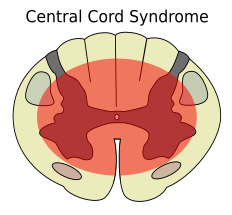
Central cord syndrome
Background
- Most common incomplete spinal cord injury (accounts for ~9% of all traumatic spinal cord injuries)
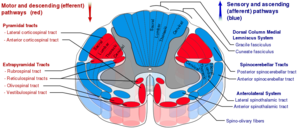
- Injury to the central gray matter and medial portions of the corticospinal tracts
Etiology
- Classic: Elderly patient with pre-existing cervical spondylosis/spinal stenosis who sustains a hyperextension injury (e.g., ground-level fall)
- Ligamentum flavum buckles inward → cord contusion of central gray matter
- May occur without fracture or dislocation (important — can have normal plain films/CT)
- Young patients: high-energy trauma with cervical fracture/dislocation
- Non-traumatic: syringomyelia (progressive, chronic onset), central canal ependymoma
Clinical Features
- Upper extremity weakness > lower extremity weakness (hallmark finding)
- Due to somatotopic organization of corticospinal tract: upper extremity fibers are medial (central), lower extremity fibers are lateral (peripheral)
- Sacral sparing — distinguishes incomplete from complete injury:
- Intact toe flexion
- Intact perianal sensation
- Normal rectal tone
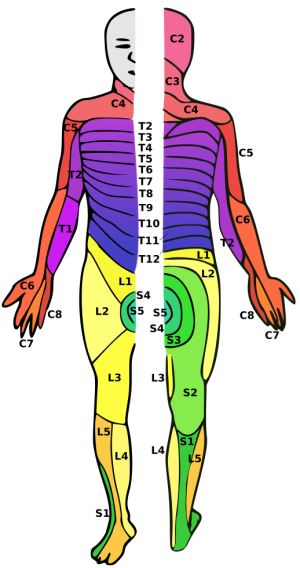
- Variable sensory deficits: pain/temperature loss in cape-like distribution (upper extremities > lower)
- +/- bladder dysfunction, urinary retention
Differential Diagnosis
Spinal Cord Syndromes
- Complete spinal cord transection syndrome
- Anterior cord syndrome
- Central cord syndrome
- Brown-Séquard syndrome
- Epidural compression syndromes
Evaluation
- MRI of cervical spine — gold standard; shows cord edema/contusion, pre-existing stenosis
- CT cervical spine — may show spondylosis, stenosis, fracture
- Key pearl: May have normal CT in elderly patients with low-energy mechanism — always obtain MRI if clinical suspicion is high
- Neurological exam: document motor levels, sensory levels, rectal tone (ASIA scoring)
Management
Acute Management of Spinal Cord Injury
- Neurogenic shock management
- Consider intubation injuries at C5 or above
- Manual in-line stabilization reduces cervical movement better than C-collar, but be careful of tracheal pressures inadvertently applied which can worsen laryngeal visualization[1][2]
- Direct laryngoscopy causes C-spine extension at atlanto-occipital junction, C1-C2, and C4-C7 in order from most to least
- Consider video laryngoscopy with hyperangulated stylet or bougie assisted DL to intubate higher-grade laryngoscopy views of vocal cords without C-spine overextension[3]
- Post-intubation sedation takes into consideration hemodynamics and potential intraoperative EMG and evoked potential monitoring by anesthesia
- Consider surgical intervention for:
- Progressive neurologic deficits
- Unstable spine fractures
- Steroids are no longer recommended
Administration of methylprednisolone (MP) for the treatment of acute spinal cord injury (SCI) is not recommended. Clinicians considering MP therapy should bear in mind that the drug is NOT approved by the FDA for this indication. There is no Class I or Class II medical evidence supporting the clinical benefit of MP in the treatment of acute SCI. Scattered reports of Class III evidence claim inconsistent effects likely related to random chance or selection bias. However, Class I, II, and III evidence exists that high-dose steroids are associated with harmful side effects including death.
[6]- See EBQ:High Dose Steroids in Cord Injury for further discussion
- Early surgical decompression within 24 hours is safe and effective for patients with cord compression
- Mean arterial pressure goal ≥85 mmHg to maintain spinal cord perfusion
Prognosis
- Best prognosis of all incomplete cord syndromes (>50% regain ambulatory function)
- Lower extremities recover first, then bladder, then upper extremities
- Fine hand motor function recovers last and often incompletely
Disposition
- Admit all patients with acute spinal cord injury
- Neurosurgery consult for surgical decompression timing
- Surgery within 24 hours is safe and effective, but may be extended to <2 weeks after injury
See Also
References
- ↑ The effect of laryngoscopy of different cervical spine immobilisation techniques. Heath KJ. Anaesthesia. 1994 Oct; 49(10):843-5.
- ↑ Manual in-line stabilization increases pressures applied by the laryngoscope blade during direct laryngoscopy and orotracheal intubation. Santoni BG, Hindman BJ, Puttlitz CM, Weeks JB, Johnson N, Maktabi MA, Todd MM. Anesthesiology. 2009 Jan; 110(1):24-31.
- ↑ Cervical spinal motion during intubation: efficacy of stabilization maneuvers in the setting of complete segmental instability. Lennarson PJ, Smith DW, Sawin PD, Todd MM, Sato Y, Traynelis VC. J Neurosurg. 2001 Apr; 94(2 Suppl):265-70.
- ↑ Improvement of motor-evoked potentials by ketamine and spatial facilitation during spinal surgery in a young child. Erb TO, Ryhult SE, Duitmann E, Hasler C, Luetschg J, Frei FJ. Anesth Analg. 2005 Jun; 100(6):1634-6.
- ↑ Effects of dexmedetomidine on intraoperative motor and somatosensory evoked potential monitoring during spinal surgery in adolescents. Tobias JD, Goble TJ, Bates G, Anderson JT, Hoernschemeyer DG. Paediatr Anaesth. 2008 Nov; 18(11):1082-8.
- ↑ Hurlbert RJ et al. Pharmacological therapy for acute spinal cord injury. Neurosurgery. 2013 Mar;72 Suppl 2:93-105 http://www.ncbi.nlm.nih.gov/pubmed/23417182