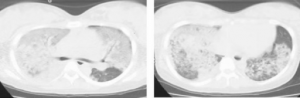
Amniotic fluid embolus
Background
- Maternal mortality rate ~80%
- 85% of survivors have neurologic sequelae
- Occurs in 2-8 per 100,000 deliveries[1]
- Responsible for ~10% of maternal mortality in US
Risk Factors
- Cesarean delivery
- Advanced maternal age
- Abnormal placental implantation
- Uterine rupture
- Eclampsia
- Amniocentesis
- Trauma
Clinical Features
- Typically occurs during labor and delivery or 30 minutes after delivery
- Any of the following:
Differential Diagnosis
3rd Trimester/Postpartum Emergencies
- Acute fatty liver of pregnancy
- Amniotic fluid embolus
- Chorioamnionitis
- Eclampsia
- HELLP syndrome
- Mastitis
- Peripartum cardiomyopathy
- Postpartum endometritis (postpartum PID)
- Postpartum headache
- Postpartum hemorrhage
- Preeclampsia
- Resuscitative hysterotomy
- Retained products of conception
- Septic abortion
- Uterine rupture
Evaluation
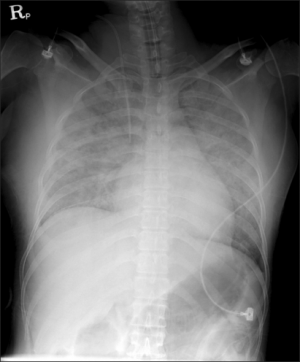
Post cesarean chest X-ray in a patient with acute amniotic fluid embolus.
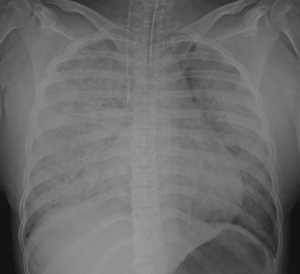
Chest X-ray with diffuse infiltration throughout the lungs in a patient with acute amniotic fluid embolus.
- Diagnosis of exclusion
- Consider CXR and/or chest CT
Management
- Treat hypoxia (may require intubation)
- Treat hypotension → Pressors / blood products
- Avoid hypoperfusion → Place patient in left lateral decubitus position
- Immediate delivery of fetus → Emergent c-section
- Resuscitative hysterotomy within 5min of cardiac arrest if mother cannot be resuscitated
A-OK Medications
Only case reports have described the following three therapies[2]
- Atropine - 1mg IV
- Vagolytic properties may help
- Ondansetron 8 mg IV
- Blocking of serotonin receptors can inhibits the release of more inflammatory mediators.
- Ketorolac - 30mg IV
- Can block thromboxane production and prevent coagulopathies.
Disposition
- Admit
See Also
References
- ↑ Fong A, Chau CT, Pan D, et al. Amniotic fluid embolism: antepartum, intrapartum and demographic factors. J Matern Fetal Neonatal Med. 2014 Jun 30. 1-6.
- ↑ Rezai S. et al. Atypical Amniotic Fluid Embolism Managed with a NovelTherapeutic Regimen Case Reports in Obstetrics and Gynecology. 2017. https://www.researchgate.net/profile/Shadi_Rezai/publication/312332674_Atypical_Amniotic_Fluid_Embolism_AFE_Managed_With_A_Novel_Therapeutic_Regimen/links/5a3b50da458515a77aa99a21/Atypical-Amniotic-Fluid-Embolism-AFE-Managed-With-A-Novel-Therapeutic-Regimen.pdf