Intubation
(Redirected from Endotracheal intubation)
This page is for adult patients. For pediatric patients, see: intubation (peds)
Indications
- Failure to ventilate
- Failure to oxygenate
- Inability to protect airway
- Gag reflex is absent at baseline in ~1/3 of people[1], so lack of gag reflex is inadequate in determination of ability to protect airway.
- If a patient is able to tolerate placement of an oropharyngeal airway, they likely require intubation for airway protection
- GCS <8 generally an indication for intubation in trauma patients
- Anticipated clinical course (anticipated deterioration, need for transport, or impending airway compromise)
- Combative patient who needs imaging (suspicion of intracranial process, etc)
Considerations
- 2015 AHA ACLS guidelines deemphasize placement of advanced airway placement in initial resuscitation
- Out-of-hospital arrest data suggests lower survival of those intubated in field[2]
- 108,000 patients examined in U.S. registry of inpatient hospital arrests, with 95% of intubations occurring within 15 min of resuscitation[3]
- Patients intubated were significantly less likely to survive to discharge, 16% vs. 19%
- Also less likely to be discharged with good functional status, 11% vs. 14%
Absolute Contraindications
- No absolute contraindications when performed as an emergent procedure
- Exception: cannot ventilate and anticipate near impossible orotracheal intubation, strongly consider awake fiberoptic intubation (if possible) and also performing a surgical airway as a back up plan
Relative Contraindications
See Predicting the difficult airway
Difficult BVM (MOANS)
- Mask seal
- Obesity
- Aged
- No teeth
- Stiffness (resistance to ventilation)
Difficult Intubation (LEMON)
- Look externally (gestalt)
- Evaluate 3-3-2 rule
- Mallampati
- Obstruction
- Neck mobility
Equipment Needed
- Medications
- Induction agent
- Paralytic agent
- Pre-oxygenation devices (nasal cannula, non-rebreather, bag valve mask, etc.)
- Oropharyngeal/nasopharyngeal airway for difficult to ventilate patients
- Leave nasal cannula on for apneic oxygenation if possible
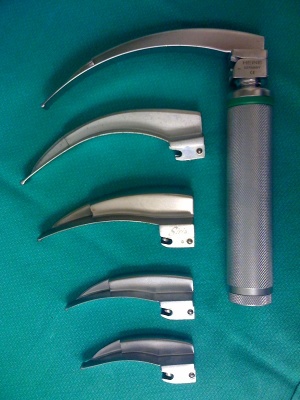
- Laryngoscope (type based on clinical indication and provider preference)
- Direct laryngoscope with blade of provider's choice or
- Video laryngoscope (Glidescope, C-Mac, KingVision, etc.) or
- Optical stylet (Shikani, Levitan, etc.) or
- Fiberoptic device
- Endotracheal tube
- End-tidal CO2 device (colorimetric or quantitative)
- Ventilator
- Suction
- Intubation adjuncts (bougie, lighted stylet, etc)
- Ensure you have correct stylet for type of laryngoscope you are using
- Direct or Mactintosh-blade videolaryngoscopes require malleable stylets
- Hyperangulated videolaryngoscopes require rigid stylets
- Ensure you have correct stylet for type of laryngoscope you are using
- Bag valve mask
SOAP-ME Checklist Mnemonic
- Suction
- Oxygen
- Nasal cannula
- Non-rebreather
- Bag-valve mask
- Airways
- Endotracheal tube
- Rescue devices
- Adjuncts
- Positioning
- Medications
- Equipment
- Laryngoscope
- EtCO2
- Bougie
Procedure
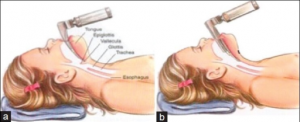
Direct laryngoscopy (with Macintosh blade)
- Place patient into sniffing position
- Use "scissor" technique with right hand to open mouth
- Insert laryngoscope blade into right side of mouth
- Slowly advance blade into mouth while performing "tongue sweep"
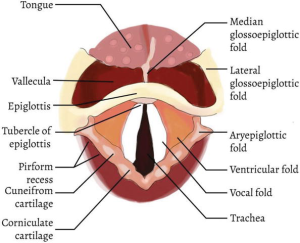
- Identify epiglottis
- Advance tip of blade into vallecula
- Lift upward and away from operator to expose glottis
- Deliver tube through vocal cords
Video laryngoscopy
- Hyperangulated video laryngoscope
- Patient ideally in neutral spine position (as opposed to "sniffing" position for direct laryngoscopy)
- After induction, use right hand to "scissor" mouth open
- Place hyperangulated blade midline and slowly advance with progressive identification of airway landmarks
- Advance blade into vallecula
- When cords fill entire screen (Cormack-Lehane Grade I), slightly retract laryngoscopy so that cords only occupy upper 1/3 of screen (CL Grade II, allows for passage of ETT with rigid stylet)[4]
- If intubation is attempted with the best view possible, operators often have difficulty advancing the tube around the tongue and hypopharyngeal soft tissues
- Standard geometry video laryngoscope
- Same technique utilized with direct laryngoscopy
- Can either visualize directly or utilize video screen for tube delivery
Post-Procedure
- Confirm tube placement with auscultation and end tidal CO2[5]
- Secure tube
- Place OG to decompress stomach
- Provide sedation and analgesia
- Head of bed to at least 30°
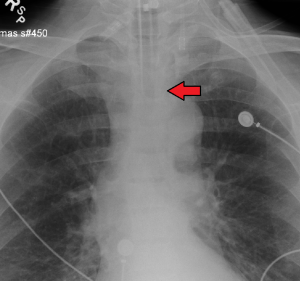
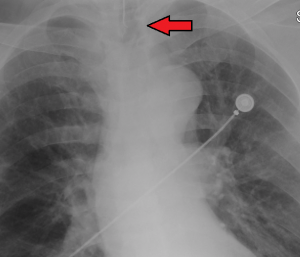
- Obtain CXR
- Tube should be 3-5 cm from the carina
- Check ABG ~30 minutes after intubation
- Check cuff pressures - should be between 20-30 cm H2O
- Check plateau pressure using "inspiratory hold" - should be less than 30 cm H2O
Initial ventilation settings
| Disease | Tidal Volume (mL/kg^) | Respiratory Rate | I:E | PEEP | FiO2 |
| Traditional | 8 | 10-12 | 1:2 | 5 | 100% |
| Lung Protective (e.g. ARDS) | 6 | 12-20 | 1:2 | 2-15 | 100% |
| Obstructive (e.g. bronchoconstriction) | 6 | 5-8 | 1:4 | 0-5 | 100% |
| Hypovolemic | 8 | 10-12 | 1:2 | 0-5 | 100% |
Complications
Special Situations
Severe Metabolic Acidosis
Further drop in pH during intubation can be catastrophic
- NIV (SIMV Vt 550, FiO2 100%, Flow Rate 30 LPM, PSV 5-10, PEEP 5, RR 0)
- SIMV on ventilator, not NIV machine
- "Pseudo-SIMV" mode
- Attach end-tidal CO2 and observe value
- Push RSI medications
- Turn the respiratory rate to 12
- Perform jaw thrust
- Wait 45sec
- Intubate
- Re-attach the ventilator
- Immediately increase rate to 30
- Change Vt to 8cc/kg
- Change flow rate to 60 LPM (normal setting)
- Make sure end-tidal CO2 is at least as low as before
Active GI Bleed
- Empty the stomach
- Place an NG and suction out blood
- Varices are not a contraindication
- Metoclopramide 10mg IV
- Increases LES tone
- Place an NG and suction out blood
- Intubate with HOB at 45°
- Preoxygenate!
- Want to avoid bagging if possible
- Intubation meds
- Use sedative that is BP stable with lower dose (etomidate, ketamine)
- Use paralytics with higher dose (actually increases LES tone)
- If need to bag:
- Bag gently and slowly (10BPM)
- Consider placing LMA
- If patient vomits
- Place in Trendelenberg
- Place LMA
- Use meconium aspirator
- If patient aspirates anticipate a sepsis-like syndrome
- May need pressors, additional fluid (not antibiotic!)
See Also
Airway Pages
- Pre-intubation
- Induction
- Intubation
- Surgical airways
- Post-intubation
Mechanical Ventilation Pages
- Noninvasive ventilation
- Intubation
- Mechanical ventilation (main)
- Miscellaneous
External Links
- EMCrit Podcast – Ventilatory Kills – Intubating the patient with Severe Metabolic Acidosis
- First 10 EM: Intubation
Videos
- Hippo ED (12:50) https://www.youtube.com/watch?v=-M3OlfmKjO8
References
- ↑ Davies AE, Kidd D, Stone SP, MacMahon J. Pharyngeal sensation and gag reflex in healthy subjects. Lancet. 1995 Feb 25;345(8948):487-8.
- ↑ Hasegawa K et al. Association of prehospital advanced airway management with neurologic outcome and survival in patients with out-of-hospital cardiac arrest. JAMA 2013 Jan 16; 309:257.
- ↑ Angus DC.Whether to intubate during cardiopulmonary resuscitation: Conventional wisdom vs big data. JAMA 2017 Feb 7; 317:477.
- ↑ Gu Y, Robert J, Kovacs G, et al. A deliberately restricted laryngeal view with the GlideScope® video laryngoscope is associated with faster and easier tracheal intubation when compared with a full glottic view: a randomized clinical trial. Une vue laryngée délibérément restreinte à l'aide du vidéolaryngoscope GlideScope® est associée à une intubation trachéale plus rapide et plus aisée qu'une vue glottique totale: une étude clinique randomisée. Can J Anaesth. 2016;63(8):928-937. doi:10.1007/s12630-016-0654-6
- ↑ Scott Weingart, MD FCCM. Podcast 84 – The Post-Intubation Package. EMCrit Blog. Published on October 16, 2012. Accessed on January 16th 2021. Available at [1].