Open-angle glaucoma: Difference between revisions
| Line 2: | Line 2: | ||
==Background== | ==Background== | ||
[[File:Schematic diagram of the human eye en.png|thumb|Eye anatomy.]] | [[File:Schematic diagram of the human eye en.png|thumb|Eye anatomy.]] | ||
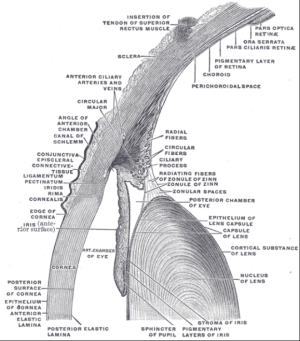
[[ File:Gray883.png|thumb|Eye angle anatomy.]] | |||
[[File:PMC4614311 qmj-2015-01-0006-g002.png|thumb|Mechanism of open vs closed angle closure glaucoma.]] | |||
*Elevated intraocular pressure and resulting optic nerve damage manifested initially as visual field loss and ultimately irreversible blindness if left untreated | *Elevated intraocular pressure and resulting optic nerve damage manifested initially as visual field loss and ultimately irreversible blindness if left untreated | ||
*Unclear pathogenesis, however thought to be related to two mechanisms: | *Unclear pathogenesis, however thought to be related to two mechanisms: | ||
Revision as of 21:49, 4 February 2026
Background
- Elevated intraocular pressure and resulting optic nerve damage manifested initially as visual field loss and ultimately irreversible blindness if left untreated
- Unclear pathogenesis, however thought to be related to two mechanisms:
- Increased aqueous production
- Decreased outflow
Clinical Features
- Rarely experience symptoms, in contrast to acute angle closure glaucoma
- Typical pattern characterized by progressive peripheral visual field loss followed by central field loss, usually but not always associated with elevated intraocular pressure
Differential Diagnosis
Acute Vision Loss (Noninflamed)
- Painful
- Arteritic anterior ischemic optic neuropathy
- Optic neuritis
- Temporal arteritis†
- Painless
- Amaurosis fugax
- Central retinal artery occlusion (CRAO)†
- Central retinal vein occlusion (CRVO)†
- High altitude retinopathy
- Open-angle glaucoma
- Posterior reversible encephalopathy syndrome (PRES)
- Retinal detachment†
- Stroke†
- Vitreous hemorrhage
- Traumatic optic neuropathy (although may have pain from the trauma)
†Emergent Diagnosis
Evaluation
Workup
Diagnosis
- Characteristic nerve damage (eg, cupping) on fundus examination
- Visual field abnormalities
- +/- elevated IOP