Acute flaccid myelitis: Difference between revisions
| Line 28: | Line 28: | ||
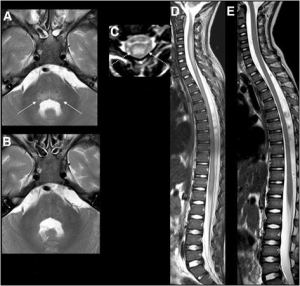
<small>(Spinal cord lesions may not be present on initial MRI if performed within the first 72 hours of onset of acute limb weakness.)</small> | <small>(Spinal cord lesions may not be present on initial MRI if performed within the first 72 hours of onset of acute limb weakness.)</small> | ||
[[File:MRI Brain and Spinal Cord in a child with Acute Flaccid Myelitis.png|thumb <ref>https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5234096/</ref>]] | [[File:MRI Brain and Spinal Cord in a child with Acute Flaccid Myelitis.png|thumb| <ref>https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5234096/</ref>]] | ||
==Management<ref>http://www.cdc.gov/acute-flaccid-myelitis/downloads/acute-flaccid-myelitis.pdf</ref>== | ==Management<ref>http://www.cdc.gov/acute-flaccid-myelitis/downloads/acute-flaccid-myelitis.pdf</ref>== | ||
Revision as of 05:07, 17 May 2019
Background
- Polio-like illness, subset of transverse myelitis
- More common in children
- Likely caused by:
- Enterovirus, particularly Enterovirus D68, poliovirus
- West nile virus
- Adenovirus
Clinical Features[1]
- Acute onset, focal weakness of 1 or more extremity
- Decreased muscular tone
- Absent or hypoactive reflexes
- Rarely have numbness, but may have some neuropathic pain
- Fever and other symptoms of infection by causative virus (e.g. URI symptoms, gastroenteritis)
- In severe cases:
- Bulbar dysfunction (dysphagia, dysarthria, dysphonia, facial weakness, ptosis)
- Respiratory muscle weakness
- Autonomic instability, arrythmias if cervical lesion present
- Paralysis usually maximal at 3-5 days after onset
Differential Diagnosis
Weakness
- Neuromuscular weakness
- Upper motor neuron:
- CVA
- Hemorrhagic stroke
- Multiple sclerosis
- Amyotrophic Lateral Sclerosis (ALS) (upper and lower motor neuron)
- Lower motor neuron:
- Spinal and bulbar muscular atrophy (Kennedy's syndrome)
- Spinal cord disease:
- Infection (Epidural abscess)
- Infarction/ischemia
- Trauma (Spinal Cord Syndromes)
- Inflammation (Transverse Myelitis)
- Degenerative (Spinal muscular atrophy)
- Tumor
- Peripheral nerve disease:
- Neuromuscular junction disease:
- Muscle disease:
- Rhabdomyolysis
- Dermatomyositis
- Polymyositis
- Alcoholic myopathy
- Upper motor neuron:
- Non-neuromuscular weakness
- Can't miss diagnoses:
- ACS
- Arrhythmia/Syncope
- Severe infection/Sepsis
- Hypoglycemia
- Periodic paralysis (electrolyte disturbance, K, Mg, Ca)
- Respiratory failure
- Emergent Diagnoses:
- Symptomatic Anemia
- Severe dehydration
- Hypothyroidism
- Polypharmacy
- Malignancy
- Aortic disease - occlusion, stenosis, dissection
- Other causes of weakness and paralysis
- Acute intermittent porphyria (ascending weakness)
- Can't miss diagnoses:
Evaluation
- Evaluate for other causes of symptoms (e.g. HSV, bacterial meningitis, Guillain-Barre syndrome)
- CSF: Pleocytosis (WBC count >5 cells/mm3), +/- elevated protein
- MRI: spinal cord lesion, largely restricted to gray matter, spanning one or more spinal segments
(Spinal cord lesions may not be present on initial MRI if performed within the first 72 hours of onset of acute limb weakness.)
Management[3]
- Report suspected cases to CDC/department of health
- Respiratory:
- Consider intubation for airway protection if evidence of bulbar dysfunction
- Consider NIPPV if evidence of respiratory muscle weakness (by clinical exam, hypoxia, hypercarbia, vital capacity <15 mL/kg, or NIF <30)
- Treat neuropathic pain
- Elevate head of bed >30 degrees
- No evidence of benefit from corticosteroids, IVIG, plasmapheresis, or antivirals as of yet
Disposition
- Admit
- Consider ICU admission for:
- Respiratory muscle weakness
- Bulbar weakness causing impaired airway protection
- Altered mental status
- Autonomic instability
- Cervical lesion on MRI
- Rapidly progressive course
See Also
External Links
https://wwwn.cdc.gov/nndss/conditions/acute-flaccid-myelitis/case-definition/2018/