Hypertriglyceridemia
Background
- ~5% of acute pancreatitis caused by high triglycerides[1]
- Etiologies
- Familial hypertriglyceridemia, autosomal dominant with variable penetrance
- Secondary forms
- DM, obesity, EtOH, estrogen therapy
- Hypothyroidism, ESRD, nephrotic syndrome, HIV, anti-HIV meds
- TG levels > 2000mg/dL almost always have both secondary and genetic form[2]
- 1.7% of US estimated to have [TG] between 500-2000[3]
- May present with normal serum lipase levels
Pathophysiology
- Excess TG hydrolyzed by increased concentration of pancreatic lipase
- Produces increased concentration of free fatty acids that exceeds binding capacity of albumin
- Micelles are formed that attack platelets, vascular endothelium and acinar cells
- Ischemia and pancreatic injury result
- An acidic environment potentiates free fatty acid toxicity
Clinical Features
General
- Most are generally asymptomatic until sequelae present
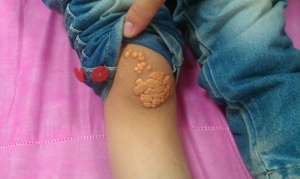
- Eruptive xanthoma may be found on dermatologic exam
Hypertriglyceridemic Pancreatitis
Signs/symptoms of pancreatitis
- Pain is the most common symptom and is often characterized by:
- Persistent
- Localizes to epigastric area, around waist, RUQ, or occasionally LUQ
- Radiates to back
- The onset may be less abrupt and the pain poorly localized
- Nausea/vomiting noted in most
- Abdominal distention is frequent complaint
- Cullen sign (ecchymosis of periumbilical region) - intrabdominal hemorrhage
- Turner sign (ecchymosis of flanks) - retroperitoneal hemorrhage
- Pulmonary Findings
Differential Diagnosis
Epigastric Pain
- Gastroesophageal reflux disease (GERD)
- Peptic ulcer disease with or without perforation
- Gastritis
- Pancreatitis
- Gallbladder disease
- Myocardial Ischemia
- Splenic Infarctionenlargement/rupture/aneurysm
- Pericarditis/Myocarditis
- Aortic dissection
- Hepatitis
- Pyelonephritis
- Pneumonia
- Pyogenic liver abscess
- Fitz-Hugh-Curtis Syndrome
- Hepatomegaly due to CHF
- Bowel obstruction
- SMA syndrome
- Pulmonary embolism
- Bezoar
- Ingested foreign body
Evaluation
- Triglycerides; Severely elevated (at least >500 mg/dL, generally >1,000 mg/dL)
- Lipids in serum may interfere with other lab tests
- Falsely low Na+, amylase
- Lipids in serum may interfere with other lab tests
Pancreatitis workup
- Rule out other causes of pancreatitis (e.g. gallstone pancreatitis)
- In general, if triglycerides >1000, can assume this is cause of pancreatitis
- Lipase level >3x upper limit of normal
- Sensitivity 82-100%, specificity 82-100%[4]
- Negative lipase does not exclude pancreatitis in chronic/recurrent disease
- Absolute value not associated with prognosis or severity
- Characteristic findings on ultrasound or CT
Management
Management of acute pancreatitis in the setting of hypertriglyceridemia
- Evidence for management based on case series and reports[5][6]
- Insulin drip - most dramatic and rapid intervention, with reduction within 24 hrs
- Initiate at 0.1 units/kg/hr (similar to treatment for DKA)
- Goal is to reduce triglycerides to < 500
- Add D5NS if glucose drops < 200 [7]
- Monitor BMP q2 hr
- Manage potassium
- K < 3.2 stop insulin and replete K
- K 3.3 to 5 add 20 mEq K/Lto IVF
- K > 5 no extra potassium
- IVF as for standard pancreatitis treatment, add potassium as per above
- Treat concurrent hypothyroidism if present
- Pain control
- Niacin 500mg QD
- Gemfibrozil or fenofibrate
- Max dose statin, 81mg ASA
- Heparin q8 SC, effect short-lived
- NPO initially
- May advance diet starting at TG level < 1000mg/dL with resolution of abdominal pain/pancreatitis symptoms
- No fat diet
- Low calorie diet
Plasma exchange
- Therapeutic plasma exchange, for 1-3 days (sickest patients)
- Generally indicated for hypocalcemia, persistent elevated lactic acidosis, other signs of worsening organ dysfunction
- For euglycemic patients, not routine first line
- Requires central venous access
Disposition
- Asymptomatic hypertriglyceridemia is treated as an outpatient
- For acute pancreatitis, ICU or step-down for frequent labs, insulin drip
See Also
External Links
References
- ↑ Yadav D, Pitchumoni CS. Issues in hyperlipidemic pancreatitis. J Clin Gastroenterology 2003;36:54-62.
- ↑ Yuan et al. Hypertriglyceridemia: its etiology, effects and treatment. CMAJ 2007;176:1113-1120.
- ↑ Brown, Virgil W. Et al. “Clinical Lipidology Roundtable Discussion: Severe Hypertriglyceridemia.” Journal of Clinical Lipidology 2012; 6:397-408
- ↑ Yadav D, Agarwal N, Pitchumoni CS. A critical evaluation of laboratory tests in acute pancreatitis. Am J Gastroenterol. 2002 Jun;97(6):1309-18.
- ↑ Santana YR et al. Treatment of severe hypertriglyceridemia with continuous insulin infusion. Case Reports in Critical Care. June 2011.
- ↑ Poonuru S et al. Rapid Reduction of Severely Elevated Serum Triglycerides with Insulin Infusion, Gemfibrozil and Niacin. Clin Med Res. 2011 Mar; 9(1): 38–41.
- ↑ Schaefer EW. Management of Severe Hypertriglyceridemia in the Hospital: A Review. Journal of Hospital Medicine Vol 7|No 5|May/June 2012.