. Combat trauma airway management: endotracheal intubation versus laryngeal mask airway versus combitube use by Navy SEAL and Reconnaissance combat corpsmen. J Trauma. 1999;46(5):927–932
- ↑ Tarascon Adult Emergency Pocketbook
- ↑ https://calsprogram.org/manual/volume2/Section5_AirwaySkills/09-AirSk8IntubLarynMaskAirway13.html
- ↑ Timmermann, A. Supraglottic airways in difficult airway management: successes, failures, use and misuse. Anaesthesia, 2011, 66(Suppl. 2), pages 45–56.
- ↑ Patel B., Bingham R. Laryngeal mask airway and other supraglottic airway devices in paediatric practice. Contin Educ Anaesth Crit Care Pain (2009) 9 (1): 6-9.
- ↑ Benger JR, et al. Supraglottic airway device versus tracheal intubation in the initial airway management of out-of-hospital cardiac arrest: the AIRWAYS-2 cluster RCT. Health Technol Assess. 2022;26(21):1-158. doi:10.3310/VHOH9034