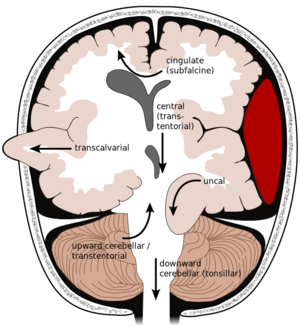
Brain herniation syndromes
(Redirected from Herniation Syndromes)
Background
- Brain herniation occurs when increased intracranial pressure causes brain tissue to shift across rigid dural structures (falx, tentorium) or through the foramen magnum
- Represents a life-threatening neurological emergency requiring immediate recognition and intervention
- Most commonly caused by mass lesions (intracranial hemorrhage, tumor, abscess) or diffuse cerebral edema
Types
Uncal (Lateral Transtentorial)
- Most common clinically significant herniation pattern
- Medial temporal lobe (uncus) herniates over the tentorial edge
- Classic triad: ipsilateral blown pupil (third nerve palsy), contralateral hemiparesis, decreased consciousness
- Contralateral hemiparesis occurs ~75% of the time (ipsilateral Kernohan notch phenomenon in ~25%)
- May progress to bilateral fixed dilated pupils and posturing if untreated
Central Transtentorial
- Both cerebral hemispheres herniate downward through the tentorium
- Progressive rostral-to-caudal deterioration:
- Early: small reactive pupils, Cheyne-Stokes respiration, increased tone
- Late: midpoint fixed pupils, extensor posturing, loss of brainstem reflexes
Cerebellotonsillar (Tonsillar)
- Cerebellar tonsils herniate through foramen magnum → brainstem compression
- Pinpoint pupils
- Sudden respiratory and cardiovascular collapse
- Flaccid quadriplegia
- Most rapidly fatal herniation pattern
Upward (Ascending) Transtentorial
- Posterior fossa mass pushes cerebellum upward through tentorial notch
- Pinpoint pupils, downward conjugate gaze
- Obstructive hydrocephalus may occur
Subfalcine
- Cingulate gyrus herniates under the falx cerebri
- May compress anterior cerebral artery → contralateral leg weakness
- Often clinically silent early but may progress to other herniation patterns
Clinical Features
- Decreasing GCS
- Unilateral or bilateral pupil dilation and fixation
- Abnormal posturing (decorticate → decerebrate)
- Cushing reflex: hypertension, bradycardia, irregular respirations (late finding)
- Loss of brainstem reflexes (corneal, gag, oculocephalic)
- Respiratory pattern changes (Cheyne-Stokes → central neurogenic hyperventilation → ataxic → apnea)
Management
- ABCs — secure airway early; avoid hypoxia and hypotension
- Elevate head of bed 30 degrees, keep head midline
- Hyperosmolar therapy:
- Mannitol 1-1.5 g/kg IV bolus
- Hypertonic saline (23.4%) 30 mL IV over 10-20 min via central line (or 3% saline 250-500 mL via peripheral line)
- Hyperventilation to PaCO2 30-35 mmHg (temporary bridge — effect lasts 15-20 min)
- Emergent neurosurgery consult for surgical decompression or EVD placement
- Treat underlying cause (evacuate hematoma, treat cerebral edema)
- Avoid hyperthermia, hyperglycemia, seizures
Disposition
- All patients with brain herniation require emergent ICU admission
- Neurosurgical consultation is mandatory
- Consider emergent operative intervention for:
- Epidural hematoma with herniation signs
- Large subdural hematoma with midline shift
- Obstructive hydrocephalus
- Transfer to neurosurgical center if unavailable on site
- Goals of care discussion appropriate for devastating injuries
See Also
- Elevated intracranial pressure
- Head trauma (main)
- Intracranial hemorrhage (main)
- Glasgow Coma Scale (GCS)