High altitude cerebral edema
(Redirected from HACE)
Background
- Also known as HACE
- Progressive neurologic deterioration in someone with acute mountain sickness or HAPE (due to ↑ ICP)
- Least common form of acute mountain sickness
- Typically occurs three to five days after arrival of high elevation
- Almost never occurs at <8,000ft (~2000m)
Clinical Features
- Will have clinical features of acute mountain sickness before HACE, as HACE is a progression from AMS
- Altered mental status, ataxia, gait disturbance, stupor (most sensitive findings)
- Ataxia at high altitude is cerebral edema until proven otherwise
- Progresses to coma if untreated
- Uncertain mechanism, presumed cause is hypoxia leading to cerebral edema
- Headache, nausea/vomiting (not always present)
- Focal neuro deficits may be seen (3rd/6th CN palsies)
- Seizures are rare
Differential Diagnosis
High Altitude Illnesses
- Acute mountain sickness
- Chronic mountain sickness
- High altitude cerebral edema
- High altitude pulmonary edema
- High altitude peripheral edema
- High altitude retinopathy
- High altitude pharyngitis and bronchitis
- Ultraviolet keratitis
- Dehydration
- Exhaustion
- Hypoglycemia
- Hypothermia
- Hyponatremia
- Carbon monoxide poisoning
- Stroke
- Meningitis
- Encephalitis
- CNS lesion
- Intoxication
Evaluation
- The Lake Louise Consensus Criteria for HACE
- The presence of a change in mental status OR ataxia in a person with AMS
- OR the presence of BOTH a change in mental status and ataxia in a person without AMS
- Lumbar puncture is not required, but if performed, will generally show elevated opening pressures (>44 mmH2O) and normal fluid analysis[1]
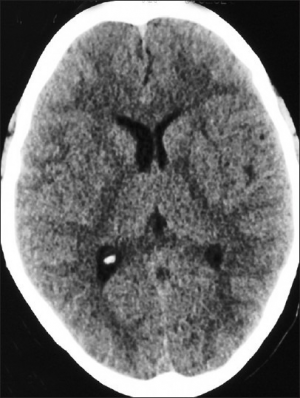
- CT or MRI may be confirmatory, but not necessary. Most beneficial to rule out alternative etiologies. If performed, may show signs of vasogenic edema. MRI will show white matter edema (increased T2 signal), particularly in the corpus callosum[2]
Expected SpO2 and PaO2 levels at altitude[3]
| Altitude | SpO2 | PaO2 (mm Hg) |
|---|---|---|
| 1,500 to 3,500 m (4,900 to 11,500 ft) | about 90% | 55-75 |
| 3,500 to 5,500 m (11,500 to 18,000 ft) | 75-85% | 40-60 |
| 5,500 to 8,850 m (18,000 to 29,000 ft) | 58-75% | 28-40 |
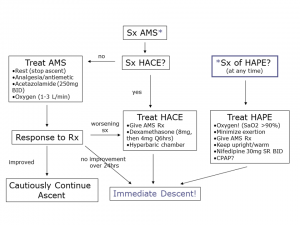
Management
- Immediate descent is the treatment of choice
- If descent not possible use combination of:
- Supplemental O2 (goal SpO2 90%)[4]
- Supportive hyperventilation
- Dexamethasone 8mg initially (PO, IM, or IV), then 4mg q6hr
- Acetazolamide 250mg BID (better as ppx)
- Hyperbaric bag (Gamow bag) if available
- Of note, furosemide, mannitol, and oral glycerol have all been studied but have undetermined effectiveness at this time.
Prevention
- Acclimatization, slow ascent
- Acetazolamide 125mg BID (250mg BID if greater than 100kg)
- Dexamethasone 4mg q6h PO or IV
Medication Dosing
Dexamethasone 8mg initially, then 4mg q6hr PO/IM/IV Acetazolamide 250mg BID PO
Disposition
- Admission for close monitoring, neurological checks
- Recovery ranges from 2 to 21 days with 25% of patients recovering within 48 hours
See Also
References
- ↑ Medical Aspects of Harsh Environments Vol 2: Textbook of Military Medicine Series. Published by The US Army office of the surgeon general 2002. (Text, review)
- ↑ Hackett PH, Yarnell PR, Hill R, Reynard K, Heit J, McCormick J. High-altitude cerebral edema evaluated with magnetic resonance imaging: clinical correlation and pathophysiology. JAMA. 1998;280(22):1920-1925.
- ↑ Gallagher, MD, Scott A.; Hackett, MD, Peter (August 28, 2018). "High altitude pulmonary edema". UpToDate. Retrieved May 2, 2019.
- ↑ Hackett PH, Roach RC. High altitude cerebral edema. High Alt Med Biol 2004; 5:136-146.