Purple urine bag syndrome: Difference between revisions
(Strip excess bold) |
|||
| (One intermediate revision by one other user not shown) | |||
| Line 6: | Line 6: | ||
===Pathophysiology=== | ===Pathophysiology=== | ||
* | *Mechanism: | ||
**Dietary Tryptophan is metabolized by gut bacteria into Indole | **Dietary Tryptophan is metabolized by gut bacteria into Indole | ||
**Indole is absorbed and converted to Indoxyl sulfate in the liver | **Indole is absorbed and converted to Indoxyl sulfate in the liver | ||
**Indoxyl sulfate is excreted into urine | **Indoxyl sulfate is excreted into urine | ||
**Bacteria producing | **Bacteria producing indoxyl sulfatase or phosphatase catalyse the breakdown of indoxyl sulfate into: | ||
*** | ***Indigo (Blue pigment) | ||
*** | ***Indirubin (Red pigment) | ||
** pigments interact with the polyvinyl chloride (PVC) of the catheter bag to create a | ** pigments interact with the polyvinyl chloride (PVC) of the catheter bag to create a | ||
* | *Risk Factors: | ||
**Chronic Indwelling Catheter (PVC material) | **Chronic Indwelling Catheter (PVC material) | ||
**[[Constipation]] (Prolonged gut transit increases bacterial deamination of tryptophan) | **[[Constipation]] (Prolonged gut transit increases bacterial deamination of tryptophan) | ||
| Line 37: | Line 37: | ||
==Differential Diagnosis== | ==Differential Diagnosis== | ||
*[[Rhabdomyolysis]] (Tea-colored) | *[[Rhabdomyolysis]] (Tea-colored) | ||
*[[Porphyria]] (Port-wine colored) | *[[Porphyria]] (Port-wine colored) | ||
| Line 50: | Line 49: | ||
==Evaluation== | ==Evaluation== | ||
*[[Urinalysis]] | *[[Urinalysis]] | ||
**Typically | **Typically Alkaline pH (> 7.0) | ||
**Pyuria/Leukocyte esterase positive | **Pyuria/Leukocyte esterase positive | ||
*[[Urine Culture]] | *[[Urine Culture]] | ||
| Line 60: | Line 59: | ||
==Management== | ==Management== | ||
* | *Reassurance | ||
**Explain the benign chemical nature of the discoloration to patient/caregivers | **Explain the benign chemical nature of the discoloration to patient/caregivers | ||
*Source Control | *Source Control | ||
| Line 67: | Line 66: | ||
*Antibiotics | *Antibiotics | ||
**Based on clinical status: | **Based on clinical status: | ||
*** | ***Asymptomatic Bacteriuria: Antibiotics generally ''not'' indicated solely for purple bag; focus on hygiene/catheter exchange | ||
*** | ***Symptomatic CAUTI/Sepsis: Empiric broad-spectrum coverage covering Gram-negatives (e.g., [[Cefepime]], [[Piperacillin-Tazobactam]]) until sensitivities return | ||
**Note: Many causative organisms (Example: ''Providencia'', ''Morganella'') have intrinsic resistance to common agents like Nitrofurantoin or Colistin | **Note: Many causative organisms (Example: ''Providencia'', ''Morganella'') have intrinsic resistance to common agents like Nitrofurantoin or Colistin | ||
Latest revision as of 09:37, 22 March 2026
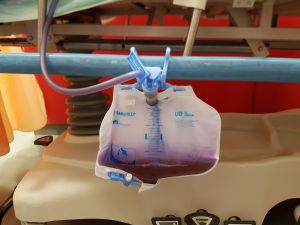
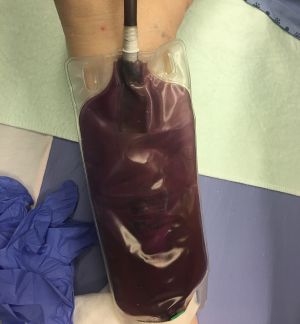
Background
- Rare phenomenon characterized by purple discoloration of the urinary drainage bag and tubing
- Benign reaction in itself, but indicates high bacterial load and Catheter-associated urinary tract infection
- Predominantly affects chronically catheterized, constipated, elderly females (often in nursing homes)
- Caused by specific Gram-negative bacteria producing sulphatase and phosphatase enzymes[ncbi.nlm.nih.gov]
Pathophysiology
- Mechanism:
- Dietary Tryptophan is metabolized by gut bacteria into Indole
- Indole is absorbed and converted to Indoxyl sulfate in the liver
- Indoxyl sulfate is excreted into urine
- Bacteria producing indoxyl sulfatase or phosphatase catalyse the breakdown of indoxyl sulfate into:
- Indigo (Blue pigment)
- Indirubin (Red pigment)
- pigments interact with the polyvinyl chloride (PVC) of the catheter bag to create a
- Risk Factors:
- Chronic Indwelling Catheter (PVC material)
- Constipation (Prolonged gut transit increases bacterial deamination of tryptophan)
- Alkaline Urine (Favors pigment precipitation)
- High bacterial load
- Female gender (shorter urethra, higher UTI risk)
Clinical Features
- Altered Mental Status (if associated with symptomatic UTI/Sepsis)
- Visual alarm (Patient/family/staff often distressed by bright purple color)
- Otherwise usually asymptomatic regarding the discoloration itself
- Common causative organisms (Sulfatase/Phosphatase producers):
Differential Diagnosis
- Rhabdomyolysis (Tea-colored)
- Porphyria (Port-wine colored)
- Medication/Dietary inputs:
- Methylene blue
- Rifampicin (Orange/Red)
- Beets/Blackberries
- Phenolphthalein (laxatives)
Red or Purple Urine
- Hematuria
- Hemoglobinuria
- Porphyria
- Myoglobinuria (rhabdomyolysis)
- Foods
- Blackberries
- Beets
- Blackberries
- Rhubarb
- Food coloring
- Fava beans
- Drugs
- Purple urine bag syndrome
- Uric acid crystalluria (neonates)
Evaluation
- Urinalysis
- Typically Alkaline pH (> 7.0)
- Pyuria/Leukocyte esterase positive
- Urine Culture
- Mandatory to guide susceptibility (high resistance rates in this population)
- Renal function
- Check for AKI/Dehydration
- Evaluate for Sepsis
- Hypothermia/Fever, Hypotension, Tachycardia
Management
- Reassurance
- Explain the benign chemical nature of the discoloration to patient/caregivers
- Source Control
- Exchange the urinary catheter (mandatory to remove biofilm and stained plastic)
- Crucial to reduce gut production of indole
- Antibiotics
- Based on clinical status:
- Asymptomatic Bacteriuria: Antibiotics generally not indicated solely for purple bag; focus on hygiene/catheter exchange
- Symptomatic CAUTI/Sepsis: Empiric broad-spectrum coverage covering Gram-negatives (e.g., Cefepime, Piperacillin-Tazobactam) until sensitivities return
- Note: Many causative organisms (Example: Providencia, Morganella) have intrinsic resistance to common agents like Nitrofurantoin or Colistin
- Based on clinical status: