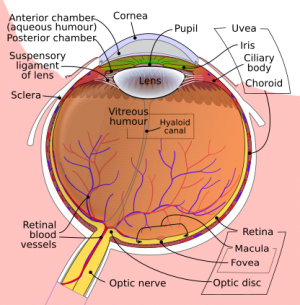
Corneal laceration
For full-thickness corneal lacerations see globe rupture
Background
- Traumatic injury to the eye, most often associated with penetrating injury or impact with debris.[1]
- Must rule out full-thickness corneal laceration (i.e., globe rupture), which is a medical emergency
Clinical Features
- Foreign body sensation
- Photophobia (+/- consensual)
- Decreased vision
- If associated iritis or if abrasion occurs in visual axis
- Eye pain
- Relief of pain with topical anesthesia
Differential Diagnosis
Unilateral red eye
- Nontraumatic
- Acute angle-closure glaucoma^
- Anterior uveitis
- Conjunctivitis
- Corneal erosion
- Corneal ulcer^
- Endophthalmitis^
- Episcleritis
- Herpes zoster ophthalmicus
- Inflamed pinguecula
- Inflamed pterygium
- Keratoconjunctivitis
- Keratoconus
- Nontraumatic iritis
- Scleritis^
- Subconjunctival hemorrhage
- Orbital trauma
- Caustic keratoconjunctivitis^^
- Corneal abrasion, Corneal laceration
- Conjunctival hemorrhage
- Conjunctival laceration
- Globe rupture^
- Hemorrhagic chemosis
- Lens dislocation
- Ocular foreign body
- Posterior vitreous detachment
- Retinal detachment
- Retrobulbar hemorrhage
- Traumatic hyphema
- Traumatic iritis
- Traumatic mydriasis
- Traumatic optic neuropathy
- Vitreous detachment
- Vitreous hemorrhage
- Ultraviolet keratitis
^Emergent diagnoses
^^Critical diagnoses
Evaluation
Workup
- A complete eye exam should be conducted
- Eyelid Exam
- Flip upper lid and exam lower lid for foreign body
- If concern for foreign body despite normal exam, consider orbital CT (or MRI if certain foreign body is nonmetallic)
- Fluorescein Exam
- Apply 1 gtt of flourescein or use strip with anesthetic
- Use Wood's lamp or slit lamp with cobalt blue light
- Fluorescein will fill corneal defects and glow
- Multiple vertical abrasions suggests foreign body embedded under the upper lid
- Topical anesthetic (i.e., proparacaine or tetracaine) may assist in patient cooperation with exam once open globe excluded.
- Repeated doses or prescriptoin for topical anesthesia is controversial given concerns for impaired healing
Corneal laceration (non full-thickness) vs Globe Rupture
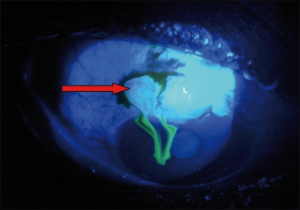
Positive Seidel’s test (see globe rupture).
- Fluorescein Examination
- Seidel sign (streaming of fluorescein) indicates globe rupture
- If high-risk metallic foreign body injury (e.g., hammering a nail, grinding metal), perform ocular CT on all patients
- Normal ocular pressure (do not perform if high suspicion of globe rupture) supports simple (non full-thickness) corneal laceration diagnosis
Diagnosis
- Typically determined on clinical exam +/- ocular CT (if high risk)
Management
See globe rupture for full thickness lacerations.
Antibiotics
Does Not Wear Contact Lens
- Erythromycin ointment qid x 3-5d OR
- Ciprofloxacin 0.3% ophthalmic solution 2 drops q6 hours OR
- Ofloxacin 0.3% solution 2 drops q6 hours OR
- Sulfacetamide 10% ophthalmic ointment q6 hours
Wears Contact Lens
Antibiotics should cover pseudomonas and favor 3rd or 4th generation fluoroquinolones
- Levofloxacin 0.5% solution 2 drops ever 2 hours for 2 days THEN q6hrs for 5 days OR
- Moxifloxacin 0.5% solution 2 drops every 2 hours for 2 days THEN q6hrs for 5 days OR
- Tobramycin 0.3% solution 2 drops q6hrs for 5 days OR
- Gatifloxacin 0.5% solution 2 drops every 2 hours for 2 days THEN q6hrs for 5 days OR
- Gentamicin 0.3% solution 2 drops six times for 5 days
Pediatric
Same topical regimens as adults
- Erythromycin 0.5% ointment applied QID x 3-5 days (preferred in young children)
- Moxifloxacin 0.5% ophthalmic solution 1-2 drops QID x 5 days
Analgesia
- Systemic NSAIDs or opioids
- Cycloplegics can be consider for patients with large abrasions (>2mm) and/or severe pain
- Cyclopentolate 1% 1 drop q6-8hr
- Ophthalmic NSAIDs
- Ketorolac 0.4% 1 drop q6hr x 2-3d
- Topical anesthetics
- Tetracaine 1% 1 drop q30min has been found to be safe in the first 24 hrs[2]
- Proparacaine 0.05% ophthalmic (dilute 1 mL of proparacaine 0.5% with 9 mL of NS in flush syringe then place 3 mL in bottle) 1-2 drops in eye Q30 min PRN pain for 24-48 hours only[3]
Other
- Tetanus prophylaxis not indicated (unless penetrating injury)[4]
- Patch is not routinely recommended[5] and can prolong healing time[6]
Disposition
(Assuming no globe rupture)
- Ophtho follow up in 48h for routine cases
See Also
External Links
References
- ↑ [1], Ramirez DA. Ocular Injury in United States Emergency Departments: Seasonality and Annual Trends Estimated from a Nationally Representative Dataset. Am J Ophthalmol. 2018;191:149-155.
- ↑ Waldman N, et al. Topical tetracaine used for 24 hours is safe and rated highly effective by patients for the treatment of pain caused by corneal abrasions: a double-blind, randomized clinical trial. Acad Emerg Med. 2014; 21(4):374-82.
- ↑ Salim Rezaie, "Topical Anesthetic Use on Corneal Abrasions", REBEL EM blog, April 21, 2014. Available at: https://rebelem.com/topical-anesthetic-use-corneal-abrasions/.
- ↑ Mukherjee P, et al. Tetanus prophylaxis in superficial corneal abrasions. Emerg Med J. 2003; 20:62-64.
- ↑ Flynn CA, et al. Should we patch corneal abrasions? A meta-analysis. J Fam Pract. 1998; 47(4):264-70.
- ↑ Fraser, S. Corneal abrasion. Clin Ophthalmol. 2010; 4:387-390.